Manual Small Incision Cataract Surgery
All content on Eyewiki is protected by copyright law and the Terms of Service. This content may not be reproduced, copied, or put into any artificial intelligence program, including large language and generative AI models, without permission from the Academy.
Background
Manual small-incision cataract surgery (MSICS; also SICS or SECCE) is a low-cost, small-incision form of extracapsular cataract extraction (ECCE) that is principally employed in the developing world. Compared to traditional ECCE, MSICS has the advantage of a self-sealing sutureless wound. In resource-poor settings, MSICS also has several distinct advantages over phacoemulsification, including shorter operative time, less need for technology, and lower cost.[1][2][3][4] Recent studies have shown comparable outcomes and complication rates between patients undergoing phacoemulsification and MSICS with posterior chamber intraocular lens placement.[5][6][7][8]
Surgical Technique & History of Procedure
The contemporary MSICS technique most commonly employed is based on the method that Ruit et al first described in 1999.[2] However, in 1992 Blumenthal described a technique of manual ECCE[4] that served as a basis for later developments in MSICS.
Blumenthal Technique
Blumenthal and colleagues were the first to describe a technique of manual ECCE.[4] All of the steps of the operation are not described in detail in Blumenthal’s original article. However, the authors state that with their technique of manual ECCE the nucleus can be removed through a 5 to 7 mm scleral or limbal incision:
- After performing a paracentesis and capsulorhexis, the exposed cortical material and underlying epinucleus is aspirated until the anterior surface of the nucleus is seen.
- Hydrodissection is performed by guiding a cannula along the exposed nucleus with penetration between the epinucleus and nucleus and injection of 0.1 to 0.2 cc of irrigation solution to loosen adhesions between the nucleus and epinucleus.
- With an anterior chamber maintainer in place, the tip of the cannula is positioned behind the nucleus and its tip is used to move the nucleus toward the anterior chamber.
- The dimensions of the nucleus determine the size of the scleral incision, which is performed now.
- A glide is introduced to the anterior chamber behind the nucleus and external pressure along with internal hydroexpression delivers the nucleus.
- The epinucleus is brought into the anterior chamber with a spatula and hydroexpressed whole or in pieces by aspiration through the limbal/scleral incision.
Ruit Technique
In 1999, Ruit and colleagues described a new MSICS technique based on their experience at Tilganga Eye Centre in Kathmandu, Nepal:[2][3]
- A peribulbar anesthetic injection is administered by an ophthalmic assistant
- The patient is prepped with an iodine-based antiseptic and drapes are laid over the patient
- A lid speculum is inserted
- A superior rectus bridle suture may be placed (not necessary)
- A fornix-based conjunctival flap from the 10-2 o’clock position is used to expose bare sclera
- Diathermy is used to blanch the scleral incision area
- A sclerocorneal tunnel is made and a tissue plane parallel to the ocular surface is dissected from the sclera through the limbus and 1-1.5 mm into clear cornea. The tunnel should be wider in the cornea than at its scleral opening
- A triangular capsulotomy is made with its apex at the 12 o'clock position using a 26G needle on a syringe
- A blade is used to further open the inner aspect of the sclerocorneal tunnel into the anterior chamber. This internal flaring of the tunnel helps to engage the nucleus at the time of expression
- For less mature cataracts anterior chamber irrigation fluid is injected into the lens to separate the nucleus from other lens components; the nucleus may prolapse at this point into the anterior chamber
- For more mature cataracts hydrodissection is not required. In these cases the nucleus can be prolapsed into the anterior chamber by gently rotating and tilting the nucleus with a Simcoe irrigation/aspiration cannula. If needed, fluid can be directed behind the nucleus to assist in its movement into the anterior chamber
- The nucleus should not be fragmented in the anterior chamber; two methods exist for nuclear removal:
- Method One: Use toothed forceps to grasp the lip of the incision and rotate the eye inferiorly. Pass a flowing Simcoe cannula underneath the nucleus. The hydrostatic pressure from accumulating fluid along with a gentle lifting action with the Simcoe tip forces the nucleus into the tunnel
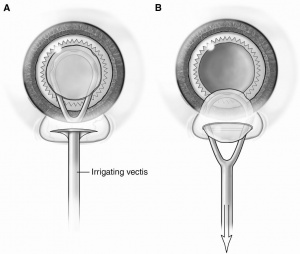
- Method Two: An irrigating vectis can be passed under the nucleus and the nucleus is lifted and drawn into the tunnel.
- A Simcoe cannula is used to remove epicortical and cortical material.
- Air is injected into the anterior chamber
- A polymethylmethacrylate intraocular lens is passed into the eye
- Using the Simcoe cannula anterior chamber air is removed and replaced with irrigation fluid
- The wound should self-seal. This is checked by pressing on the globe and observing the wound for leakage
- Subconjunctival injection of antibiotic and steroid is given just above the cut edge of conjunctiva
- The lids and closed and a standard dressing is applied
In order to make this technique sustainable in the developing world, additional innovations included the local manufacture of high-quality posterior chamber intraocular lenses for US$7 each, the development of a low-cost operating microscope (US$3000) and the development of a low-cost yttrium aluminium garnet laser (US$1200). The authors reported that average operative time was under 10 minutes and the average cost was less than $20 per surgery.[3]
Intratunnel Phacofracture Technique
In 2012, Dr, Sudhir Singh,MS published a new manual small-incision cataract surgery (MSICS) technique based on his experience at Global Hospital Research Centre, Mount Abu, India [9] [10] .The MSICS and phacoemulsification are the most popular methods of cataract extraction today. The former is significantly faster, less expensive, and less technology-dependent than phacoemulsification and has been extensively practiced in developing countries such as India. However, the draw-back of most commonly practiced MSICS techniques— Blumenthal, visco expression, irrigating wire vectis, and fish-hook needle—is that they all require a large incision of 7 to 9 mm, which leads to induced astigmatism. In the intratunnel phacofracture technique, the lens nucleus is broken inside a sub−6-mm sclerocorneal tunnel incision and removed. The nucleus removal steps take place inside the sclerocorneal tunnel, in contrast with other nucleotomy techniques in which this maneuvering takes place inside the anterior chamber. More...
Topical Intratuunel Ohacofracture Manual Small Incision Cataract Surgery HD (Unedited)
Modifications
More recently, authors have suggested modifications to the Ruit technique:[11]
- A temporal based scleral tunnel may be appropriate for patients with very deeply set orbits
- After creating the scleral tunnel superiorly, a paracentesis is made at the 9 o'clock position prior to penetrating clear cornea
- The lens capsule is stained with trypan blue under an air bubble and viscoelastic is injected into the anterior chamber
- The scleral tunnel is extended into the anterior chamber with an internal incision parallel to the limbus
- A continuous curvilear capsulorhexis is made
- Additional viscoelastic is injected prior to insertion of the intraocular lens and is then aspirated with the Simcoe cannula
- The paracentesis port is sealed by stromal hydration
- The conjunctiva can be sealed using diathermy
It is also noted that MSICS can be done along with trabeculectomy in a combined cataract-glaucoma operation using the superior conjunctival flap.[11]
Combined SICS With Trabeculectomy The Kelly's Punch HD (Unedited)
Outcomes
In their first report on MSICS outcomes, Ruit and colleagues analyzed data from 62 consecutive cases performed at Tilganga Eye Centre in Kathmandu, Nepal and 207 cases from a remote eye camp in rural Nepal.[2] The authors reported that 87.1% of patients from Tilganga had best-corrected visual acuity (BCVA) of 20/60 or better. Approximately 50% of patients at the rural eye camp had a preoperative visual acuity of counting fingers at 2 feet or worse and 74.1% had BCVA 20/60 or better at two months postoperatively. As familiarity with the MSICS technique has improved so have outcomes. In a 2007 report from the Tilganga Eye Centre, 85% of patients undergoing MSICS had an uncorrected visual acuity (UCVA) of 20/60 or better and 98% had BCVA of at least 20/60.[5]
This study and others[7][6][8][12] have compared outcomes between MSICS and phacoemulsification. In the 2007 prospective randomized trial from Tilganga Eye Centre, UCVA, BCVA and keratometric astigmatism were not significantly different between the two surgical groups. However, operative time was significantly shorter for the MSICS cohort (9.0 vs. 15.5 minutes; p<.001). Additionally, the per-case cost of surgical supplies was US$70 for phacoemulsification and US$15 for MSICS.[5] In another trial, investigators from India also compared phacoemulsification and MSICS. Among both groups, 98% of patients attained a BCVA of 20/60 by post-operative week six. However, UCVA was better in the phacoemulsification group.[7] L. V. Prasad Eye Institute, also in India, examined outcomes of MSICS and phacoemulsification performed by ophthalmology trainees at their institution. There was no difference in BCVA between groups. However, the complication rate was higher among the MSICS cohort which was significantly older and had worse preoperative visual acuity.[6] A 2012 study of 127644 cataract surgeries at Aravind Eye Hospital compared complication rates and types of complication for phacoemulsification, MSICS and ECCE. The complication rates for these procedures were 1.01% and 1.11% and 2.6%, respectively. Subgroup analysis showed that the combined complication rate for all trainees was higher with phacoemulsification compared to MSICS. The rate of endophthalmitis did not differ by surgical method.[12] A recent Cochrane Review sought to synthesize available data comparing phacoemulsification and MSICS. Eight trials with a total of 1708 patients were included in the meta-analysis. The investigators found similar BVCA using either surgical technique but better short-term UCVA after phacoemulsification. They note that the number of complications was low with both techniques but that they were underpowered to detect differences in complication rate, poor visual outcome or long-term outcome. Overall, in the included studies phacoemulsification was about four times costlier than MSICS.[8]
Developing World Applications
Approximately 39 million people are blind worldwide.[13] According to a 2004 World Health Organization report, 47.8% of blindness worldwide is due to cataract.[14] Of the disability-adjusted life years due to cataract more than 90% are in the developing world.[15] Cost of surgery and lack of awareness are the most commonly cited barriers to patients obtaining surgery in developing countries.[16] Accordingly, solutions are needed to provide high-volume, low-cost cataract surgery. Investigations have consistently demonstrated similar visual outcomes and complication rates between phacoemulsification and MSICS, while MSICS is considerably faster, less expensive and less dependent on expensive technology than phacoemulsification.[16] Additionally, some authors have even suggested that MSICS (or ECCE) may be preferred over phacoemulsification for very hard cataracts, which are frequently encountered in resource-poor settings.[17][16]
MSICS appears to offer a promising avenue for increasing surgical coverage in resource-poor areas of the world without sacrificing clinical outcomes.
References
- ↑ Kongsap P. Visual outcome of manual small-incision cataract surgery: comparison of modified Blumenthal and Ruit techniques. Int J Ophthalmol, 2011;4(1):62-5.
- ↑ 2.0 2.1 2.2 2.3 Ruit S, Tabin GC, Nissman SA, et al. Low-cost high-volume extracapsular cataract extraction with posterior-chamber intraocular lens implantation in Nepal. Ophthalmol, 1999; 106(10):1887-92.
- ↑ 3.0 3.1 3.2 Ruit S, Paudyal G, Gurung R, et al. An innovation in developing world cataract surgery: sutureless extracapsular cataract extraction with intraocular lens implantation. Clin Experiment Ophthalmol, 2000; 28(4):274-9.
- ↑ 4.0 4.1 4.2 Blumenthal M, Ashkenazi I, Assia E, Cahane M. Ophthalmic Surg, 1992;23(10):699-701.
- ↑ 5.0 5.1 5.2 Ruit S, Tabin G, Chang D, et al. A prospective randomized clinical trial of phacoemulsification vs manual sutureless small-incision cataract surgery in Nepal. Am J Ophthalmol, 2007;143:32-8.
- ↑ 6.0 6.1 6.2 Khanna RC, Kaza S, Palamaner SSG, Sangwan VS. Comparative outcomes of manual small-incision cataract surgery and phacoemulsification performed by ophthalmology trainees in a tertiary eye care hospital in India: a retrospective cohort design. BMJ Open, 2012;2(5).
- ↑ 7.0 7.1 7.2 Gogate PM, Kulkarni SR, Krishnaiah S. Safety and efficacy of phacoemulsification compared with manual small-incision cataract surgery by a randomized controlled clinical trial: six-week results. Ophthalmol, 2005;112(5):869-74.
- ↑ 8.0 8.1 8.2 Riaz Y, de Silva SR, Evans JR. Manual small incision cataract surgery (MSICS) with posterior chamber intraocular lens versus phacoemulsification with posterior chamber intraocular lens for age-related cataract. Cochrane Database Syst Rev, 2103;10.
- ↑ Sudhir Singh. First Postoperative Day Visual Outcome Following 6 mm Manual Small Incision Cataract Surgery Using Intratunnel Phacofracture Technique. US Ophthalmic Review, 2014;7(1):26–30
- ↑ Sudhir Singh.Step By Step:intratunnel Phacofracture.Cataract & Refractive Surgery Today Europe.May 2016:38-41
- ↑ 11.0 11.1 Dhanapal P and Yadalla D. How to Perform Manual Small-Incision Cataract Surgery. EyeNet Magazine. http://www.aao.org/publications/eyenet/201006/pearls.cfm. Accessed December 25, 2013.
- ↑ 12.0 12.1 Haripriya A, Chang DF, Reena M, Shekhar M. Complication rates of phacoemulsification and manual small-incision cataract surgery at Aravind Eye Hospital. J Cataract Refract Surg, 2012;38(8):1360-9.
- ↑ Pascolini D, Mariotti SP. Global estimates of visual impairment: 2010. Br J Ophthalmol, 2012;96(5):614-8.
- ↑ Resnikoff S, Pascolini D, Etya'ale D, et al. Global data on visual impairment in the year 2002. Bull World Health Organ, 2004;82(11):844-51.
- ↑ Ono K, Hiratsuka Y, Murakami A. Global inequality in eye health: country-level analysis from the global burden of disease study. Am J Public Health, 2010;100(9):1784-8.
- ↑ 16.0 16.1 16.2 Tabin G, Chen M, Espandar L. Cataract Surgery for the developing world. Curr Opin Ophthalmol, 2008;19:55-9.
- ↑ Bourne RR, Minassian DC, Dart JK, et al. Effect of cataract surgery on the corneal endothelium: modern phacoemulsification compared with extracapsular cataract surgery. Ophthalmol, 2004; 111(4):679-85.