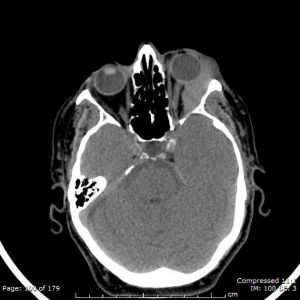
Orbital Lymphoma
All content on Eyewiki is protected by copyright law and the Terms of Service. This content may not be reproduced, copied, or put into any artificial intelligence program, including large language and generative AI models, without permission from the Academy.
Disease Entity
Lymphoproliferative tumors of the ocular adnexa encompass a wide spectrum of lesions that range from reactive benign hyperplasia to malignant lymphoma. Ocular adnexal lymphoma (OAL) is a localized form of systemic lymphoma affecting the orbit, the lacrimal gland, the lids and/or the conjunctiva. It comprises 6-8% of orbital tumors, and 10-15% of adnexal lesions.
Disease
Ocular adnexal lymphoma (OAL) is considered primary if it involves the ocular adnexa alone and secondary if it is accompanied by a lymphoma of identical type at another site. OAL is defined as solitary if it involves one or both orbits only, extension if it involves contiguous sites such as the sinuses, and systemic if remote sites are involved. The majority of lesions in this area are non-Hodgkin lymphoma (NHL), 80% of which arises from B-lymphocytes, 14% from T cells and only 6% from natural killer cells. The most common primary OAL is the low-grade malignant extranodal marginal zone B-cell lymphoma of mucosa-associated lymphoid tissue (ENZL or MALT), but other types can occur: follicular lymphoma (FL), diffuse large B-cell lymphoma (DLBCL), mantle cell lymphoma (MCL) and lymphoplasmatic lymphoma (LPL). Secondary OALs arise from systemic disease and are represented by intermediate or high-grade follicular lymphomas. The reported frequency of involvement of periocular sites is: conjunctiva, 20% to 33%; orbit, 46% to 74%; and eyelid, 5% to 20%. In those presenting with orbital lymphoma alone, systemic lymphoma eventually develops in one-third of patients by 10 years, whereas only 5% of patients with NHL develop ocular adnexal involvement during the course of their disease.
Etiology
Tumors arise from germinal center cells (follicular lymphoma), mantel cells (mantle cell lymphoma) or memory B cells (extranodal marginal zone lymphoma) all of which have undergone antigen exposure. The infection/inflammation/mutation model (IMM) of lymphopathogenesis explains why the ocular adnexa is so often affected by lymphoma, occurring as a result of mistakes during normal lymphocyte response to infection or inflammation.
Risk Factors and Pathophysiology
Though there are no clear risk factors of orbital lymphoma, a combination of infectious, genetic, and inflammatory factors have been proposed. Multiple infectious etiologies have been implicated including chronic Chlamydia psittaci, the herpesvirus, TCLV, HIV, and possibly Toxoplasma gondii and Helicobacter pylori while other pathogens remain controversial. Furthermore, there are reports of autoimmune and inflammatory disorders such as Sjogren's Syndrome as a risk factor for development of lymphoma. On a genetic level, single nucleotide polymorphisms of TNF and IL-10 have been implicated drivers of development of DLBCL. In summary, chronic antigenic stimulation through any route may promote lymphoma within the orbit.
On an epidemiologic level, there is a higher incidence in females and in Asian and Pacific Islanders, while lower in Caucasian and African Americans.
Diagnosis
Clinical and imaging data cannot be used to make the diagnosis of OAL with certainty. Diagnosis is made based on a combination of histopathologic, immunophenotypic, and molecular genetic studies, therefore, open biopsy should be obtained. If conjunctival or eyelid OAL is identified clinically, MRI or CT of the orbit is indicated for staging. If there is palpable cervical adenopathy, imaging of this region is performed as well. As more than half of patients have systemic lymphoma at the time of orbital diagnosis or will develop the disease, it is important to run a complete systemic evaluation at diagnosis and at regular follow-ups. The role of positron-emission tomography (PET) scanning in lymphoma staging and more particularly in staging of OAL is not established. PET has greater sensitivity in detecting abnormalities than does CT or MRI, but the significance of minimal lesions is not known. In addition, dynamic contrast-enhanced (DCE) in combination with diffusion-weighted imaging (DWI) has demonstrated efficacy in differentiation of lacrimal gland tumors and may be of assistance in diagnosis and treatment.
Radiology
Computed Tomography (CT): CT findings may commonly show a moderately well-defined homogeneous orbital mass molding to the adjacent ocular structures without bony involvement. Patterns of presentation include retroocular, anterior preseptal, lacrimal gland involvement, or extension of adnexal lesion. Higher grade lesions are associated with a more heterogeneous mass appearance with bony destruction.
Magnetic Resonance Imaging (MRI): MRI findings may commonly show an isointense or hypointense orbital mass on T1-weighted MRI and an isointense or hyperintense orbital mass on T2-weighted MRI.
Spiral CT: Findings may show decreased density on delayed images which aids in differentiation from orbital pseudotumor (increased density)
Histopathology
In the large majority of cases, orbital lymphoma classically presents as a low-grade malignancy, with marginal zone B-cell lymphoma of the mucosa-associated lymphoid tissue (MALT) being the major type of lymphoma, accounting for 40% to 70% of orbital lymphomas. MALT lymphomas carry a unique characteristic known as “homing” which allows the lymphoma cells to adhere to epithelial and mucosal sites leading to potential for bilateral involvement.
In order to confirm diagnosis, biopsy may be performed, followed by flow cytometry specifically looking for markers CD20, BCL-2, CD21, CD23, CD43, CD3, CD5, p53, cyclin D1, pan-cytokeratin, kappa, lambda, IgD.
The Revised European American Lymphoma (REAL) classification system segments lymphomas on the basis of histological, immunophenotypic, and genetic features, with MALT tumors similarly considered to be most common in this classification. This scheme classifies based off of subtype (eg DLBCL, EMZL), and morphology (eg large cells, minimal cytoplasm, prominent nucleoli, centrocyte-like cells, plasmacellular differentiation) to facilitate diagnosis and treatment of intra and extranodal orbital lymphoma.
Grading and Staging
Grading and staging is done through the Ann Arbor system. (E) denotes local extranodal extension. (A) denotes asymptomatic status. (B) denotes fever, night sweats, unexpected weight loss.
Grading
- Low grade. Indolent or slow growth rate
- Intermediate grade. Moderate growth rate
- High grade. Aggressive or rapid growth rate
Staging
- Stage I. Confined to the orbit
- Stage II. Involvement of adjacent structures such as the sinuses, tonsil, and/or nose
- Stage III. Abdominal nodal disease below the diaphragm
- Stage IV. Disseminated involvement of one or more extranodal sites, such as liver or bone
History
Orbital lymphoma more commonly presents in the middle-age and the elderly. Patients will often present with an orbital process that has been slowly progressing, and typically painless. Severe pain, or rapid onset should raise suspicion for a different process.
Signs
In the conjunctiva: the typical lesion is salmon or flesh-pink color. In the orbit, eyelid or lacrimal gland: when palpable, the masses are firm. If present in the lacrimal gland, the typical presentation may appear to be an "S-shaped" mass due to the lateral location of the lacrimal gland. Proptosis should be measured with exophthalmometry. Ptosis and decreased levator function may indicate superior orbital and levator muscle involvement, and motility should also be measured if the patient complains of diplopia. Signs are more commonly unilateral, although bilateral involvement may also occur.
Symptoms
Many lesions are asymptomatic but depending on the location of the mass, patients can complaint of exophthalmos, pain or diplopia, as well of conjunctival, eyelid, orbital or lacrimal gland mass. With a lacrimal gland mass or anterior orbital extension, patients complain of an eyelid swelling or fullness in the lid. If the tumor is located in the posterior orbit, the patient can complain of proptosis, or double vision.
Differential diagnosis
Differential diagnosis includes benign lymphoproliferative lesions, lymphoid hyperplasia, systemic lymphoma, metastasis, amelanotic melanoma, epithelial tumors, inflammatory and infectious lesions, orbital pseudotumor, cavernous hemangioma, among others.
Management
Radiation: it has been the most frequently used modality for treating OAL, because many patients present with localized disease. Electron or photon irradiation can be used depending on the site, extent of disease and the tumor grade or type. A wide variation of doses has been recommended, ranging from lows of 15–20 Gy up to 40 Gy. Typical doses are 26 to 36 Gy. More recently, studies have suggested that low dose radiotherapy (defined as 2Gy x 2 fractions) is an effective alternative to moderate-dose radiotherapy (4-36 Gy) for indolent orbital adnexal lymphomas. Recurrences of low-grade types are often treatable with local modalities.
Chemotherapy: Systemic chemotherapy is not routinely indicated for solitary OAL, except in the presence of diffuse large B-cell lymphoma (DLBCL). For OAL part of stage II or greater, chemotherapy has included the use of standard regimens for systemic lymphoma.
Immunotherapy - The local use of IFN-a for OAL is not yet established. - Antilymphocyte antibodies represent the newest form of lymphoma treatment. Using antibodies to CD20 (rituximab), destruction of B cells can take place based on the induction of apoptosis, complement-mediated cytolysis, and antibody-dependent cytoxicity.
In microbial-associated MALT lymphomas, antimicrobial treatment can lead to remission. Further studies are needed to verify this infectious association and those with other possible inciting pathogens.
Surgery
Typically, surgery is performed to obtain adequate specimens for biopsy and histopathological evaluation. Complete excision is usually not indicated nor performed, and can risk injury to vital orbital structures. Excision is reserved for small localized lesions of the conjunctiva and orbit. Cryotherapy has been used infrequently for OAL, with varying success. Typically, it is used in patients with conjunctival lymphoma to reduce tumor bulging or those unable to receive other treatment modalities.
Complications
Complications include biopsy related injury to adjacent eyelid and orbital structures as well as side effects from treatment modalities such as orbital radiotherapy
Followup
Patients with orbital lymphoma that have undergone treatment require lifelong follow-up to monitor for complications, recurrence and secondary tumor formation with complete history, physical examination, and radiologic evaluation. It is suggested that visits should occur once every three months for two years, once every 6 months for three years after and annually after that with close coordination with an oncologist and radiation oncologist if involved.
Prognosis
The site of presentation of OAL has been associated with prognosis with 20% of conjunctival, 35% of orbital, and 67% of eyelid OALs developing systemic lymphoma after 4 years. Among the common OAL tumor types, EMZL, FL, and LPL are considered low grade or indolent, whereas DLBCL and MCL are considered high grade. Mortality for EMZL ranges from 0-20%, FL 20-37%, MCL 38-100% and LPL 14-100%. The mean time to relapse was over 5 years, suggesting that longer follow-up than typically recommended is needed.
References
- Bardenstein DS. Ocular Adnexal Lymphoma: Classification, Clinical Disease, and Molecular Biology. Ophthalmology clinics of North America. 2005; vol:18(1):187-197.
- Bardenstein DS. Orbital and adnexal lymphoma. In: Singh AD, Damato BE, Peér J, Murphree AL, Perry JD, ed. Clinical Ophthalmic Oncology. Philadelphia. Saunders-Elsevier. 2007:565-570.
- Bernardini FP, Bazzan M. Lymphoproliferative disease of the orbit. Current opinion in ophthalmology. 2007; vol 18(5):398 -401
- Rootman J, White VA, Connors JM, Gascoyne RD. Lymphoproliferative, leukemic, and Histiocytic Lesions of the Orbit. In: Rootman J, ed. Diseases of the orbit: a multidisciplinary approach. Philadelphia, 2nd ed. Lippincott Williams & Wilkins; 2003:385-416
- Honavar SG, Manjandavida FP. Recent Advances in Orbital Tumors--A Review of Publications from 2014-2016. Asia Pac J Ophthalmol (Phila). 2017 Mar-Apr;6(2):153-158.
- Yen MT, Bilyk JR, Wladis EJ, Bradley EA, Mawn LA. Treatments for ocular adnexal lymphoma: a report by the American Academy of Ophthalmology. Ophthalmology. 2018;125:127-136.
- Moslehi R, Schymura MJ, Nayak S, Coles FB. Ocular adnexal non-Hodgkin’s lymphoma: a review of epidemiology and risk factors. Expert review of ophthalmology. 2011 Apr 1;6(2):181-93.
- Baron, Jonathan, Christopher M. Wright, Daniel Y. Lee, Maribel Carpenter, Shwetha H. Manjunath, César A. Briceño, Elise Chong, Amit Maity, John P. Plastaras, and Ima Paydar. Low-Dose Radiotherapy Versus Moderate-Dose Radiotherapy for the Treatment of Indolent Orbital Adnexal Lymphomas. Frontiers in Oncology 11 (2021): 2662.
- Li X, Wu X, Qian J, Yuan Y, Wang S, Ye X, Sha Y, Zhang R, Ren H. Differentiation of lacrimal gland tumors using the multi-model MRI: classification and regression tree (CART)-based analysis. Acta Radiologica. 2021 May 31:02841851211021039.
- Demirci H, Shields CL, Karatza EC, Shields JA. Orbital lymphoproliferative tumors: analysis of clinical features and systemic involvement in 160 cases. Ophthalmology. 2008;115(9):1626–31, 1631.e1–3.
- Auw-Haedrich C, Coupland S, Kapp A, et al. Long term outcome of ocular adnexal lymphoma subtyped according to the REAL classification. Br J Ophthalmol. 2001;85:63–9.
- Rao, Raksha, and Santosh G. Honavar. Orbital Tumors. Ocular Tumors. Springer, Singapore, 2021. 155-173.
- Ocular adnexal marginal zone lymphoma (OAMZL). (n.d.). http://atlasgeneticsoncology.org/Anomalies/OcularAdnexalMZLID1778.html
- Harris NL, JaVe ES, Stein H, et al. A revised EuropeanAmerican classification of lymphoid neoplasms: a proposal from the International Lymphoma Study Group. Blood 1994;84:1361–92.
- Eckardt, A.M., Lemound, J., Rana, M. et al. Orbital lymphoma: diagnostic approach and treatment outcome. World J Surg Onc 11, 73 (2013). https://doi.org/10.1186/1477-7819-11-73