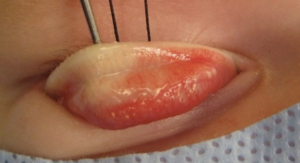
Tarsal Kink Syndrome
Disease Entity
Disease
Tarsal kink syndrome is a rare and severe form of congenital entropion characterized by horizontal kink within the upper tarsal plate. It is characterized by blepharospasm and absence of an upper eyelid fold that may lead to corneal ulceration caused by the folded edge of the upper tarsus or the inturned eyelids and eyelashes if not corrected by surgery.
It was first described by Kettesy [1] in 1948 as a folding of the tarsus in infancy, but then Callahan[2] gave it its current description – a congenital horizontal tarsal kink.
Etiology
The etiology of tarsal kink is unknown but the proposed causes include overaction of the marginal fibers of the orbicularis muscle causing tarsal infolding in utero [3][4][5]; an aponeurotic defect [4]; a primary tarsal defect [5] ; an eyelid dysjunction defect in utero [6] or an exogenous mechanical cause in utero. [7]
Diagnosis
Demographics
Age of presentation varies from 1 to 60 weeks. It is usually unilateral but can be bilateral, with male preponderance. [7],[8]
Clinical diagnosis
- Congenital inward rotation of lid margins and eyelashes toward the globe (Entropion). It is more common in lower eyelid. The diagnosis of upper eyelid may be easily missed since, examination of lower eyelid by eversion is easier than upper eyelid.
- Marked folding across the horizontal length of the upper tarsal plate. It is due to characteristic horizontal kink within the tarsal plate. Ideally requires eversion of upper eyelid for proper examination. Mild kink have obtuse tarsal bent while severe kink have acute angle tarsal bent.
- Absent upper eyelid crease
- Corneal opacity or infiltrate – the majority of the reported cases had corneal ulcers, which typically were sterile. However, microbiology work-up have revealed Corynebacterium species and Pseudomonas aeruginosa in few cases. [8]
- Secondary blepharospasm
- Photophobia
- Microphthalmos, Distichiasis has been reported to be associated.[8][9]
Systemic association
Majority of the cases do not feature systemic abnormalities, however there have been reports of associated developmental delay, cardiac abnormalities, central nervous system defects and Trisomy 13 (Patau syndrome).[9][10] The incidence of associated developmental abnormalities in children with congenital primary upper lid entropion is such that all children with upper lid entropion should be carefully assessed by a pediatrician, with particular reference to the skeletal, cardiovascular, and nervous systems.
Management
Early diagnosis and treatment of entropion is essential to reduce the risk of corneal scarring and amblyopia. Surgery is usually required to prevent damage to the cornea.
Surgery
The surgical goal involves weakening the tarsal kink with margin rotation and eyelid crease formation. Various surgical procedures have been described for the correction of congenital horizontal tarsal kink.
The surgical approaches include cutting (posterior or anterior lamella) techniques and non-cutting techniques. Each procedure has been individually successful, with no reports of recurrence.
A. Cutting methods
Different cutting methods include:
- Excision of the kink with everting sutures [2]
- Horizontal tarsal splitting with everting sutures [3]
- Anterior lamella repositioning [5]
- Transconjunctival horizontal tarsotomy with marginal rotation [8]
- Lamellar tarsoplasty [11]
- Anterior lamella resection [12]
B. Non-cutting methods
Non-cutting techniques include:
- Eyelid eversion sutures. This offers simple, minimally invasive and effective method. Various methods of everting sutures have been described.
- Three double-armed sutures placed inferior to the tarsal kink from the conjunctival surface exiting via skin superior to the upper border of tarsus and tied over cotton bolsters. [6][10]
- Prolene sutures through the anterior lamella and part of the tarsal plate and tied just above the lash line. [9]
- Three double armed 6/0 vicryl sutures passed via a transconjunctival approach extending from just above the upper edge of the tarsal plate to exit on the skin of the eyelid above the eyelashes [13]
- Intermarginal suture tarsorrhaphy or modified suture tarsorrhaphy [14][15]
- Mechanical stretching of tarsal plate over a strabismus hook followed by a temporary lid margin sutures passed through the gray line of the upper and lower eyelids[16]
Prognosis
Visual outcome in patients with tarsal kink syndrome is favourable except when the diagnosis is delayed or an ulcer develops.
Conclusion
Tarsal kink syndrome, a rare congenital eyelid disorder, is a severe disease with potentially blinding sequelae. One study reported that correct referral diagnosis was noted in only one third of patients presenting to a tertiary care referral center.[8]
Nonvisibility of upper eyelid margin, an absent upper eyelid crease and corneal opacity at birth could be important diagnostic clues for the pediatrician or comprehensive ophthalmologist. Simple surgical techniques are effective in treating this potentially vision threatening disease. Awareness about this disease entity is thus essential for early diagnosis and treatment.
References
- ↑ Kettesy A. Entropion in infancy caused by folding of the tarsus. Arch Ophthalmol 1948;39:640-3.
- ↑ Jump up to: 2.0 2.1 Callahan A. Callahan A, ed. Anomalies of the lids. In: Reconstructive Surgery of the Eyelids and Ocular Adnexa. Birmingham, AL: Aesculapius, 1966;1:37–40.
- ↑ Jump up to: 3.0 3.1 Biglan AW, Buerger GF. Congenital horizontal tarsal kink. Am J Ophthalmol 1980; 89: 522–4.
- ↑ Jump up to: 4.0 4.1 Zak TA. Congenital primary upper eyelid entropion. J Pediatr Ophthalmol Strabismus 1984; 21: 69–73
- ↑ Jump up to: 5.0 5.1 5.2 Price NC, Collin JR. Congenital horizontal tarsal kink: a simple surgical correction. British journal of ophthalmology. 1987 Mar 1;71(3):204-6.
- ↑ Jump up to: 6.0 6.1 Bosniak S, Hornblass A, Smith B. Re-examining the tarsal kink syndrome: considerations of its etiology and treatment. Ophthalmic Surgery, Lasers and Imaging Retina. 1985 Jul 1;16(7):437-40.
- ↑ Jump up to: 7.0 7.1 Sires BS. Congenital horizontal tarsal kink: clinical characteristics from a large series. Ophthal Plast Reconstr Surg 1999; 15:355–9.
- ↑ Jump up to: 8.0 8.1 8.2 8.3 8.4 Naik MN, Honavar SG, Bhaduri A, et al. Congenital horizontal tarsal kink: a single-center experience with 6 cases. Ophthalmology 2007;114:1564–8.
- ↑ Jump up to: 9.0 9.1 9.2 Aziz S, Bhatt PR, Lavy T, Dutton G. A simple correction for congenital tarsal kink associated with distichiasis. Journal of American Association for Pediatric Ophthalmology and Strabismus {JAAPOS}. 2006 Jun 1;10(3):281-2
- ↑ Jump up to: 10.0 10.1 Lucci LM, Fukumoto WK, Alvarenga LS. Trisomy 13: a rare case of congenital tarsal kink. Ophthalmic Plast Reconstr Surg 2003;19:408-10.
- ↑ McCarthey RW. Lamellar tarsoplasty. A new technique for correction of horizontal tarsal kink. Ophthalmic Surg 1984; 15: 859-60.
- ↑ Salour H1, Owji N, Razavi ME, Zeaei H. Tarsal kink syndrome associated with congenital corneal ulcer. Ophthal Plast Reconstr Surg 2003;19:81–3.
- ↑ Vahdani K, Konstantinidis A, Thaller VT. A Simple New Technique for Treatment of Tarsal Kink Syndrome. Ophthalmic Plast Reconstr Surg. 2017 May/Jun;33(3S Suppl 1):S77-S79.
- ↑ Pushker N, Meel R, Kaushal S, et al. Congenital horizontal tarsal kink with microphthalmos corrected by intermarginal suture tarsorrhaphy. J Pediatr Ophthalmol Strabismus 2010;47:51–3.
- ↑ Demirel S, Firat C, Firat PG. Modified temporary eyelid margin suture for correction of congenital horizontal tarsal kink: a novel surgical technique. Ophthal Plast Reconstr Surg 2012; 28:300–2.
- ↑ El-Mulki S, Lawson J, Taylor D. A new and simple procedure for correction of congenital tarsal kink. J Pediatr Ophthalmol Strabismus 1998;35:172-3.