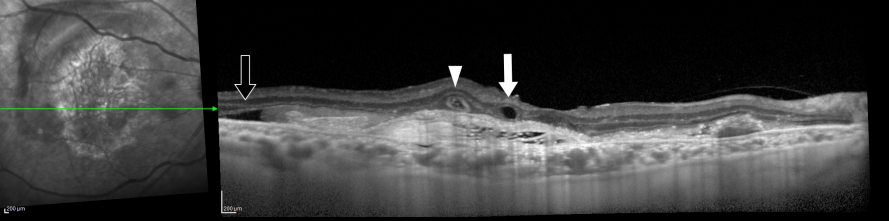
Outer Retinal Tubulation
All content on Eyewiki is protected by copyright law and the Terms of Service. This content may not be reproduced, copied, or put into any artificial intelligence program, including large language and generative AI models, without permission from the Academy.
Disease Entity
Outer retinal tubulation (ORT) is a feature of photoreceptor rearrangement after retinal injury.[1][2] Degenerating photoreceptors are arranged in a circular or tubular fashion. ORT is most commonly seen in neovascular age-related macular degeneration (AMD) but is also seen in various chronic degenerative retinal disorders.[1] This process is not disease specific but a general response to various outer retinal degenerative diseases, such as, non-exudative and exudative age-related macular degeneration, retinal dystrophies, choroideremia, angioid streaks, myopic neovascularization, multifocal choroiditis, pseudoxanthoma elasticum, central serous choroidopathy and gyrate atrophy. [3] It is important to recognize this entity since the ovoid cystic lesions can be misinterpreted to be intraretinal fluid prompting initiation of unnecessary treatment.
With spectral-domain optical coherence tomography (SD-OCT), ORT has the distinctive feature of round or ovoid hyporeflective spaces with hyperreflective borders located in the outer nuclear layer (Figure 1).[1] En face OCT shows that ORT has a branching network.[4]
The adaptive optics scanning laser ophthalmoscope (AOSLO) imaging shows ORTs as hyporeflective areas that range in length from small tubes to as long as the width of atrophy.
Risk Factors
In a retrospective study of 238 eyes of 119 patients, geographic atrophy and subretinal hyperreflective material were baseline risk factors for development of ORT.[5]
Pathogenesis
The exact pathogenesis is unknown. It is postulated that after retinal injury, degenerating photoreceptors lose adhesions to surrounding structures; the remaining viable photoreceptors reorganize by inward folding of the photoreceptor layer to form tubular structure.[1]It is postulated that this tubular arrangement may be provide some survival benefit for the photoreceptors located over diseased or atrophic retinal pigmented epithelium.
Recently the evolution of ORT has been described in 4 phases as nascent, mature, degenerate, and end stage depending on the contents within the tubule walls. The SD-OCT showed changes in the ELM in areas adjacent to geographic atrophy.[6][7]
Pathology
Histological and transmission electron microscopy suggest the hyperreflective border of ORT consists of external limiting membrane and photoreceptor inner segment mitochondria.[8] As nicely stated by Dolz-Marco, "The main histologic characteristics of ORT include: (1) location at the level of the outer nuclear layer, (2) presence of an ELM delimiting all or part of the lumen, (3) presence of surrounding radially oriented photoreceptors pointing into the lumen, and (4) degeneration or absence of the underlying RPE. ORTs are commonly found at the border of relatively normal and atrophic outer retina. These can change but may remain relatively stable over a period of time.
Causes
ORT has been seen in a variety of retinal disorders:
- Neovascular AMD[1][9]
- Pseudoxanthoma elasticum with angioid streak[1][10]
- Choroidal neovascularization secondary to multifocal choroiditis and panuveitis[1]
- Advanced AMD with geographic atrophy[1]
- Chronic central serous chorioretinopathy[1]
- Bietti crystalline dystrophy[1][11]
- Pattern dystrophy[1][11]
- Acute zonal occult outer retinopathy[11]
- Retinitis pigmentosa[11][12]
- Stargardt disease[11][12]
- Gyrate atrophy[11]
- Choroideremia[1][11]
- Best disease[12]
- Diabetic macular edema[13][3]
- Chronic retinal detachment[14]
Incidence
The incidence of ORT increases with time in neovascular AMD. One study showed that ORT developed in 17%, 28%, 35% and 41% of eyes after 1, 2, 3 and 4 years of follow up.[15] Another study showed that ORT occurred in 7%, 18% and 31% of eyes after 1, 2 and 3 years, respectively, of follow up.[16]
Clinical Implications
In neovascular AMD treated with anti-VEGF injections, eyes with ORTs had worse visual acuity[9][17], central macular thickness[9] and retinal sensitivity[9] than those without ORT. In addition, eyes with ORT had a slower rate of enlargement of geographic atrophy than those without ORT.[18]
Diagnosis
Differential Diagnoses
The major differential diagnoses are: cystoid macular edema, intraretinal fluid and subretinal fluid.[1] In contrast to cystoid macular edema, ORT has a distinctive hyperreflective border and is located within the outer retina.[11]
Treatment
ORT generally remains stable over time.[1] No treatment is required if seen in patients with neovascular AMD since it indicates inactive disease. However, presence of ORTs in CSR patients, may indicate activity of the disease which may need some treatment. [19]ORT also can be noted with RPE atrophy. It is important to recognize ORT and differentiate it from cystoid macular edema, intraretinal or subretinal fluid to avoid unnecessary invasive treatments (Figure 1).[1]
References
- ↑ Jump up to: 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 1.12 1.13 1.14 Zweifel SA, Engelbert M, Laud K, Margolis R, Spaide RF, Freund KB. Outer retinal tubulation: a novel optical coherence tomography finding. Arch Ophthalmol 2009;127(12):1596-602.
- ↑ Jung JJ, Freund KB. Long-term follow-up of outer retinal tubulation documented by eye-tracked and en face spectral-domain optical coherence tomography. Arch Ophthalmol 2012;130(12):1618-9.
- ↑ Jump up to: 3.0 3.1 Huang XL, Song YP, Ding Q, Chen X, Hong L. Evaluation of outer retinal tubulations in diabetic macular edema underwent anti-VEGF treatment. Int J Ophthalmol. 2019 Mar 18;12(3):442-450.
- ↑ Wolff B, Matet A, Vasseur V, Sahel JA, Mauget-Faysse M. En Face OCT Imaging for the Diagnosis of Outer Retinal Tubulations in Age-Related Macular Degeneration. J Ophthalmol 2012;2012:542417.
- ↑ Preti RC, Govetto A, Filho RGA, Cabral Zacharias L, Gianotti Pimentel S, Takahashi WY, Monteiro MLR, Hubschman JP, Sarraf D. OPTICAL COHERENCE TOMOGRAPHY ANALYSIS OF OUTER RETINAL TUBULATIONS: Sequential Evolution and Pathophysiological Insights. Retina. 2018 Aug;38(8):1518-1525.
- ↑ Dolz-Marco R, Litts KM, Tan ACS, Freund KB, Curcio CA. The Evolution of Outer Retinal Tubulation, a Neurodegeneration and Gliosis Prominent in Macular Diseases. Ophthalmology. 2017 Sep;124(9):1353-1367.
- ↑ Schaal, K. B., Freund, K. B., Litts, K. M., Zhang, Y., Messinger, J. D., & Curcio, C. A. (2015). Outer Retinal Tubulation In Advanced Age-Related Macular Degeneration: Optical Coherence Tomographic Findings Correspond to Histology. Retina, 35(7), 1339-1350.
- ↑ Litts KM, Messinger JD, Dellatorre K, Yannuzzi LA, Freund KB, Curcio CA. Clinicopathological correlation of outer retinal tubulation in age-related macular degeneration. JAMA Ophthalmol 2015;133(5):609-12
- ↑ Jump up to: 9.0 9.1 9.2 9.3 Iaculli C, Barone A, Scudieri M, Giovanna Palumbo M, Delle Noci N. Outer Retinal Tubulation: Characteristics in Patients With Neovascular Age-Related Macular Degeneration. Retina 2015;35(10):1979-84.
- ↑ Ellabban AA, Hangai M, Yamashiro K, Nakagawa S, Tsujikawa A, Yoshimura N. Tomographic fundus features in pseudoxanthoma elasticum: comparison with neovascular age-related macular degeneration in Japanese patients. Eye (Lond) 2012;26(8):1086-94.
- ↑ Jump up to: 11.0 11.1 11.2 11.3 11.4 11.5 11.6 11.7 Goldberg NR, Greenberg JP, Laud K, Tsang S, Freund KB. Outer retinal tubulation in degenerative retinal disorders. Retina 2013;33(9):1871-6.
- ↑ Jump up to: 12.0 12.1 12.2 Braimah IZ, Dumpala S, Chhablani J. Outer retinal tubulation in retinal dystrophies. Retina 2017;37(3):578-84.
- ↑ Al-Halafi AM. Outer retinal tubulation in diabetic macular edema following anti-VEGF treatment. Eye Vis (Lond) 2015;2:9.
- ↑ Dolz-Marco R, Cooney MJ, Engelbert M. Outer Retinal Tubulation Associated With Chronic Retinal Detachment. Retina 2017;37(11):e128-e9.
- ↑ Dirani A, Gianniou C, Marchionno L, Decugis D, Mantel I. Incidence of outer retinal tubulation in ranibizumab-treated age-related macular degeneration. Retina 2015;35(6):1166-72.
- ↑ Takagi S, Mandai M, Miyamoto N, Nishida A, Hirami Y, Uyama H, et al. Incidence of outer retinal tubulation in eyes with choroidal neovascularization under intravitreal anti-vascular endothelial growth factor therapy in a Japanese population. Clin Ophthalmol 2017;11:1219-25.
- ↑ Lee JY, Folgar FA, Maguire MG, Ying GS, Toth CA, Martin DF, et al. Outer retinal tubulation in the comparison of age-related macular degeneration treatments trials (CATT). Ophthalmology 2014;121(12):2423-31.
- ↑ Hariri A, Nittala MG, Sadda SR. Outer retinal tubulation as a predictor of the enlargement amount of geographic atrophy in age-related macular degeneration. Ophthalmology 2015;122(2):407-13.
- ↑ Mandadi SKR, Iovino C, Sacconi R, Querques G, Peiretti E, Singh SR, Chhablani J. Outer retinal tubulations in central serous chorioretinopathy associated with choroidal neovascularisation. Eur J Ophthalmol. 2021 May;31(3):1225-1230.