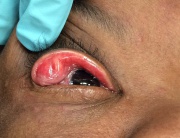
Floppy Eyelid Syndrome
All content on Eyewiki is protected by copyright law and the Terms of Service. This content may not be reproduced, copied, or put into any artificial intelligence program, including large language and generative AI models, without permission from the Academy.
Disease Entity
Disease
Floppy eyelid syndrome (FES) is an underdiagnosed, frequently bilateral eyelid malposition commonly involving the upper eyelids, presenting as recurrent or chronic ocular surface irritation and chronic papillary conjunctivitis of upper palpebral conjunctiva from severe eyelid laxity. It has a strong association with obesity, obstructive sleep apnea (OSA), etc.
Etiology
The extensive eyelid laxity can be attributed to significant decrease in elastin content when eyelid tissue was examined by special stains, immunohistochemistry, and electron microscopy. A report by Parunovic suggests that mechanical stimulation of the lid results to the upregulation of enzymes causing elastolysis which degrades the elastic properties of the lid, resulting to tarsal laxity.[1] Collagen content has not been noted to be decreased in these patients. This decrease in elastin content may explain the spontaneous eversion ("floppy") of upper eyelids especially at sleep, leading to chronic irritation and inflammation of the tarsal and palpebral conjunctiva being mechanically irritated by constant rubbing with the pillow. It has been observed that patients who sleep on one side more than the other side tend to have more severe changes on that side. This finding suggests mechanical injury as the primary cause of the papillary conjunctivitis in patients with FES. Other postulated pathophysiology suggests that the cause of the chronic conjunctivitis is poor apposition of the lax upper eyelid to the globe with inadequate spreading of the tear film. This condition leads to corneal and conjunctival compromise, rather than direct mechanical irritation.
Association
FES is known to be associated with obesity, male gender, obstructive sleep apnea, Down syndrome, and keratoconus. Keratoconus can also be linked to frequent rubbing and mechanical effect of upper eyelids on the cornea. Like a few other eyelid conditions related to upper or lower eyelid laxity, it is far less commonly seen in East Asians.
Diagnosis
History
Patients initially present with non-specific symptoms including eye irritation and a long history of unilateral or bilateral ocular redness and discharge. They may describe the eyelids spontaneously "flipping over" when they sleep, especially in prone position, due to rubbing on the pillow. Some patients may have a history of preexisting obstructive sleep apnea and/or history of heavy snoring. These symptoms in association with increased body mass index, a diagnosis of obstructive sleep apnea or use of a C-PAP or BiPAP device and the ethnicity should alert the ophthalmologist about the possibility of floppy eyelid syndrome . However, many reports have also documented the symptoms and signs of floppy eyelid syndrome in patients of both genders and without a history of obesity or sleep disorders.
Physical examination
Easy eversion of the eyelid without excess manipulation or even spontaneous eversion is an important examination mark for FES with subsequent increased horizontal laxity and redundancy of the lid (See Figure). The lateral upper eyelid may appear elongated and imbricate (overlap) over the edge of the lower lid margin. Chronic severe papillary conjunctivitis with whitish mucus discharge is often present.
Superficial punctate erosions, corneal, abrasions and microbial keratitis, and eyelashes ptosis are common clinical findings. Occasionally dry eye symptoms with low tear meniscus or discharge
Occasionally, this condition may be associated with keratoconus.
Diagnostic procedures
There is no diagnostic test for this entity. It is primarily a clinical diagnosis based on history, clinical features and systemic association. It should be directed to address possible associated conditions including obstructive sleep apnea and keratoconus and other morbidity consequences of obesity and obstructive sleep apnea. When possible, affected patients should be managed in cooperation with internal medical team and sleep disorder specialist.
Differential diagnosis
- Blepharitis
- Allergic conjunctivitis
- Atopic keratoconjunctivitis
- Superior limbic keratoconjunctivitis
- Involutional Ptosis
- Giant papillary conjunctivitis
- Contact lens complication
- Dermatochalasis
- Ectropion
Management
Supportive measures such as ocular lubrication, nighttime ophthalmic ointment and temporary antihistamine in addition to prevention of the upper lid from everting during sleep by taping the eyelids laterally or the use of eye shield can be effective in solving the patient's complaints temporarily. Addressing underlying obesity, obstructive sleep apnea and avoiding sleeping in the prone position may also improve symptoms. There is evidence that high axenic hypopneic index may be positively correlated with the development of FES and hence mitigation of the same using CPAP devices may be beneficial. If there is minimal response to medical treatment, surgical procedures such as horizontal eyelid shortening with a lateral tarsal strip procedure can help to relieve ocular symptoms and provide good functional and cosmetic results, which may be performed both for the lower eyelids and upper eyelids as indicated. Other notable techniques include a full-thickness wedge-excision, a simple lateral tarsorrhaphy or a lateral canthal tendon plication.[2][3][4] Surgery should be considered in significantly symptomatic patients , after controlling ocular surface disease, optimising their medical status with tightening procedures, that may often involve full thickness upper eyelid resection.
If upper lid laxity is predominantly medial, excision of this area may stabilize the upper eyelid in an anatomic fashion.
General treatment
Obstructive sleep apnea is a potentially fatal disorder. Frequent episodes of apnea and hypopnea can lead to systemic and pulmonary hypertension and, ultimately, congestive cardiomyopathy and heart failure. Patients need to be managed by a sleep specialist to prevent these potentially fatal conditions.
References
- Orbit, Eyelids and Lacrimal System, Section 7. Basic and Clinical Science Course, AAO, 2011-2012.
- Burkat CN, Lemke BN. Acquired lax eyelid syndrome: an unrecognized cause of the chronically irritated eye. Ophthal Plast Reconstr Surg. 2005 Jan;21(1):52-8.
- Fowler AM, Dutton JJ Floppy eyelid syndrome as a subset of lax eyelid conditions: relationships and clinical relevance. Ophthal Plast Reconstr Surg. 2010;26(3):195-204.
- Valenzuela AA, Sullivan TJ. Medial upper eyelid shortening to correct medial eyelid laxity in floppy eyelid syndrome: a new surgical approach. Ophthal Plast Reconstr Surg. 2005;21(4):259-63.
- Chambe J, Laib S, Hubbard J, Erhardt C, Ruppert E, Schroder C, et al. Floppy eyelid syndrome is associated with obstructive sleep apnea: a prospective study on 127 patients. J Sleep Res. Oct 11 2011.
- Periman LM, Sires BS. Floppy eyelid syndrome: a modified surgical technique. Ophthal Plast Reconstr Surg.2002;(18)5:370-2.
- ↑ Parunović A. Floppy eyelid syndrome. Br J Ophthalmol. 1983 Apr;67(4):264-6.
- ↑ Phillips ME, Fowler BT, Dryden SC, Fleming JC. Canthal V-plasty for Floppy Eyelid Surgery. Plast Reconstr Surg Glob Open. 2019 Oct;7(10):e2464.
- ↑ Dutton JJ. Surgical management of floppy eyelid syndrome. Am J Ophthalmol. 1985 May 15;99(5):557-60.
- ↑ Scholten E, Marck KW, Grond AJ. Surgical correction of floppy eyelids. Br J Plast Surg. 1998 Apr;51(3):264-6.