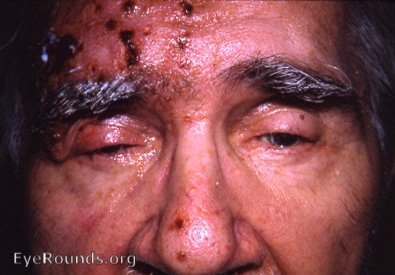
Herpes Zoster Ophthalmicus
All content on Eyewiki is protected by copyright law and the Terms of Service. This content may not be reproduced, copied, or put into any artificial intelligence program, including large language and generative AI models, without permission from the Academy.
Disease Entity
Disease
Herpes zoster ophthalmicus (HZO), commonly known as shingles, is a viral disease characterized by a unilateral painful skin rash in one or more dermatome distributions of the fifth cranial nerve (trigeminal nerve), shared by the eye and ocular adnexa. HZO occurs typically in older adults, but it can present at any age and it occurs after reactivation of latent varicella-zoster virus (VZV) that is present within the sensory spinal or cerebral ganglia.[1]
Etiology
HZO is caused by the varicella-zoster virus (VZV) that has reactivated from its dormant status in the dorsal ganglion cells of the central nervous system. From there, it travels along neurons to the sensory axons of the skin to form vesicular lesions.
Risk Factors
Virulence of the VZV and the immune status of the host are primary factors leading to the development of HZO. The incidence and severity of herpes zoster increases with advancing age, and patients over the age of 60 are at the highest risk.[2] One study showed that racial factors may play a role in the development of the disease, since elderly black patients were one-fourth as likely as elderly white patients to have herpes zoster. [3] Immune system status plays a role; patients who are treated with immunosuppressive drugs have a significantly increased risk for herpes zoster. [4] In an immunocompromised patient, HZO is more likely to result in prolonged illness, more likely to recur, and more likely to lead to myelitis and vasculopathy.[5]The risk of herpes zoster is 15 times greater in men with HIV than in men without HIV. [6]
General Pathology
HZO is a result of activated VZV, which is a double-stranded DNA virus in the herpes simplex virus group.
Pathophysiology
Unless the immune system is compromised, the VZV virus is usually suppressed. However, for reasons that are not fully understood, the virus reactivates from its dormant state in the sensory ganglion, replicates in the nerve cells, and sheds virions from the cells that are carried down the axons to the skin served by that ganglion. The local immune response results in skin blisters or ocular inflammation, depending on which tissues are affected. Perineuritis causes intense pain along with the nerve distribution.[7] Paresthesia and segmental pain at the area supplied by trigeminal nerve may be noted before the onset of rash. Aging, immunosuppression therapy, and psychological stress all could be factors resulting in reactivation of the virus. [8]
Primary Prevention
A varicella-zoster (shingles) vaccination is recommended for patients over the age of 50 or in adults aged 18 years and older who are or will be at increased risk of HZ due to immunodeficiency or immunosuppression caused by known disease or therapy. Although 90% of the population has prior exposure to VZV, there appears to be a benefit to booster immunity, especially since the community incidence of native VZV exposure has decreased. Clinical trials leading to the approval of the Shingrix recombinant vaccine in the US demonstrated >90% efficacy at preventing HZ. A recent real-world study demonstrated 70% decreased incidence of zoster and 74% reduction of postherpetic neuralgia.[9]
Diagnosis
History
Herpes zoster is an acute, painful, vesicular eruption distributed along a single dermatome and is associated with a prodrome of fever, malaise, headache, and pain in the dermatome. The vesicles typically crust and will heal within 2-6 weeks.
Physical Examination
- Visual acuity with the best correction
- External examination of eyelids, periocular skin, and scalp
- Measurement of intraocular pressure
- Slit-lamp biomicroscopy of the anterior segment, with special attention to any staining cornea defects, stroma opacities, cornea vascularization, keratic precipitates, and anterior chamber cell and flare
- Dilated examination of the lens, macula, peripheral retina, optic nerve, and vitreous.
Signs
Erythematous skin lesions with macules, papules, vesicles, pustules, and crusting lesions in the distribution of the trigeminal nerve. Hutchinson’s sign is defined as skin lesions at the tip, side, or root of the nose. This is a strong predictor of ocular inflammation and corneal denervation in HZO, especially if both branches of the nasociliary nerve are involved. [10][11]
Symptoms
Many cases of HZO exhibit a prodromal period of fever, malaise, headache, and eye pain prior to the eruption of the skin rash. The patient may describe eye pressure, tearing, eye redness, or decreasing vision. Pain in the distribution of the trigeminal nerve may be severe.
Clinical Diagnosis
Dermatome distribution pain and rash with associated ocular findings strongly suggest HZO. Corneal epithelial defects, decreased corneal sensation, and ocular inflammation in any of the layers of the eye also correlate with the diagnosis. HZO iritis is frequently associated with high intraocular pressure.
Diagnostic Procedures
Cornea sensation should be tested prior to the instillation of anesthetic drops. This can be accomplished with Corneal Esthesiometry or with a fine wisp of a cotton-tip applicator. Decreased sensation is very suspicious for herpes simplex virus (HSV). Using fluorescein, cornea epithelial defects should be ruled out.
Laboratory test
Cornea scrapings of any skin lesions may be sent to the laboratory for a Tzanck smear. However, this test will not differentiate between herpes simplex virus (HSV) and varicella virus. Alternatively, cultures may be sent for immunofluorescence assays to look for IgM specific to VZV. Viral cultures and polymerase chain reaction testing may also be obtained to diagnose VZV. [12]
Differential Diagnosis
Not many disease processes produce a painful vesicular rash. However, other conditions that create vesicular rashes should be considered, especially in the absence of pain; examples include contact dermatitis and vaccinia dermatitis. Other disease entities that can mimic cornea findings include recurrent erosion, noninfectious cornea melts, and infectious keratitis. There are numerous infectious and noninfectious entities that can exhibit ocular inflammation in the aqueous, vitreous, optic nerve, retina, and choroid.
Management
General Treatment
Skin rash treatment should prevent bacterial superinfection. With careful examination inflammation in all layers of the eye should be ruled out and treated with antivirals and steroids if indicated. When a skin rash is the only clinical sign, follow-up care must be directed to ruling out any ocular manifestations that may develop.
Medical Therapy
Oral acyclovir 800 mg PO five times daily for 7 to 10 days is the standard treatment. Alternatively, famciclovir 500 mg PO TID or valacyclovir 1000 mg PO TID can be used. If the systemic condition warrants or if the patient is unable to tolerate food by mouth, then acyclovir 5-10 mg/kg IV q8 for 5 days may be utilized.
Topical steroids (eg, prednisolone acetate 1%) should be used for interstitial keratitis and uveitis. For episodes of scleritis, retinitis, choroiditis, and optic neuritis, systemic steroids by mouth or intravenous administration should be strongly considered.
For increased intraocular pressure commonly found in herpes trabeculitis, topical steroids should be administered, as well as aqueous suppressants (eg, timolol, brimonidine, dorzolamide, acetazolamide).
Pain should be treated with narcotics if warranted. Neuropathic pain responds well to amitriptyline 25 mg PO QHS and can decrease the incidence of postherpetic neuralgia. Capsaicin cream applied to the rash may decrease pain as well. [13] Pregabalin 150 mg /day in divided doses may alleviate pain due to acute herpetic neuralgia.
Medical Follow-up
Depending on the ocular findings and severity of the disease, patients should be monitored every 1 to 7 days during the acute episode. Monitoring every 3-12 months afterward may be helpful to check for delayed sequelae such as ocular hypertension, cataract, and cornea scarring. If there is any concern about future exacerbations, viral prophylaxis should be considered, using acyclovir 400 mg PO BID.
Surgery
Cornea transplantation is sometimes required for lesions that cause severe cornea thinning and loss of structural integrity of the eye. Scars that are visually significant and refractory to medical therapy and/or hard contact lenses may require transplantation. Vitrectomy or retinal detachment surgery may be performed, especially in cases of acute retinal necrosis (ARN). Glaucoma filtration surgery is sometimes performed if there are difficulties with maintaining optimum intraocular pressure. If the intraocular inflammation and/or steroid treatment causes a cataract, then cataract surgery may be performed when the disease process is quiescent.
Surgical Follow-up
Depending on the type of surgery performed, the patient should be closely monitored for severe inflammation commonly associated with herpes after surgical procedures. Viral prophylaxis with antiviral therapy and steroids should be strongly considered.
Complications
Zoster skin manifestations in the eyelids can affect the deep dermis. Therefore, cicatrix can result in ptosis, lid scarring, ectropion, and entropion. Scleritis can cause scleral, limbal, and corneal atrophy. Inflammation in the cornea, optic nerve, retina, and choroid could result in permanent vision loss. Corneal scars commonly affect the vision, requiring hard contact lens or cornea transplantation interventions. Postherpetic neuralgia occurs in 36.6% of patients over the age of 60 and in 47.5% over the age of 70.[11]
- Ocular complications:
- Corneal disease
- Uveitis
- Postherpetic neuralgia
- Scleritis
- Ocular motor palsies
- Increased intraocular pressure (IOP)
- Acute retinal necrosis (ARN)
- Ptosis
- Cicatricial ectropion
- Neurologic complications:
- Contralateral hemiplegia due to segmental cerebral arteritis
Prognosis
Prognosis is greatly variable and dependent on long-term sequelae. Long-term vision loss, need for surgery, and long-term antiviral prophylaxis are all possible.
Additional Resources
- CDC Information on Shingles Vaccination
- CDC Information on Varicella Vaccination
- Boyd K, Yeu E. Herpes Zoster (Shingles). American Academy of Ophthalmology. EyeSmart/Eye health. https://www.aao.org/eye-health/diseases/shingles-herpes-zoster-list. Accessed March 7, 2025.
References
- ↑ Liesegang TJ. Herpes Zoster Ophthalmicus. Ophthalmology 2008;115:S3-S12.
- ↑ Chapman RS, Cross KW, Fleming DM. The incidence of shingles and its implications for vaccination policy. Vaccine 2003;21:2541-2547.
- ↑ Schmader K, George LK, Burchett BM, et al. Racial differences in the occurrence of herpes zoster. J Infect Dis 1995;171:701-704.
- ↑ Cohen PR, Grossman ME. Clinical features of human immunodeficiency virus-associated disseminated herpes zoster virus infection –a review of the literature. Clin Exp Dermatol 1989;14:273-276.
- ↑ Hilt DC, Bucholz D, Krumholz A, et al. Herpes zoster ophthalmicus and delayed contralateral hemiparesis caused by cerebral angiitis: diagnosis and management approaches. Ann Neurol 1983;14:543-553.
- ↑ Buchbinder SP, Katz MH, Hessol NA, et al. Herpes zoster and human immunodeficiency virus infection. J Infect Dis 1992;166:1153-1156.
- ↑ Schmader K. Herpes zoster and postherpetic neuralgia in older adults. Clin Geriatr Med 2007;23(3):615-632.
- ↑ Thomas SL, Hall AJ. What does epidemiology tell us about risk factors for herpes zoster?. Lancet Infect Dis 2004;4(1):26-33.
- ↑ Izurieta HS, Wu X, Forshee R, Lu Y, Sung HM, Agger PE, Chillarige Y, Link-Gelles R, Lufkin B, Wernecke M, MaCurdy TE, Kelman J, Dooling K. Recombinant Zoster Vaccine (Shingrix): Real-World Effectiveness in the First 2 Years Post-Licensure. Clin Infect Dis. 2021 Sep 15;73(6):941-948. doi: 10.1093/cid/ciab125. PMID: 33580242.
- ↑ Hutchinson J. A clinical report on herpes zoster ophthalmicus (shingles affecting the forehead and nose). Trans Am Ophthalmol Soc 1942;40:390-439.
- ↑ 11.0 11.1 Zaal MJ, Volker-Dieben HJ, D’Amarao J. Prognostic value of Hutchinson’s sign in acute herpes zoster ophthalmicus. Graefes Arch Clin Exp Ophthalmol 2003;241:187-191.
- ↑ Burns DA, et al. Rook’s Textbook of Dermatology, 7th Edition.
- ↑ Kunimoto DY, et al. Wills Eye Manual, 4th Edition.