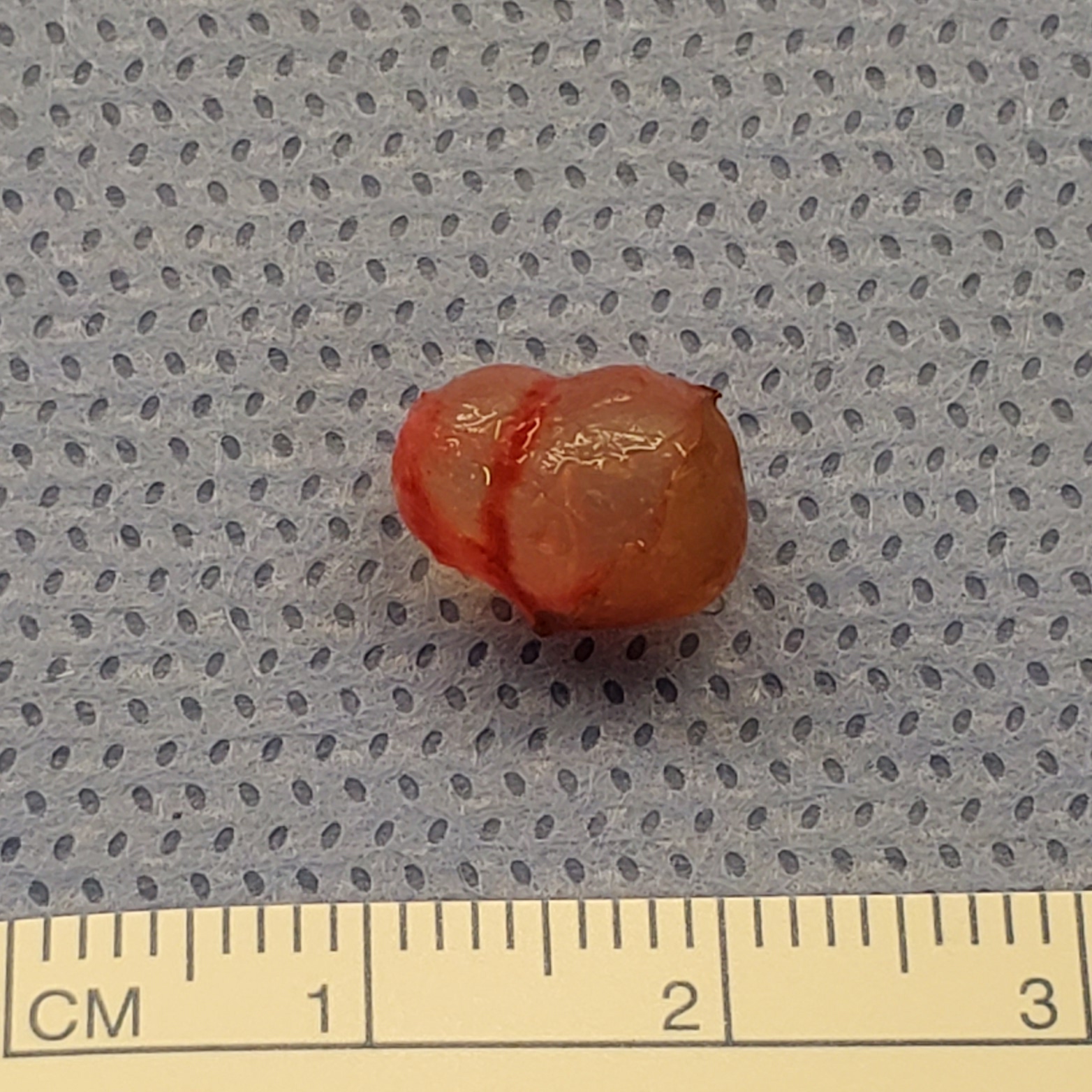
Eccrine Hidrocystoma
All content on Eyewiki is protected by copyright law and the Terms of Service. This content may not be reproduced, copied, or put into any artificial intelligence program, including large language and generative AI models, without permission from the Academy.
Eccrine hidrocystomas are benign cystic lesions of the eyelids.
Disease Entity
- 2022 ICD10 = D23.10
Disease
Eccrine hidrocystomas are small translucent, fluid-filled cysts of eccrine duct origin.[1] They are considered to be ductal retention cysts, and often enlarge in conditions that stimulate perspiration. Hidrocystomas can be classified into solitary (Smith) type and multiple (Robinson) type.[2] Solitary lesions present as skin-colored dome-shaped papules in the periorbital area usually located along the lower eyelids and canthi near but not directly involving the eyelid margin.[3] Solitary lesions typically affect males and females equally.[2] Lesions typically range from 1 to 3 mm in diameter although they may continue grow until surgical intervention or trauma.[4] Multiple type lesions are smaller in diameter and predominantly affect women in the perioribtal and malar areas. They are associated with conditions that cause hyperhidrosis and often exacerbated by hot and humid environments. Multiple eccrine hidrocystoma has been reported to be associated with Graves’ disease[5], Parkinson’s disease, idiopathic craniofacial hyperhidrosis,[6] and prolactinoma.[7]
Epidemiology
A study of the histologic features of 5504 eyelid skin tumors diagnosed in Lausanne, Switzerland showed 84% of them to be benign, and 8% of those were hidrocystomas (eccrine and apocrine).[8]
A retrospective study from two institutions over 7 years showed 107 patients diagnosed with hidrocystomas (eccrine and apocrine) with a mean age at diagnosis of 56 years (range 22-85). Lesions were found in 69 (64.4%) females and 38 (35.5%) males. Lesions were largely unilateral (74.8%) and found on the lower lid (38.6%), lateral canthus (31.2%), upper lid (17.7%), and medial canthus (12.6%). Recurrences were seen in 2.3% of lesions treated by excisional biopsy possibly related to incomplete excision or cyst rupture with residual cyst wall.[9]
General Pathology
Histopathologic features of the lesions include a solitary cyst lined by a double-layered cuboidal epithelium.[1] Eccrine secretory tubules and ducts are typically located below the cyst in close proximity to the wall. There is no connection between the cyst and the overlying epidermis.[10]
Diagnosis
Eccrine hidrocystomas are diagnosed primarily by history and clinical exam. Lesions are typically smooth cysts, single or multi lobular, and transilluminate with light. They are often located in the lateral or medial canthal eyelid skin, and can be multiloculated. They have also been reported in the peripunctal region an even in the orbit (Marangoz D, Doğan Ekici I, Çiftçi F. Orbital Eccrine Hidrocystoma. Turk J Ophthalmol. 2016 Oct;46(5):251-254. doi: 10.4274/tjo.98853. Epub 2016 Oct 17. PMID: 28058171; PMCID: PMC5200841.
Diagnostic procedures
Imaging is not required for diagnosis. Excisional biopsy is required to make a definitive diagnosis.
Differential diagnosis
- Apocrine hidrocystoma: small solitary cyst usually < 1 cm in diameter filled with milky fluid and shiny overlying skin. In contrast to eccrine hidrocystomas, these lesions are thought to be proliferative in origin and do not increase in size in hot weather.[1]
- Syringoma: benign tumor arising from adenomatous proliferation of the intraepidermal duct of eccrine glands. Appear as multiple 1-3 mm skin color or slight yellowish papules distributed symmetrically over the lower eyelids and malar region.[1]
- Epidermal inclusion cyst: slow growing keratin filled subcutaneous lesion caused by implantation of epidermis into the dermis following trauma or surgery.[3]
- Basal cell carcinoma
Management
Management options include observation versus excisional biopsy.
Surgical therapy
Most eccrine hidrocystomas are solitary and surgical treatment of choice is complete excision with an intact cyst.[1] Simple needle puncture is generally not recommended as recurrences are common and may result in infections but may be considered if patient is unwilling for complete excision.[11] Cauterization and electrodessication of the cyst wall have also been reported in cases of recurrent eccrine cysts.[12]
Medical therapy
Multiple eccrine hidrocystomas are often associated with excessive sweating and exacerbated by exercise or elevated ambient temperature. Anticholinergic therapy has been hypothesized to improve symptoms. Oral atropine was the first successful pharmacological therapy reported for multiple hidrocystomas, but was associated with multiple systemic anticholinergic side-effects.[13] Topical atropine and scopolamine creams has been used in several case reports with highly variable outcomes.[11][14] Furthermore anticholinergic side effects such as mydriasis could cause patients to discontinue the treatment.[11] Other medical treatments reported in the literature include 0.5% glycopyrrolate aqueous solution6 and botulinum toxin A to suppress eccrine epithelial secretion by reversible cholinergic blockade of nerves supplying eccrine glands.[15] Laser therapy has also been reported to treat cystic lesions, and in one study had no evidence of recurrence 18 months following treatment.[16]
Complications
A large upper eyelid eccrine hidrocystoma has been reported to cause progressive ptosis in childhood and a potential risk factor for amblyopia.[17][18] Lesions localized to peripunctal area may cause epiphora secondary to compression effects on the punctum and canaliculus.[19] Incomplete resections may result in recurrences.
References
- ↑ Jump up to: 1.0 1.1 1.2 1.3 1.4 Yanoff, M, Duker, J.S. Ophthalmology. 5thedition. (2019). 1293-1303.
- ↑ Jump up to: 2.0 2.1 Smith, J. D. Hidrocystomas. Arch. Dermatol.108, 676 (1973).
- ↑ Jump up to: 3.0 3.1 Bowling, B. & Kanski, J. J. Kanski’s clinical ophthalmology: a systematic approach. (Elsevier, 2016). 1:2-12
- ↑ American Academy of Ophthalmology. Basic and clinical science course, 2017-2018. Orbits eyelids and lacrimal system. 10:170-172 (2017)
- ↑ Kim, Y.-D. et al.Multiple eccrine hidrocystomas associated with Graves’ disease. Int. J. Dermatol.3 (2002).
- ↑ Garnacho Saucedo, G. M., Moreno Jiménez, J. C., Jiménez Puya, R. & Rodríguez Bujaldon, A. Therapeutic Hotline: Topical glycopyrrolate: a successful treatment for craniofacial hyperhidrosis and eccrine hidrocystomas. Dermatol. Ther.23, 94–97 (2010).
- ↑ Ma, L., Jakobiec, F. A., Wolkow, N., Dryja, T. P. & Borodic, G. E. Multiple Eyelid Cysts (Apocrine and Eccrine Hidrocystomas, Trichilemmal Cyst, and Hybrid Cyst) in a Patient With a Prolactinoma. Ophthal. Plast. Reconstr. Surg.34, e83–e85 (2018).
- ↑ Deprez, M. & Uffer, S. Clinicopathological features of eyelid skin tumors. A retrospective study of 5504 cases and review of literature. Am. J. Dermatopathol.31, 256–262 (2009).
- ↑ Maeng, M. et al.Bi-institutional retrospective study on the demographics and basic clinical presentation of hidrocystomas. Orbit36, 433–435 (2017).
- ↑ Alfadley, A., Al Aboud, K., Tulba, A. & Mazen Mourad, M. Multiple eccrine hidrocystomas of the face. Int. J. Dermatol.40, 125–129 (2001).
- ↑ Jump up to: 11.0 11.1 11.2 Armstrong, Walsh & Corbett. Multiple facial eccrine hidrocystomas: effective topical therapy with atropine: CORRESPONDENCE. Br. J. Dermatol.139, 558–559 (1998).
- ↑ Meys, R. & Perrett, C. M. Treatment of multiple periocular eccrine hidrocystomata: is botulinum toxin or electrocautery more effective? Clin. Exp. Dermatol.40, 101–103 (2015).
- ↑ Dostrovsky, A. & Sagher, F. Experimentally Induced Disappearance and Re-appearance of Lesions of Hidrocystoma1. J. Invest. Dermatol.5, 167–172 (1942).
- ↑ Clever, H. W. Multiple Eccrine Hidrocystomas: A Nonsurgical Treatment. Arch. Dermatol.127, 422 (1991).
- ↑ Woolery-Lloyd, H., Rajpara, V. & Nijhawan, R. I. Treatment for multiple periorbital eccrine hidrocystomas: botulinum toxin A. J. Drugs Dermatol. JDD8, 71–73 (2009).
- ↑ Tanzi, E. & Alster, T. S. Pulsed Dye Laser Treatment of Multiple Eccrine Hidrocystomas: A Novel Approach. Dermatol. Surg.27, 898–900 (2001).
- ↑ Agarwal, A. & Kumar, D. Giant eyelid eccrine hidrocystoma-induced progressive ptosis in childhood. Indian J. Ophthalmol.65, 884 (2017).
- ↑ Palamar, M., Yaman, B., Akalın, T. & Yağcı, A. Giant Hidrocystoma of the Orbit Presenting with Inversion and Ptosis of the Upper Eyelid. Türk Oftalmol. Derg.47, 113–114 (2017).
- ↑ Desai, A., Mishra, D. K. & Ali, M. J. Large peri-punctal eccrine hidrocystoma. Dermatol. Online J.25, 3