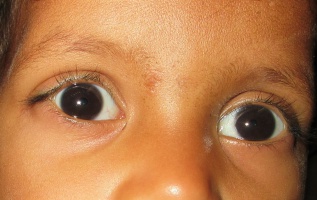
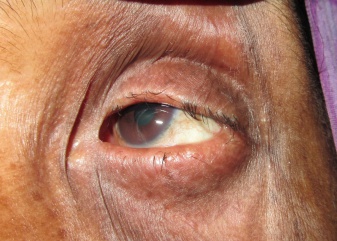
Ankyloblepharon
All content on Eyewiki is protected by copyright law and the Terms of Service. This content may not be reproduced, copied, or put into any artificial intelligence program, including large language and generative AI models, without permission from the Academy.
Disease Entity
Ankyloblepharon
- ICD9; 374.46
- ICD10; Q10.3
Disease
Ankyloblepharon is partial or complete fusion of the eyelids by webs of skin.[1] The adhesions of the edges of upper with lower eyelid may be present since birth (congenital) or may be acquired.
Types
Ankyloblepharon may be complete, partial or interrupted.[2] The interrupted form is also known as ankyloblepharon filiforme adnatum (AFA). It was first described by Von Hasner in 1881.[3] In this form, single or multiple fine epithelial bands are present between upper and lower eyelids, which decrease the palpebral fissure height and reduce excursion of eyelids.
Etiology
Congenital ankyloblepharon
During the development of eyelid structures, the epithelial fusion of the eyelid margins occur at around 9th week of gestation. The lid margins usually remain fused until about the end of the 5th fetal month. Complete separation usually does not occur until about the 7th fetal month.[4] Rarely, the lid margins may fail to separate at birth leading to ankyloblepharon. The exact etiology of this condition is unknown. The currently accepted theory is that this condition is due to temporary epithelial arrest and rapid mesenchymal proliferation, allowing union of eyelids at abnormal positions.[5] Ankyloblepharon may be an isolated sporadic malformation or may be associated with other inherited conditions. It may be associated with central nervous system and/or cardiac anomalies, ectodermal syndromes, cleft lip and/or palate, popliteal pterygium syndrome, and gastrointestinal abnormalities.[6] [7][8][9][10][11]Ankyloblepharon filiforme adanatum has been reported to be associated with infantile glaucoma and iridodysgenesis.[12]
Systemic associations
The systemic associations of congenital ankyloblepharon have been reported in following conditions:
- Hay-Wells syndrome: A rare autosomal dominant disorder characterized by ankyloblepharon, ectodermal defects, and cleft lip and palate (AEC syndrome).
- Curly hair, ankyloblepharon and nail dysplasia (CHAND) syndrome: An autosomal recessive disorder characterised by ankyloblepharon, ectodermal dysplasia, curly hair and hypoplastic nails, with absence of cleft lip or palate. It is also known as Baughman syndrome.
- Edwards’ syndrome or Trisomy 18: Edwards’ syndrome or Trisomy 18 patients may also have ankyloblepharon filiforme adnatum.
- Rapp-Hodgkin syndrome: An autosomal dominant syndrome characterised by ectodermal dysplasia, cleft lip and/or palate, and mid-facial hypoplasia.
- Popliteal pterygium syndrome: It is characterized by intercrural webbing of the lower limbs.
Acquired ankyloblepharon
Various etiologies for acquired ankyloblepharon have been described.[13][14] Ankyloblepharon may develop following:
- Trauma - Burns, chemical or physical injuries
- Cicatrizing diseases like Stevens-Johnson syndrome or cicatricial ocular pemphigoid
- Inflammatory diseases such as herpes simplex infection or ulcerative blepharitis
- Diphtheric conjunctivitis
- Trachoma
- Tarsorrhaphy - planned surgical, or unplanned
- Ankyloblepharon from cyanoacrylate glue
Diagnosis
Diagnosis of ankyloblepharon is based on clinical features.
Symptoms
Patients with ankyloblepharon may have following symptoms:
- Complete, partial or interrupted adhesions of upper and lower eyelids
- Reduced eye lid excursion
- Shortening of palpebral fissure
- Pseudoexotropia due to lateral ankyloblepharon
- Pseudoesotropia due to medial ankyloblepharon
- Downward displacement of lateral canthal angle
- Large fluid cyst due to accumulation of lacrimal tears in cases of total ankyloblepharon
- Associated congenital abnormalities like microphthalmos, anophthalmos, ptosis, cleft lip or cleft palate
Differential diagnosis
Ankyloblepharon may be differentiated from other ocular conditions like
- Blepharophimosis: It is characterized by reduced palpebral aperture and telecanthus (increased medial intercanthus distance), but the eyelid margins are normal.
- Euryblepharon: In both euryblepharon and ankyloblepharon, the lateral portion of the eyelid may be lax and displaced downward. In ankyloblepharon, the eyelid margins are fused together for some distance producing a shorter horizontal palpebral fissure but the fissure is longer than normal in cases of euryblepharon.
- Cryptophthalmos: It is a rare congenital anomaly in which the skin passes continuously over the eyeball with absence of eyelids.
- Microphthalmos: It is a congenital condition in which the affected eye is smaller than normal at birth.
- Pseudostrabismus: It is a condition where the eyes are orthotropic (without any misalignment) but appears to be misaligned.
Management
A significant central ankyloblepharon may interfere with vision and cause amblyopia in congenital variety. A medial or lateral ankyloblepharon may restrict the visual fields. A medial ankyloblepharon may obstruct the punctum. Management of ankyloblepharon is mainly surgical. Detailed systemic assessment by an experienced pediatrician is essential to rule out coexisting pathology and proper management of congenital ankyloblepharon.
Indications for surgery
Surgery is indicated to minimize any risk of occlusion amblyopia, for improvement of visual field or for cosmetic reasons.
Surgical therapy
Congenital ankyloblepharon
The surgical management of congenital ankyloblepharon depends on the type and extent of the lid margins adhesions. Fine filamentous adhesions of ankyloblepharon filiforme adnatum can resolve spontaneously.[14] Fine bands of adhesions can be broken by forcibly separating the lids or with use of muscle hook, sharp scissors or a scalpel. The fine remnants at the lid margin usually shrink and resolve.[15] Bipolar cautery forceps can be used at the bases of fine filaments to release the adhesions. More severe cases of congenital ankyloblepharon require surgery to separate and reconstruct the lid margins.
Acquired ankyloblepharon
The causative agent of the acquired ankyloblepharon need to be determined. Acquired ankyloblepharon due to trauma or inflammatory conditions may be associated with symblepharon.[16] Ankyloblepharon alone may be treated with the separation using blunt scissors. The irregularities at lid margin may be trimmed and raw surface covered. Bleeding may be stopped using light cautery. If significant symblepharon is associated with ankyloblepharon, release of symblepharon adhesion and covering with amniotic membrane or mucous membrane graft may be done. Ankyloblepharon-type adhesions from accidental or planned application of cyanoacrylate glue can be treated conservatively.[17] The glue can be peeled off the lids and lashes with forceps. If the lashes are mainly involved, they can be cut allowing the lids to open.
Prognosis
The results of ankyloblepharon surgery can be generally correlated with the extent of the ankyloblepharon. In congenital ankyloblepharon, visual prognosis is usually good if timely intervention is performed. Cosmetic appearance after separation of the bands is usually very good. In acquired ankyloblepharon the scarring process may hamper the healing process following the reconstructive surgery.
References
- ↑ Orbit, Eyelids, and Lacrimal System, Saction 7. Basic and Clinical Science Course. American Academy of Ophthalmology. 2013-2014.
- ↑ Jonathan J. Dutton, Gregg S. Gayre, Alan D. Proia. Diagnostic Atlas of Common Eyelid Diseases. CRC Press, 2007. pp. 56
- ↑ Von Hasner. Ankyloblepharon filiforme adnatum. Z Heilkd.1881; 2:429.
- ↑ Mann I. Development of the Human Eye, 3rd edition. Australia: Grune & Stratton; 1964. pp. 259-69.
- ↑ Judge H, Mott W, Gabriels J. Ankyloblepharon filiforme adnatum. Arch Ophthalmol 1929; 2: 702-8.
- ↑ Rosenman Y, Ronen S,Eidelman AI, et al. Ankyloblepharon filiforme adnatum: congenital eyelid-band syndromes. Am J Dis Child. 1980;134(8):751-3
- ↑ Akkermans CH, Stern LM. Ankyloblepharon filiforme adnatum. Br J Ophthalmol.1979;63(2):129-31
- ↑ Greene SL, Michels VV, Doyle JA. Variable expression in ankyloblepharon-ectodermal defects-cleft lip and palate syndrome. Am J med Genet.1987;27(1):207-12
- ↑ Hay RJ, Wells, RS. The syndrome of ankyloblepharon, ectodermal defects and cleft lip and palate: an autosomal dominant condition. Br J Dermatol.1976;94(3): 277–89
- ↑ Ioannides A, Georgakarakos ND. Management of ankyloblepharon filiforme adnatum. Eye (Lond). 2011;25(6):823
- ↑ Ozanics V, Jacobiec FA. Prenatal development of the eye and its adnexa. In: Jacobiec FA (Ed).Ocular Anatomy, embryology and teratology. Philadelphia: Harper and Row;1982.pp.83-91
- ↑ Scott MH, Richard JM, Farris BK. Ankyloblepharon filiforme adnatum associated with infantile glaucoma and iridogoniodysgenesis. J Pediatr Ophthalmol Strabismus,1994; 31:93–95
- ↑ Duke-Elder S. System of Ophthalmology: Normal and abnormal development. Part 2. Congenital deformities, 2nd edition. New York: Henry Kimpton;1964,pp.867-71
- ↑ 14.0 14.1 MacFaul PA. The ocular adnexa. Part 2. Lacrimal orbital and paraorbital diseases. In: Duke-Elders (Ed). System of Ophthalmology, 8th edition. London: Henry Kimpton;1975.pp.590-91
- ↑ Hill VA, Nischal KK, Collin JR, Harper JI. An unusual ectodermal dysplasia with unique eye defects. Br J Dermatol. 2005 Feb; 152(2):365-7.
- ↑ Nordlund ML, Holland EJ, Kersten RC. Ocular surface reconstruction in a patient with complete ankyloblepharon resulting from Steven-Johnson syndrome. Arch Ophthalmol. 2004;122(6):934-5
- ↑ Kimbrough RL, Okereke PC, stewart RH. Conservative management of cyanoacrylate ankyloblepharon: a case report. Ophthalmic Surg.1986; 17(3):176-7