Microspherophakia
All content on Eyewiki is protected by copyright law and the Terms of Service. This content may not be reproduced, copied, or put into any artificial intelligence program, including large language and generative AI models, without permission from the Academy.
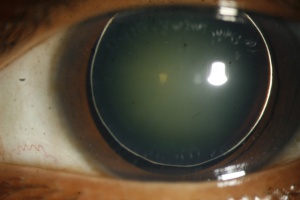
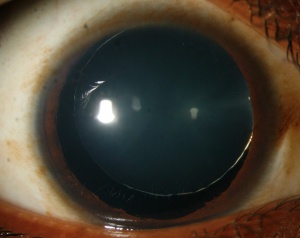
Microspherophakia (MSP) is characterized by increased anteroposterior diameter and reduced equatorial diameter of the crystalline lens. It is a rare condition, usually bilateral.
Disease Entity
Disease
Microspherophakia has the following characteristics:[1]
- It is usually bilateral
- Small diameter of the lens
- Increased anteroposterior diameter of the lens
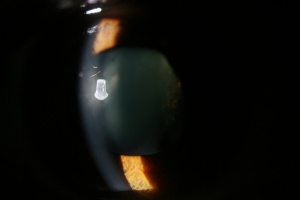
- Equator of the lens is visible with full mydriasis
- Movement of lens with change in posture
- May be associated with lens dislocation/ subluxation , high myopia, defective accommodation, glaucoma
Genetics
Mutations in following genes have been noted:
- Latent TGF β-binding protein-2 (LTBP2) gene
- ADAMTS17
LTBPs are a family of proteins showing structural homologies with fibrillins and is expressed in trabecular meshwork, ciliary processes and lens capsule/epithelium layer. It might have a role in regulation of elastic fibre assembly.
ADAMTS17 is part of same family of metalloproteinases as ADAMTS10 which is the main gene associated with Weill-Marchesani syndrome.
Associations
Microspherophakia may occur as an isolated defect, may be familial or it might be associated with systemic / local anomalies as follows:
Entities associated with microspherophakia
| Systemic |
|---|
| Weill-Marchesani syndrome |
|
Microspherophakia-metaphyseal dysplasia |
|
Klinefelter’s syndrome |
|
Rhizomelic form of Chondrodysplasia punctata |
|
Metaphyseal dysplasia |
|
Cri du chat syndrome |
|
Hyperlysinemia |
|
Mandibulofacial dystosis |
|
Congenital rubella |
| Local |
| Aniridia |
| Iridocorneal endothelial syndrome |
|
Optic disc colobomata |
Familial microspherophakia is not associated with systemic abnormalities. Pattern of inheritance is mainly autosomal recessive, but it can also be autosomal dominant.
General Pathology
In histopathological study it has been found that zonular fibers may be abnormally long and somewhat rudimentary. In addition there may be abnormal development and distribution of secondary lens fibers. Later on hyaloid degenerations are noted due to changes in shape of lens affecting the lens fibers.
Pathophysiology
Following mechanisms has been suggested :
- Arrest in development or abnormal insertion of secondary lens fibers both of which may be secondary to a nutritional deficiency from defects in tunica vasculosa lentis and may occur in the fifth and sixth month of embryonic life as the lens is normally spherical at this stage
- Zonular fibers may also be rudimentary due to lack of tension and arrest in lens development so that it may remain spherical instead of gradually converting to a normal biconvex shape
Diagnosis
History
A thorough family history and history of systemic anomalies is required.
Symptoms
Zonular instability might lead to lens dislocation/ subluxation or secondary angle closure glaucoma. Patients might present with diminution of vision or acute eye pain.
Signs
Classically, signs of microspherophakia include the triad of angle closure glaucoma, shallow anterior chamber, and refractive myopia. Other findings can include:
- Thick crystalline lens with smaller diameter and defective accommodation
- Entire equatorial margin of the lens is seen with full mydriasis which will move with change in posture
- Posterior staphyloma, myopic crescent, ectopic pupil, or blue sclera
- Signs associated with complications like ectopia lentis, glaucoma, high myopia, retinal detachment, etc.
Diagnostic procedures
UBM (ultrasound biomicroscopy) might be useful in diagnosis of microspherophakia. This imaging technology uses ultrasonic waves to produce two dimensional cross sectional images of the anterior segment. It provide morphological details of anterior chamber angle, iris, ciliary body, zonules & lens and is specially useful in challenging cases like those having small and fixed pupil.[2]
Screening tests may be required for associated systemic conditions like serum homocysteine levels and urine screening test for homocysteinuria.
Complications
Glaucoma is common in microspherophakia and has been reported in up to 51% of patients. [3] Secondary angle closure glaucoma is the most common sight threatening complication of microspherophakia. [4]
Glaucoma in microspherophakia may be caused via:
- Acute pupillary block mechanism caused by forward movement of spherical lens or anterior subluxation of lens due to weak and long zonules.
- Peripheral anterior synechiae formation due to unrelieved pupillary block causing synechial angle closure and irreversible trabecular meshwork damage.
- Chronic pupillary block leading to crowding of anterior chamber angle by the spherical lens
- Developmental anomaly of the anterior chamber angle
Progressive microspherophakia is also responsible for severe and progressive lenticular myopia while zonular instability might lead to lens dislocation or subluxation.
The probability of developing glaucoma increases with age for patients with microspherophakia. [3]
Management
Medical and surgical management of complications seen with microspherophakia may be difficult.
Cycloplegics are the treatment of choice. Miotics if given in microspherophakia might lead to pupillary block glaucoma.
Stepwise protocol for treatment of glaucoma in microspherophakia:
- Nd: Yag Laser Peripheral iridotomy (although this may have limited effect)
- Clear lens extraction with or without goniosynechiolysis
- Filtering surgery
- Tube shunt surgery
Indications of clear lens extraction in patients with microspherophakia:[5]
- Corneo-lenticular contact
- Unilateral high myopia
- Pupillary block
- Secondary intractable glaucoma
Intraoperative complications associated with clear lens extraction in these patients include difficulty in performing capsulorhexis and implanting IOL due to smaller bag size.
References
- ↑ Şimşek T, Beyazyıldız E, Şimşek E, Öztürk F. Isolated Microspherophakia Presenting with Angle-Closure Glaucoma. Türk Oftalmoloji Dergisi. 2016;46(5):237-240
- ↑ Bitar MS, Farooq AV, Abbasian J (2016) Challenges in Diagnosing Microspherophakia in a Pediatric Patient. JSM Ophthalmol 4(1): 1040
- ↑ Jump up to: 3.0 3.1 Senthil S, Rao HL, Hoang NT, et al. Glaucoma in microspherophakia: presenting features and treatment outcomes. J Glaucoma. 2014. Apr-May;23(4):262-7.
- ↑ Muralidhar R, Ankush K, Vijayalakshmi P, George V. Visual outcome and incidence of glaucoma in patients with microspherophakia. Eye. 2014;29(3):350-355
- ↑ Medhi J, DasGupta S, Bhattacharjee H, Bhattacharjee K. Clear lens extraction and intraocular lens implantation in a case of microspherophakia with secondary angle closure glaucoma. Indian Journal of Ophthalmology. 2010;58(1):67