Stye
All content on Eyewiki is protected by copyright law and the Terms of Service. This content may not be reproduced, copied, or put into any artificial intelligence program, including large language and generative AI models, without permission from the Academy.
Disease Entity
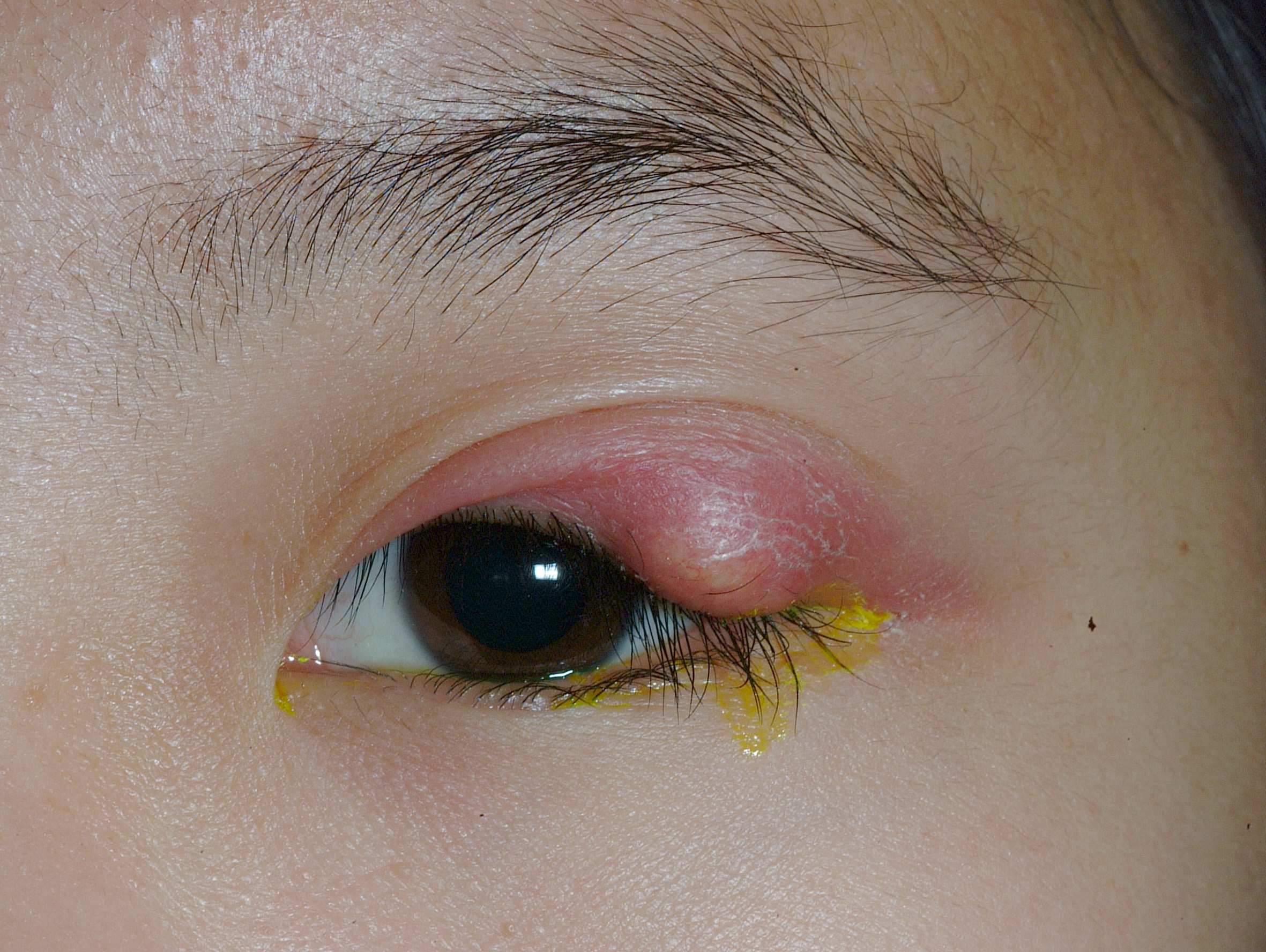
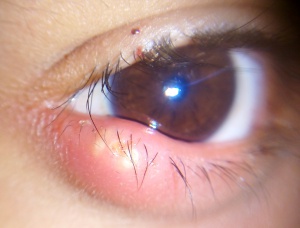
A stye (or hordeolum) is an inflamed oil gland on the margin of the eyelid at the level of the eyelashes or in the midportion of the eyelid. It appears as a red, swollen nodule that resembles a pimple in appearance. It is sometimes tender in its acute presentation, especially to the touch.
Hordeola may be on the external or internal surface of the eyelid and may lead to edema of the entire lid. If they are external, they originate from the glands of Zeiss or Moll. If they are internal, they originate from the meibomian glands.
At times, purulent material is released from the outer eyelash line in external hordeola, while internal hordeola exude on the inner conjunctival surface of eyelid. A stye and chalazion may be referred to synonymously, however, the most accurate descriptions typically refer to a stye as arising from an infectious source, whereas a chalazion manifests from sterile lipogranulomatous inflammation.
Etiology
A stye is caused by an obstruction of a meibomian gland and/or inflammation contributed by normal bacteria or mites (demodex) from the skin of the eyelids. Styes are similar to common acne eruptions that occur elsewhere on the skin. As there are 20-25 meibomian glands on the lower lid and 40-50 on the upper eyelid, patients may have more than one stye at the same time. They commonly develop over a few days and may drain and heal without treatment.
Staphylococcal bacteria are the most common causes of eyelid infections, but other organisms normally found on the skin may be precipitating factors.
Hordeola are found more frequently in patients with dry eyes and chronic blepharitis (eyelid inflammation often related to demodex).
Pathophysiology
Staphylococcus aureus is the bacteria responsible for the majority of cases of hordeola.
An external hordeolum arises from a blockage with secondary inflammation of the Zeiss or Moll sebaceous glands of the eyelid. An internal hordeolum is a secondary inflammatory response of the meibomian glands in the tarsal plate.
Primary prevention
Daily eyelid hygiene with a mild soap and warm water is necessary to reduce the incidence of styes. Eyelid and face make-up should be removed completely before going to sleep.
It is important to wash hands thoroughly before touching the skin around the eye. Patients who are susceptible to styes should carefully clean excess oils from the eyelid margin. Commercial eyelid scrubs are available and may be recommended by an eye doctor as primary prevention for styes. These are especially useful if the diagnosis of a demodex infection has been made.
Diagnosis
History
Patients usually report a localized painful swelling of one or more eyelids. In some cases, the complaint may start as a generalized edema and erythema of the lid that later becomes localized.
A history of previous similar presentations is common.
Changes in vital signs and systemic symptoms are extremely rare in the presentation of a hordeolum and presentation with such symptoms should warrant investigation into cellulitis or another disease entity.
In extreme cases, the condition may spread to involve the entire eyelid and even the adjacent facial tissues. These cases do not respond to conservative hordeolum management and must be treated as periorbital cellulitis, requiring oral and/or IV antibiotics.
Physical examination
A complete examination of the periocular area, the eye, and the conjunctival surface should be performed. Eyelid eversion can be performed to visualize a posterior hordeolum
Examination reveals a localized, tender, erythematous, elevated area with a pointing eruption either on the inner or outer side of the eyelid.
Palpation of adjacent lymph nodes can help to identify spread of the disease beyond an uncomplicated eyelid lesion. Lymph nodes should not be involved in patients with a simple hordeolum.
Visual acuity, slit lamp, and dilated fundoscopic exam is necessary to rule-out extension of eyelid pathology.
Differential diagnosis
- Chalazion
- Carcinoma
- Oil gland cyst /Tarsal cyst
- Xanthelasma
- Papilloma
- Pyogenic Granuoloma
- Amyloid Deposition
Management
Consultation with an ophthalmologist or ophthalmic plastic surgeon is necessary for appropriate diagnosis and management.
Medical therapy
Styes may be treated by applying warm compresses to the eyelid several times per day. This helps to accelerate drainage of the lesion. Antibiotic ointments or drops with concomitant steroid may help styes resolve more quickly. Regular follow-up with an ophthalmologist is necessary to chronicle regression and monitor side effects from medications. If the stye has been longstanding or manifests as a chalazion, injection of triamcinolone (Kenalog) can help in resolving the lesion, although this carries the small risks of skin deposition of the steroid, necrosis, subcutaneous fat atrophy, embolic visual loss, incomplete resolution and need for surgical removal, as well as skin hypo-pigmentation or hyper-pigmentation (particularly in patients with darker skin tones).
Surgery
A stye will typically be self limiting and resolve without requiring surgery. However, chalazion may not resolve with conservative or medical measures and require incision and drainage.
Complications
Cosmetic deformity and visual disturbance are the most common complications of styes.
If left untreated, styes may rarely lead to more widespread infections that involve the periorbital tissues. Also, stye recurrence is common especially if a prophylactic daily lid hygiene is not maintained.
Additional Resources
- Turbert D, Gregori NZ. Eyelashes. American Academy of Ophthalmology. EyeSmart/Eye health. https://www.aao.org/eye-health/anatomy/eyelashes. Accessed March 07, 2023.
- Porter D, Mendoza O, Turbert D. Inflammation. American Academy of Ophthalmology. EyeSmart/Eye health. https://www.aao.org/eye-health/symptoms/inflammation. Accessed March 07, 2023.
References
- http://emedicine.medscape.com/article/798940-overview
- Orbit, Eyelids, and Lacrimal System. BCSC Section 7. American Academy of Ophthalmology. 2008.
- Techniques in Ophthalmic Plastic Surgery with DVD: A Personal Tutorial. Jeffrey A. Nerad MD. Saunders 2010.
- Silkiss, RZ, Paap, MK, Ugradar, S, The Association between Mask Wear and Chalazion Formation during the Covid-19 Pandemic, AJO Case Reports, 2020.