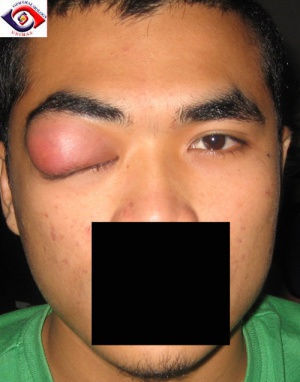
Dacryoadenitis
All content on Eyewiki is protected by copyright law and the Terms of Service. This content may not be reproduced, copied, or put into any artificial intelligence program, including large language and generative AI models, without permission from the Academy.
Disease
Inflammation of the lacrimal gland, either the main or the accessory lacrimal gland, is called dacryoadenitis. Not infrequently, this may be a sign of more sinister pathology underlying the inflammation.
Etiology
Dacryoadenitis may be infectious, idiopathic, autoimmune, or lymphoproliferative in etiology.
Idiopathic dacryoadenitis is the overall most common etiology, accounting for 46-78% of cases, though various studies have found differing ranges. Autoimmune disorders such as Thyroid Eye Disease, IgG4 related orbital disease, sarcoidosis, granulomatosis with polyangiitis, Sjögren’s syndrome, and Churg-Strauss have been associated with dacryoadenitis. Additionally, neoplastic causes such as lymphoma, adenoid cystic carcinoma, or pleomorphic adenoma should be considered.
The most common infectious etiology for dacryoadenitis is viral, specifically, Epstein-Barr virus. Less common viral causes include adenovirus, varicella zoster, herpes simplex, rhinovirus, cytomegalovirus or mumps. Bacterial causes include Staphylococcus aureus, especially methicillin-resistant S. aureus, as well as Streptococcus species. In endemic risk areas, tuberculous infections and abscesses have also been reported.[1]
Risk Factors
Potential risk factors include exposure to viral or bacterial agents or the presence of autoimmune disorders including Sjögren's syndrome, sarcoidosis or IgG4-related disease.
Diagnosis
Symptoms
Symptoms of dacryoadenitis include pain in the superolateral orbit, eyelid edema, pain with eye movements, purulent discharge, droopy upper eyelid or difficulty opening the affected eye, redness of the eye, and occasionally double vision especially in up gaze or lateral gaze. Fever and malaise may be present. Signs of dacryoadenitis include tenderness, edema, erythema or induration overlying the superolateral orbit, lid ptosis, conjunctival injection with or without chemosis, regional lymphadenopathy, proptosis, limitation of ocular motility and rarely visual loss.
Infectious dacryoadenitis presents acutely, with regional or generalized lymphadenopathy, and in 25% of cases with fever. About 40% of patients can have bilateral gland involvement.
Idiopathic dacryoadenitis presents acutely or subacutely, with the majority of patients presenting with pain, erythema of the eyelid, and dry eye. It is typically unilateral, but is bilateral in a minority of cases.[2]
Idiopathic dacryoadenitis presents acutely or subacutely, with the majority of patients presenting with pain, erythema of the eyelid, and dry eye. It is typically unilateral, but is bilateral in a minority of cases.[2]
Diagnostic procedures
A contrast-enhanced computed tomography (CT) scan of the orbits will typically demonstrate enlargement of the affected lacrimal gland with enhancement. There may be associated fat stranding with contiguous involvement of the lateral rectus and /or superior rectus/levator muscle complex. In children and in adults with persistent/recurrent symptoms, Magnetic Resonance Imaging (MRI) of the orbits may also be considered.
If sarcoidosis or other specific orbital inflammatory disorders are suspected, a chest radiograph is a reasonable screening tool to evaluate for lymphadenopathy or pulmonary disease.
Prior to biopsy, corticosteroids should be avoided.
Laboratory tests
Although there are no specific laboratory tests for dacryoadenitis, depending on the clinical context, it may be of use to obtain a complete blood count (CBC) with differential, erythrocyte sedimentation rate (ESR), and/or C-reactive protein (CRP) level to evaluate for leukocytosis and systemic inflammatory response. If secondary to overlying viral conjunctivitis, a conjunctival swab for PCR or cultures may be considered. If autoimmune etiology is suspected, additional labs could include antinuclear antibody (ANA) screen, SS-A/SS-B antibodies, and serum IgG4 level may be requested. In less severe cases when Thyroid Eye Disease is suspected, a thyroid function test panel with autoimmune antibodies may also be requested.
Management
Medical therapy
Depending on the severity of the presentation, therapy could include observation and symptomatic treatment for viral dacryoadenitis. Bacterial dacryoadenitis will require systemic broad spectrum IV or PO antibiotics depending on severity of disease, and when indicated (for example, if there is no improvement after 24 hours of antibiotics), abscess drainage. [3]Oral corticosteroids may be considered especially in idiopathic dacryoadenitis. Refractory cases may benefit from orbital radiation or systemic therapy such as rituximab or methotrexate. Biopsy for tissue diagnosis should be considered if concerned for atypical infections or for refractory disease.
Follow up
Close follow up is warranted if there are orbital signs including decreased visual acuity, pain with eye movements, relative afferent pupillary defect, or abnormal color vision.
Surgery
Although typically reserved for severe or recurrent cases, a trans-septal or trans-conjunctival biopsy of the lacrimal gland may be of diagnostic value if the etiology is in question.[4][5] A detailed histopathologic assessment of the tissue obtained for specific orbital inflammatory disease such as sarcoidosis, IgG4-related disease and for tumors should be performed. During biopsy, debulking may also be attempted for idiopathic dacryocystoadenitis. Large debulking biopsies may be taken, or if there is a well-delineated mass present, the entire mass can be removed. This has been shown to result in full clinical recovery in 80% of 46 patients with an 8% recurrence rate, and the authors recommend first-line treatment with surgery rather than corticosteroids. [6]
When an abscess is suspected clinically or radiologically, drainage should be performed with material sent for stains and microscopy including staining and culturing for acid-fast bacilli.
Complications
The most common complications arise from misdiagnosis or delayed diagnosis of specific lacrimal gland inflammatory or neoplastic pathology. There is limited data on complications of viral dacryoadenitis, however one case series reported ptosis affecting some patients, as well as a measurable (but clinically insignificant) decrease in tear production.[7] When clinical behavior and response is inconsistent with typical clinical course or biopsy non-contributory, a repeat biopsy including representative tissue should be considered.
Prognosis
The prognosis of dacryoadenitis is generally good, with variability depending on the etiology. Viral dacryoadenitis is typically a self-limited disease, whereas idiopathic dacryoadenitis is more heterogeneous. One case series of 79 patients reported poor response to treatment in 37% of patients with idiopathic dacryoadenitis, and recurrent disease in 15% of the patients.[8] The same series found that male sex and inflammation extending to an extraocular muscle were risk factors for incomplete treatment response, and that patients with bilateral dacryoadenitis had an increased risk of recurrent disease.[8]
Additional Resources
Rhem MN, Wilhelmus KR, Jones DB. Epstein-barr virus dacryoadenitis. Am J Ophthalmol 2000;129:372-5.
Foster WJ Jr, Kraus MD, Custer PL. Herpes simplex virus dacryoadenitis in an immunocompromised patient. Arch Ophthalmol 2003;121:911-3.
Obata H, Yamagami S, Saito S, et al. A case of acute dacryoadenitis associated with herpes zoster ophthalmicus. Jpn J Ophthalmol 2003;47:107-9.
Galpine JF, Walkowski J. A case of mumps with involvement of the lacrimal glands. Br Med J 1952;1(4767):1069-70.
Kiratli H, Sekeroglu MA, Soylemezoglu F. Unilateral dacryoadenitis as the sole presenting sign of Wegener's granulomatosis. Orbit 2008;27(3):157-60.
Dutt S, Cartwright MJ, Nelson CC. Acute dacryoadenitis and crohn's disease: Findings and management. Ophthal Plast Reconstr Surg 1992;8(4):295-9.
Witmer, M. (2009, August 13). Unraveling the Difficult Diagnosis of Dacryoadenitis. Retrieved from https://www.reviewofophthalmology.com/article/unraveling-the-difficult-diagnosis-of-dacryoadenitis
References
- ↑ Singh S, Selva D. Non-infectious Dacryoadenitis. Surv Ophthalmol. 2022 Mar-Apr;67(2):353-368. doi: 10.1016/j.survophthal.2021.05.011. Epub 2021 May 31. PMID: 34081929.
- ↑ Jump up to: 2.0 2.1 Mombaerts, I. (2015). The many facets of dacryoadenitis. Current Opinion in Ophthalmology, 26 (5), 399-407. doi: 10.1097/ICU.0000000000000183.
- ↑ Wai KM, Locascio JJ, Wolkow N. Bacterial dacryoadenitis: clinical features, microbiology, and management of 45 cases, with a recent uptick in incidence. Orbit. 2022 Oct;41(5):563-571. doi: 10.1080/01676830.2021.1966813. Epub 2021 Aug 29. PMID: 34455901.
- ↑ Luemsamran P, Rootman J, White VA, Nassiri N, Heran MKS. The role of biopsy in lacrimal gland inflammation: A clinicopathologic study [published correction appears in Orbit. 2018 Apr;37(2):158]. Orbit. 2017;36(6):411-418. doi:10.1080/01676830.2017.1352608
- ↑ Luemsamran P, Rootman J, White VA, Nassiri N, Heran MKS. The role of biopsy in lacrimal gland inflammation: A clinicopathologic study [published correction appears in Orbit. 2018 Apr;37(2):158]. Orbit. 2017;36(6):411-418. doi:10.1080/01676830.2017.1352608
- ↑ Mombaerts I, Cameron JD, Chanlalit W, Garrity JA. Surgical debulking for idiopathic dacryoadenitis: a diagnosis and a cure. Ophthalmology. 2014 Feb;121(2):603-9. doi: 10.1016/j.ophtha.2013.09.010. Epub 2013 Oct 25. PMID: 24572677.
- ↑ Alexandre Robin, Toufic Maalouf, Karine Angioi, Jean-Luc George; Complications after Dacryoadenitis : about 9 cases. Invest. Ophthalmol. Vis. Sci. 2012;53(14):640.
- ↑ Jump up to: 8.0 8.1 Andrew NH, Kearney D, Sladden N, McKelvie P, Wu A, Sun MT, McNab A, Selva D. Idiopathic Dacryoadenitis: Clinical Features, Histopathology, and Treatment Outcomes. Am J Ophthalmol. 2016 Mar;163:148-153.e1. doi: 10.1016/j.ajo.2015.11.032. Epub 2015 Dec 15. PMID: 26701269.