Cicatricial Conjunctivitis
All content on Eyewiki is protected by copyright law and the Terms of Service. This content may not be reproduced, copied, or put into any artificial intelligence program, including large language and generative AI models, without permission from the Academy.
Disease Entity
Definition
Cicatrizing Conjunctivitis refers to a vision-threatening family of rare disorders characterized by inflammation and resultant scarring of the conjunctiva.[1]
Etiology
Cicatrizing conjunctivitis can be caused by trauma, medication, infection, systemic bullous pathologies, autoimmune conditions, and conjunctival diseases [2].
A history of severe conjunctivitis, chemical injury, Stevens-Johnson Syndrome (SJS)/Toxic Epidermal Necrolysis (TEN), and chronic use of ophthalmic solutions for glaucoma have been associated with conjunctival scarring consistent with non-progressive cicatrizing conjunctivitis.[3]
Autoimmune etiologies including ocular rosacea with meibomian gland disease, atopic disease, and most commonly, ocular cicatricial pemphigoid (OCP), part of the mucous membrane pemphigoid (MMP) spectrum of disorders,[4] have been implicated in active, progressive cicatrizing conjunctivitis. Cases of cicatrizing conjunctivitis secondary to systemic inflammatory conditions such as Sjogren’s syndrome, granulomatosis with polyangiitis (GPA), and sarcoidosis have also been reported.[3] Additionally, trachoma and paraneoplastic cases have been linked to the development of cicatrizing conjunctivitis.[3]
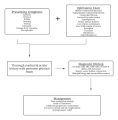
The provider should be vigilant in eliciting a thorough history to better ascertain whether these findings of cicatrizing conjunctivitis reflect an active disease process. This determination, in addition to identifying the specific etiology of cicatrizing conjunctivitis, will allow the ophthalmologist to optimally guide management.
Table 1 - Possible Etiologies of Cicatricial Conjunctivitis[1][2][3][4][5]
| Autoimmune Conditions | Conjunctival Diseases | Infections | Malignancies | Medications | Systemic Inflammatory Pathologies | Trauma | Other |
|---|---|---|---|---|---|---|---|
| Bullous pemphigoid | Atopic keratoconjunctivitis | Adenoviral keratoconjunctivitis | Intraepithelial epithelioma | Systemic practolol | Amyloidosis | Carotid-cavernous fistula | Congenital ichthyosiform erythroderma |
| Dermatitis herpetiformis | Ligneous conjunctivitis | Chronic mucocutaneous candidiasis | Mucosa-associated lymphoid tissue lymphoma | Systemic D-penicillamine | Prophyria cutanea tarda | Chemical injury | |
| Discoid lupus | Corynebacterium diphtheriae conjunctivitis | Sebaceous cell carcinoma | Topical epinephrine | Stevens-Johnson Syndrome/Toxic Epidermal Necrolysis (SJS/TEN) | Mechanical injury | ||
| Epidermolysis bullosa acquisita | Herpes simplex conjunctivitis | Squamous cell carcinoma | Topical glaucoma medications, notably pilocarpine and echothiophate iodide | Radiation injury | |||
| Graft-versus-host disease (GVHD) | Streptococcal conjunctivitis | Topical idoxuridine | Surgical injury | ||||
| Granulomatosis with polyangiitis (GPA) | Trachoma | Self-induced cicatricial conjunctivitis | |||||
| Lichen planus | Thermal injury | ||||||
| Linear IgA disease | |||||||
| Lupus erythematosus | |||||||
| Ocular cicatricial pemphigoid (OCP) | |||||||
| Ocular rosacea | |||||||
| Paraneoplastic pemphigus | |||||||
| Pemphigus vulgaris | |||||||
| Progressive systemic sclerosis | |||||||
| Sarcoidosis | |||||||
| Sjogren’s syndrome | |||||||
| Stevens- Johnson syndrome |
Pathophysiology
As mentioned above, a spectrum of disease conditions can lead to cicatrizing conjunctivitis including autoimmune diseases, atopy, chemical burns, infectious causes, and malignancies.[3][4][5] For this reason, the exact pathogenic mechanism of each case of cicatrizing conjunctivitis will depend on its specific etiology. Generally speaking, chronic inflammation of the conjunctiva leads to an inflammatory infiltrate, composed of macrophages and other monocytes. These cells release growth factors that stimulate fibroblasts and extracellular matrix formation, leading to eventual fibrosis of the conjunctiva [5] and alterations of the ocular surface.[4]
The pathologic process of OCP, the most common autoimmune cause of cicatrizing conjunctivitis, is mediated by genetic susceptibility[4] for autoantibody formation against basement membrane glycoproteins of mucosal membranes, including the conjunctiva, esophagus, and larynx.[3] This is followed by activation of the complement pathway and subsequent recruitment of inflammatory cells that leads to a chronic inflammation and fibrosis.[5]
Epidemiology
Epidemiological data of cicatrizing conjunctivitis remains limited, with two surveillance studies, one from the United Kingdom and one from New Zealand and Australia, reporting an annual incidence of 1.3 per million[6] and 1.5 per million, respectively.[7]
Diagnosis
Clinical Presentation
Patients may present in a variety of ways, depending on the severity of the disease process and the multitude of potential etiologies responsible for it. Symptoms include chronic conjunctival injection, dryness, itching, irritation, burning, tearing, discharge, foreign body sensation, and photophobia.[3][4] These symptoms will typically be refractory to dry eye treatment.[3]
Ophthalmic Exam and Findings
Thorough examination of the entire anterior segment and ocular adnexal structures is critical for recognition of the clinical features present in the early stages of this disease.[3] The following are ophthalmic exam findings associated with cicatrizing conjunctivitis:
- Diffuse conjunctival injection.[3]
- Subepithelial fibrosis of the palpebral conjunctiva (upper and lower eyelids) that forms one to two millimeters from the lid margin. It has been described as “fine interweaving strands with a white glistening appearance running parallel to the lid margin”.[3]
- Caruncular fibrosis has also been reported as an early and subtle sign.[1]
- With lower eyelid retraction and eye in upward gaze, forniceal foreshortening is evidenced by incomplete visualization of the fornix even with downward traction of the lower lid.[3]
- Severe and advanced cicatrizing conjunctivitis presents with symblepharon formation, ocular surface dryness, keratin deposits, and dermalization, loss of plica semilunaris, loss of lid margin structure and mucocutaneous junction, entropion, trichiasis, distichiasis, and ankyloblepharon.[1]
Additional Diagnostic Procedures
As mentioned above, questioning should include any history of ocular injuries, ocular infections, and past or present medications.[4] Pertinent review of systems and physical examination of the mucosa, skin, and joints should also be conducted for known systemic inflammatory and autoimmune conditions that provoke cicatrizing conjunctivitis. A few salient examples will be reviewed:
- In the case of OCP, history and physical examination should investigate mucous membrane involvement in the form of oral, laryngeal, tracheal, or esophageal lesions,[3] some of which are potentially life-threatening. Oral mucosal involvement may manifest as desquamative gingivitis or vesicular and bullous lesions.[4] Esophageal lesions can lead to patient complaints of heartburn or dysphagia. Laryngeal and tracheal involvement can result in difficulty breathing, hoarseness, and dysphonia.[4] Though less frequently associated, cutaneous involvement in the form of erythematous plaques with vesicles and bullae should also be considered.[4]
- In the case of SJS/TEN, skin, mucosal, or ocular findings typically arise 3 weeks after exposure to an inciting drug, classically a sulfonamide, anticonvulsant, penicillin, or salicylate.[4] The diagnosis is made clinically, although a skin or mucosal biopsy with histopathologic findings of epithelial necrosis and separation of epidermis and basement membrane from the dermis can be confirmatory.[4]
Further workup includes specimen examination and serologic studies. Serologic workup includes ESR, CBC, CMP, ANA, SS-A, SS-B, ANCA, ACE, and lysozyme for evaluation of underlying granulomatosis with polyangiitis (GPA), Sjogren’s, or sarcoidosis, among others[3]. A biopsy of the lower bulbar conjunctiva[4] for histopathology (formalin) and immunofluorescence (Michel’s solution) should be collected. Evidence of granulomatous features would be more suggestive of sarcoidosis or GPA[3] while demonstration of linear immunoglobulin and/or complement deposition at the conjunctival epithelial basement membrane is supportive of a diagnosis of OCP.[3] Negative immunofluorescence results do not rule out OCP, especially as false-negative biopsies occur in a large proportion of patients.[3][4] If available, avidin-biotin complex (ABC) staining should increase sensitivity of biopsy results.[3] A second biopsy can also be considered, if possible. In the case that history, physical examination, and disease course continue to point towards OCP despite negative or equivocal biopsy results, the patient should still be offered systemic therapy.[3]
Management
As specified above, treatment will be differentially targeted at the etiology of chronic cicatricial conjunctivitis. The goals of treatment should include halting any progressive cicatrization, preventing and correcting both corneal and lid complications, and symptomatic relief.[1]
Table 2 - Diagnosis and Management of Cicatricial Conjunctivitis[1][2][3][4][5]
Treatment of OCP
OCP is a systemic disease that requires systemic treatment. Although steroids can be used as a bridge in therapy, immunomodulatory therapy (IMT) should be considered for primary treatment.[3] Because antimetabolites such as methotrexate, mycophenolate mofetil, or azathioprine are preferred, inter-specialty care with rheumatology and/or hematology is strongly recommended.[3] Treatment efficacy is monitored by tracking improvement in symptoms and conjunctival injection (via regular anterior segment photography), with remission defined as a white and quiet eye.[3] Dosage can be increased in partial responders, but 6 weeks should be allowed before assessing efficacy.[3]
Treatment of SJS/TEN
Treatment of SJS and TEN involves immediate cessation of the suspected offending agent with symptomatic treatment with careful attention to hydration, electrolyte balance, and sepsis prevention.[4]Ocular surface care during the acute phase of SJS involves maintenance of corneal epithelial integrity with preservative-free lubricants,[4] topical antibiotics, topical steroids, and possible amniotic membrane transplantation.[8]
Following resolution of skin and mucosal ulcerations and discharge from the intensive care unit, patients must continue to be monitored for chronic ocular sequelae to prevent progression to end-stage blindness.[8] Ophthalmic examination within the first month following discharge, every 2-4 months during the first year, and at least every 6 months thereafter is critical and strongly advised, as thirty to fifty percent of patients with acute SJS/TEN subsequently develop chronic ocular sequelae, including trichiasis, entropion, lid margin keratinization, corneal pannus, and persistent corneal epithelial defects.[8]
Managing these ocular manifestations within the windows of opportunity present in both acute and chronic SJS/TEN is vital to preventing vision loss.
References
- ↑ Jump up to: 1.0 1.1 1.2 1.3 1.4 1.5 Vazirani J, Donthineni PR, Goel S, Sane SS, Mahuvakar S, Narang P, et al. Chronic cicatrizing conjunctivitis: A review of the differential diagnosis and an algorithmic approach to management. Indian J Ophthalmol 2020;68:2349–55. https://doi.org/10.4103/ijo.IJO_604_20.
- ↑ Jump up to: 2.0 2.1 2.2 Kirzhner M, Jakobiec FA. Ocular Cicatricial Pemphigoid: A Review of Clinical Features, Immunopathology, Differential Diagnosis, and Current Management. Semin Ophthalmol 2011;26:270–7. https://doi.org/10.3109/08820538.2011.588660.
- ↑ Jump up to: 3.00 3.01 3.02 3.03 3.04 3.05 3.06 3.07 3.08 3.09 3.10 3.11 3.12 3.13 3.14 3.15 3.16 3.17 3.18 3.19 3.20 3.21 3.22 3.23 Swan RT, Cao J, Foster CS. Diagnosis and Management of Cicatricial Conjunctivitis. In: Djalilian AR, editor. Ocul. Surf. Dis. Case-Based Guide, Cham: Springer International Publishing; 2018, p. 171–92. https://doi.org/10.1007/978-3-319-15823-5_12.
- ↑ Jump up to: 4.00 4.01 4.02 4.03 4.04 4.05 4.06 4.07 4.08 4.09 4.10 4.11 4.12 4.13 4.14 4.15 4.16 Akpek EK, Ilhan-Sarac O. Cicatrizing Conjunctivitis. In: Foster CS, Azar DT, Dohlman CH, editors. Smolin Thofts Cornea Sci. Found. Clin. Pract., Lippincott Williams & Wilkins; 2005, p. 477–502.
- ↑ Jump up to: 5.0 5.1 5.2 5.3 5.4 Faraj HG, Hoang-Xuan T. Chronic cicatrizing conjunctivitis. Curr Opin Ophthalmol 2001;12:250–7. https://doi.org/10.1097/00055735-200108000-00003.
- ↑ Radford CF. Incidence, presenting features, and diagnosis of cicatrising conjunctivitis in the United Kingdom. Eye 2012;26:1199–208. https://doi.org/10.1038/eye.2012.119.
- ↑ Bobba S. Incidence, clinical features and diagnosis of cicatrising conjunctivitis in Australia and New Zealand. Eye 2018;32:1636–43. https://doi.org/10.1038/s41433-018-0155-7.
- ↑ Jump up to: 8.0 8.1 8.2 Kohanim S, Palioura S, Saeed HN, Akpek EK, Amescua G, Basu S, et al. Acute and Chronic Ophthalmic Involvement in Stevens-Johnson Syndrome/Toxic Epidermal Necrolysis – A Comprehensive Review and Guide to Therapy. II. Ophthalmic Disease. Ocul Surf 2016;14:168–88. https://doi.org/10.1016/j.jtos.2016.02.001.