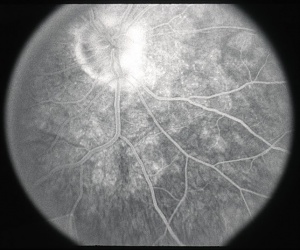
Idiopathic Multifocal Choroiditis
All content on Eyewiki is protected by copyright law and the Terms of Service. This content may not be reproduced, copied, or put into any artificial intelligence program, including large language and generative AI models, without permission from the Academy.
Disease Entity
Idiopathic multifocal choroiditis (IMFC) is a spontaneously occurring inflammatory condition presenting with multiple lesions in the retinal and choroidal tissue. IMCP causes episodes of inflammation that can occur bilaterally, simultaneously or separately. In the past, this disease was described with other names such as punctate inner choroidopathy, multifocal choroiditis with panuveitis, and progressive subretinal fibrosis and uveitis syndrome.[1] However, IMFC is a unique disease from these other disease processes.
History
In 1984 Deutsch and Tessler described 28 “pseudo- POHS” cases with uveitis including lesions of the retinal pigment epithelium and choriocapillaris.[2] This term was coined because the lesions were comparable to the ones present in patients with presumed ocular histoplasmosis syndrome. In 1986, Morgan and Shatz reported 11 cases of a condition called “recurrent multifocal choroiditis”. Described patients had concomitant vitreous inflammation which was not seen with patients with POHS. [1][2][3]
Etiology
The etiology of idiopathic multifocal choroiditis is unknown. It is hypothesized that a preceding infection may stimulate the immune response observed in multifocal choroiditis.[2] IMFC can resemble other uveitic conditions associated with systemic, infectious, or malignant underlying disease, so it is crucial to approach these patients with a broad differential. The choice of clinical therapy is contingent on making an accurate diagnosis.
Risk Factors
Idiopathic multifocal choroiditis is seen more often in white female patients with the average age at presentation of 30-years-old; however, it has been reported in an age range of 6-69 years.[3] Most patients who develop IMFC are myopic and ocular involvement is typically bilateral. IMFC predominantly affects healthy patients with no known systemic or ocular disease.[2]
General Pathology
Idiopathic multifocal choroiditis is a chronic and progressive bilateral inflammatory disease that may be associated with choroidal neovascularization and chorioretinal atrophy.[4] The commonly affected sites are the retinal pigment epithelium (RPE), outer retinal spaces, choriocapillaris, and, less commonly, the choroidal stroma. [5]
Chorioretinal lesions present are scattered throughout the posterior pole and peripheral retina. Mild to moderate anterior chamber cell reaction can be seen. Vitritis is typically seen in one or both eyes and essentially rules out POHS as a diagnosis. [2]
Multifocal choroiditis lesions are categorized into four types: active inflammatory lesions, inactive inflammatory lesions, secondary active choroidal neovascularization, and secondary inactive choroidal neovascularization. In the past, clinicians decided which stage the MFC lesions were based on changes in visual acuity, vitreous inflammatory cells and focal pigmentation.[4] However, this unstandardized approach was not accurate enough to guide therapy.
Pathophysiology
Idiopathic MFC was shown to be associated with interleukin-10 and tumor necrosis factor haplotypes. However, the exact mechanism of IMFC is still widely unknown. [5] It is hypothesized that a preceding infection is responsible for stimulating the immune response that is observed in IMFC. Inflammatory lesions initiate from the level of the retinal pigment epithelium and choroidal capillaries. Some hypothesize that antigens become sensitized in the retinal photoreceptors and RPE by a foreign pathogen. These inflammatory lesions can then jeopardize the integrity of Bruch’s membrane, the innermost layer of the choroid. [6] This allows room for a choroidal neovascular membrane to develop, which may occur in up to 60% of patients.[4]
Primary Prevention
There is no recommended prevention at this time, as no specific etiology is currently associated with the disease processes.
Diagnosis
Idiopathic multifocal choroiditis is a clinical diagnosis. The differential diagnosis of MFC is extensive. It is important to rule out similar appearing ocular pathology, especially infectious, malignant, and systemic processes, as IMFC is a diagnosis of exclusion.[7]
Physical Examination
On visual field testing scotoma may be present. Slit-lamp exam reveals intraocular inflammation and anterior or vitreous cell.[2] Retinal evaluation also reveals yellow to gray lesions, located at the level of retinal pigment epithelium and choriocapillaris. The size of the lesions range between 45-350 µm.[8] Lesions are scattered throughout the retina, in clusters, or in a linear fashion. During active disease, exam may also reveal subretinal fluid, optic nerve swelling and hyperemia, cystoid macular edema, atrophic, punched-out discolored retinal pigment epithelial lesions, or choroidal neovascularization. During the acute phase, choroidal neovascularization may occur which is the most severe complication of the disease. Cystoid macular edema also develops in 14%-41% of affected eyes. Other complications of IMFC include glaucoma, optic nerve atrophy, macular atrophy, vitritis, and progressive subretinal scars.[6]
Signs & Symptoms [2][5][8]
- Eye discomfort
- Scotoma
- Blurry Vision
- Vision Loss
- Photophobia
- Photopsias
- Metamorphopsia
- Floaters
Diagnostic procedures
Retinal imaging is useful in determining lesion types. The use of multiple imaging modalities in diagnosis is recommended. [4]
Color Fundus Photography
Active lesions present as yellow-white lesions. The boundaries of the lesions can be blurred due to retinal edema. Occasionally, punctate hemorrhaging can also be visualized.[5] Inactive lesions are usually gray and the boundaries of lesions are more defined. However, scar fibrosis and pigmentation are usually present on these lesions. [4]
Fluorescein Fundus Angiography
Acute inflammatory lesions exhibit minimal early hyperfluorescence and late hyperfluorescence, staining.[4] Late staining may indicate the presence of an active CNV.
Optical Coherence Tomography
Active lesions show RPE elevation due to deposition of material in the sub RPE space. On EDI-OCT choroidal thickness can be seen beneath the active lesions. [5] The presences of subretinal or sub-RPE material with associated fluid suggests CNV. [6]
Indocyanine Green Angiography
Acute inflammatory lesions will typically present with subtle early hypofluorescence that become more pronounced in late study. Active CNV present with late hyperfluorescence.[9]
Fundus Autofluorescence
Fundus Autofluorescence (FAF) imaging demonstrates diffuse hyper-autofluorescent lesions in the peripapillary and posterior pole with late staining of the optic nerve. As the inflammation subsides, FAF may display hypoautofluorescent atrophic lesions. [10]
Electroretinogram
Displays a wide range of results, some patients have normal ERG findings, and others may show reduced a and b wave amplitudes.
Differential diagnosis
The differential diagnosis for multifocal choroiditis includes a wide range of inflammatory and infectious processes. It is crucial to approach these patients with careful observation and detailed history taking to help guide diagnostic testing.
Infectious
- Presumed Ocular Histoplasmosis Syndrome
- Syphilis
- Tuberculosis
- Toxoplasmosis
- West Nile Virus
- Pneumocystis Choroiditis
Non-Infectious
- Sarcoidosis
- Punctate Inner Choroidopathy
- Birdshot Retinochoroidopathy
- Acute Posterior Multifocal Placoid Pigment Epitheliopathy
Malignant
- Lymphoma
- Metastasis
Due to the wide range of possibilities of other pathological processes that can mimic MFC clinically, an initial laboratory work-up should be performed in patients presenting with a multifocal choroiditis-like clinical picture. With the use of proper clinical reasoning, laboratory tests and further diagnostic tests should be done to aid in the diagnosis. These tests include but are not limited to CBC, CMP, angiotensin-converting enzyme, chest X-ray, syphilis testing, and QuantiFERON-TB gold.[6][11]
Management
After the diagnosis of IMFC is made, treatment is tailored based on the extent of inflammation, development of active inflammatory lesions, and complications and decreased visual acuity. The development of cystoid macular edema, dense vitritis, or choroidal neovascular membrane is an indication for treatment. [2]
Medical therapy
Management revolves around mitigating the inflammatory process and choroidal neovascularization. The severity of the disease guides the treatment of choice; however, typically corticosteroids or other immunosuppressive agents are used. Oral corticosteroids are often the first line for treatment. They are typically started at a high to moderate dose and then tapered down as the inflammation recedes. Periocular or intraocular corticosteroid injections or implants are sometimes used as local anti-inflammatory therapy.[6] Triamcinolone acetonide (Kenalog) has a duration of action for two to three months.[12]
Ozurdex (dexamethasone) is an intravitreal injection indicated for non-infectious uveitis affecting the posterior segment. The duration of action is usually three to four months. Tonometry should be done within 30 minutes of injection and biomicroscopy between 2-7 days. Iluvien, an injection that contains a micro implant with fluocinolone acetonide, is another treatment modality used for IMFC. It is designed to release continuous low dose corticosteroid for up to three years.[12][13]
With the mentioned corticosteroids, it is crucial to monitor for elevation in intraocular pressure, cataract development, and endophthalmitis. Close to 35% of patients who use intraocular steroids have a worrisome rise in IOP. [12] Other complications include ptosis and cataracts.
In severe and refractory cases, immunomodulator drugs such as antimetabolites, biologics, and T-cell inhibitors should be considered for treatment. [14]
Intravitreal anti-VEGF therapy is used to treat choroidal neovascularization and macular edema.
Prognosis
The prognosis of multifocal choroiditis varies. Most patients with IMFC have excellent visual prognosis. However, symptoms and findings can reoccur. Poor visual prognosis is predicated by scarring and the development of CNVM. [6][9]
References
- ↑ Jump up to: 1.0 1.1 Essex, Rohan W., et al. “Idiopathic Multifocal Choroiditis.” Retina, vol. 33, no. 1, 2013, pp. 1–4., doi:10.1097/iae.0b013e3182641860.
- ↑ Jump up to: 2.0 2.1 2.2 2.3 2.4 2.5 2.6 2.7 Goldstein, Debra, and Larry Ulanski. “Multifocal Choroiditis vs. PIC: Variations on a Theme?” Review of Ophthalmology, 2004.
- ↑ Jump up to: 3.0 3.1 Pinar, Vakur, and Stephen Foster. “Bilateral Chorioretinal Lesions Appearing Late in Posterior Uveitis.” 2000.
- ↑ Jump up to: 4.0 4.1 4.2 4.3 4.4 4.5 Dolz-Marco, Rosa, et al. “How to Differentiate Myopic Choroidal Neovascularization, Idiopathic Multifocal Choroiditis, and Punctate Inner Choroidopathy Using Clinical and Multimodal Imaging Findings.” Ophthalmic Surgery, Lasers and Imaging Retina, SLACK Incorporated, 16 Mar. 2017,
- ↑ Jump up to: 5.0 5.1 5.2 5.3 5.4 Li, J., Li, Y., Li, H. et al. Imageology features of different types of multifocal choroiditis. BMC Ophthalmol 19, 39 (2019). https://doi-org.ezproxy.med.ucf.edu/10.1186/s12886-019-1045-x
- ↑ Jump up to: 6.0 6.1 6.2 6.3 6.4 6.5 6.6 Tavallali, Ali, and Lawrence A. Yannuzzi. “Idiopathic Multifocal Choroiditis.” Journal of Ophthalmic and Vision Research, vol. 11, no. 4, 2016, p. 429., doi:10.4103/2008-322x.194141.
- ↑ Crawford, Courtney M., and Okezie Igboeli. “A Review of the Inflammatory Chorioretinopathies: The White Dot Syndromes.” ISRN Inflammation, vol. 2013, 2013, pp. 1–9., doi:10.1155/2013/783190.
- ↑ Jump up to: 8.0 8.1 Dingerkus, V.L.S., Munk, M.R., Brinkmann, M.P. et al. Optical coherence tomography angiography (OCTA) as a new diagnostic tool in uveitis. J Ophthal Inflamm Infect 9, 10 (2019). https://doi.org/10.1186/s12348-019-0176-9
- ↑ Jump up to: 9.0 9.1 Slakter JS, Giovannini A, Yannuzzi LA, et al. Indocyanine green angiography of multifocal choroiditis. Ophthalmology. 1997;104(11):1813–1819. doi:10.1016/s0161-6420(97)30022-0
- ↑ Kramer M, Priel E. Fundus autofluorescence imaging in multifocal choroiditis: beyond the spots. Ocul Immunol Inflamm. 2014;22(5):349–355. doi:10.3109/09273948.2013.855797
- ↑ Jump up to: 11.0 11.1 Ongchin, Sharel, et al. “A Diagnostic Dilemma: Infectious versus Noninfectious Multifocal Choroiditis with Panuveitis.” Journal of Ophthalmic Inflammation and Infection, vol. 3, no. 1, 2013, p. 26., doi:10.1186/1869-5760-3-26.
- ↑ Jump up to: 12.0 12.1 12.2 Albini, Thomas, and Justin Yamanuha. “Current and New Steroid Therapy in Noninfectious Uveitis.” Retina Specialist, 2019.
- ↑ Pasadhika, Sirichai, et al. “Biologic Therapy for Posterior Uveitis and Panuveitis.” Medical Retina, 2012.
- ↑ Fellman, Ronald L. “Steroids for Glaucoma: Both Friend and Foe.” Review of Ophthalmology, 8 Sept. 2015, www.reviewofophthalmology.com/article/steroids-for-glaucoma--both-friend-and-foe.