Image Guided Navigation for Orbital Surgery
All content on Eyewiki is protected by copyright law and the Terms of Service. This content may not be reproduced, copied, or put into any artificial intelligence program, including large language and generative AI models, without permission from the Academy.
Overview
Image-guided surgical navigation (ISN) is a useful tool in orbital surgery which allows for 3-dimensial (3D) localization of the surgeon’s instruments within a confined space which holds important vascular and neural structures. It has long been used in surgical specialties beyond oculofacial plastic surgery. First employed by neurosurgeons to aid in tumor localization, the use of ISN has since expanded to otolaryngology, dental, spinal and now more recently orbital surgery.[1] Intraoperative navigation relies on the principle of stereotaxy, whereby external markers are used as a reference point, allowing for three planes of visualization to localize internal surgical/anatomical landmarks. Stereotactic surgery enables the surgeon to precisely direct surgical instruments or radiation towards a specific area thereby improving surgical precision, instrumentation and reducing intra-operative complication rates.[2]
Image-guided surgical navigation has been used in orbital surgery to aid in pre-operative planning, allowing the surgeon to determine the most minimally invasive route that would yield the least collateral damage to surrounding tissue. Navigation assistance also enables the surgeon to account for any possible anatomical variations or incidental findings that may complicate the surgery.
Principles
Conceptually, ISN is analogous to global positioning systems used in vehicles and smart phones.
ISN involves the following components:
- Imaging data set: Pre-operative imaging in the form of contiguous CT/MRI imaging series are required to allow for accurate calibration of image-guidance equipment. The set of images is then uploaded to the navigation software to create a 3D map of the patient’s anatomy.
- Localizers: This comprises of an emitter (infrared or electromagnetic) and a patient tracker (usually a headband) that communicate with one another to convert the position of the sensors into relative coordinates. Positioning of all components is essential to allow for free signal transfer between.
- Surgical instrument or probe: The signal emitted localizes the probe on the 3D map relative to the tracker. Conceptually, ISN is analogous to global positioning systems used in vehicles, with the imaging data set representing the “map”, the localizers (emitter and tracker), representing the satellite and tower, and the probe representing the “car”.
Modalities
At present, there are two main modalities for intraoperative navigation, optical (infrared) and electromagnetic-guided navigation.
- Optical (Infrared) Navigation: A light source or infrared cameras emit a beam which is reflected between sensors fixed to the patient’s head in the form or a headband or stickers and sensors fixed to the navigation probe. This approach requires a line of sight between the emitter and the sensors and is more costly.
- Electromagnetic Navigation: An electromagnetic field emitter transmits an electromagnetic field with the headband or metallic electric beads on the patient’s head acting as reference points for the navigation probe. This approach does not require a line of sight between the emitter and the sensors, and is less costly. The presence of other metal instruments or implants in the patient (pacemaker, cochlear implants) can cause ferromagnetic interference and lead to inaccuracies, necessitating the need for Titanium instruments.
Uses
General Indications [1]
- Real-time anatomic localization during surgery
- Hardware/graft placement confirmation
- Orbital tumor localization
- Virtual surgical planning
- Resident education[3]
Orbital Decompression
Orbital decompression is a procedure that aims to relieve proptosis compression on the optic nerve by removing a portion of bone or the orbital wall and thereby expand the orbital volume. ISN has proven advantageous in complex cases that require 3-wall decompression, cases of subtotal decompression that require reoperation, and cases with anomalous variations in orbital anatomy. Depending on the surgical approach, CSF rhinorrhea, infraorbital nerve injury, and post-operative diplopia are potential complications.[4][5][6] Numerous approaches have been proposed to find a balance between the competing factors of pre-operative proptosis, post-operative diplopia and cosmetic outcomes. In a case series of seven patients with thyroid eye disease (TED)-related proptosis there was a mean reduction in proptosis of 9.36 mm with no intra-post-operative complications 6 months after stereotactic-guided balanced (medial and lateral wall) orbital decompression.[7] The use of image guided orbital navigation may assist the surgeon in achieving confident and safe surgery. In one study that included 45 endoscopic orbital decompression surgeries the authors used image guided navigation in all cases and were able to reduce diplopia with a technique preserving the inferomedial orbital bone strut.[8]
Optic Canal Decompression
Optic canal decompression (OCD) is performed in cases of traumatic optic neuropathy; however, localization can be a challenge with the transcaruncular approach. Inadvertent injury to surrounding structures and the optic nerve are possible complications. INS provides improved precision, safety and positional orientation. Various reports have highlighted the role of ISN in presurgical planning of cases with traumatic optic neuropathy associated with optic canal fractures due to the difficult visualization of the disturbed anatomy. INS has allowed for improved post-operative visual outcomes in patients with optic canal fractures with owing to improved precision when navigating within the orbit thereby limiting iatrogenic injury to the optic nerve.[9][10]
Orbital Reconstruction
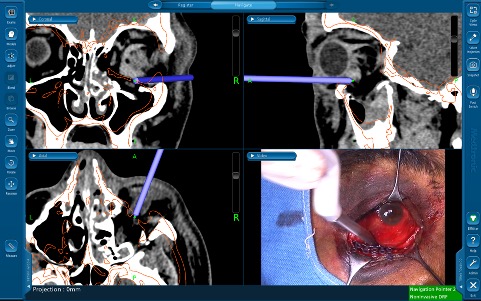
Orbital reconstruction aims to replicate the dimensions of the orbit prior to the traumatic event. The unaffected contralateral orbit is commonly used as a template when planning the procedure. Surgical navigation has risen as viable method for the measurement of orbital volume and dimensions. Markiewicz et al. found high reliability between the pre-operative unaffected and postoperative affected orbital volumes in 23 subjects who underwent orbital reconstruction with ISN.[11] Orbital reconstruction of post-traumatic and tumor ablation deformities poses the challenge of post-operative orbital asymmetry resulting in functional and cosmetic disturbances including enophthalmos. First described by Gellrich[12], the use of ISN has enhanced pre-operative planning for orbital reconstruction. Allowing for prediction of surgical steps to ensure avoidance of vulnerable structures (i.e. optic nerve), pre-planning of bone graft position and orbital frame contouring. Complex reconstructions that require sheet implantation can be challenging due to the poor visualization of key anatomical landmarks within the orbit resulting in residual enophthalmos and limitations in motility. ISN allows for real-time intraoperative measuring of the implant and symmetrization resulting in more predictable outcomes.[13]
Orbital Tumor Resection
Intraoperative navigation has proven helpful the surgical resection of orbital tumors by providing accurate localization and identifying tumor margins. In a retrospective study of 23 patients with orbital tumors, 19 of which were meningiomas, ISN altered the surgical approach in 52% of patients due to the intra-operative finding of residual tumors after initial resection.[14] The use of ISN can be limited by the inaccuracy of pre-operative scans after resection and extensive manipulation of structures results in a shift or distortion of the pre-operative anatomy.
Orbital Foreign Body Exploration
Few reports in the literature exist of the use of ISN for the removal of orbital foreign bodies.[15][16][17] The utility of INS in orbital foreign body exploration and removal is if the surgeon is able to determine the optimal site for surgical incision to minimize depth of incision and any accompanying collateral damage to surrounding tissue. In a retrospective study of 30 patients who underwent image-guided removal of orbital metallic foreign bodies, there was no significant difference between the preoperative and intraoperative depth of foreign body (20.02 vs 19.98 mm).[18]
Summary
ISN is a useful adjunct in various types of orbital surgery. At present, it is not the current standard of care but with the growing popularity of this technology and the advancement of surgical techniques, ISN will continue to prove an advantageous tool for orbital surgeons.
- ↑ Roberts, D.W., et al., A frameless stereotaxic integration of computerized tomographic imaging and the operating microscope. Journal of Neurosurgery, 1986. 65(4): p. 545-549.
- ↑ Soteriou, E., et al., Prospects and limitations of different registration modalities in electromagnetic ENT navigation.European Archives of Oto-Rhino-Laryngology, 2016. 273(11): p. 3979-3986.
- ↑ Davis KS, Vosler PS, Yu J, Wang EW. Intraoperative Image Guidance Improves Outcomes in Complex Orbital Reconstruction by Novice Surgeons. J Oral Maxillofac Surg. 2016 Jul;74(7):1410-5. doi: 10.1016/j.joms.2016.02.023. Epub 2016 Mar 3. PMID: 27019413.
- ↑ Goldberg, R.A., et al., Strabismus after balanced medial plus lateral wall versus lateral wall only orbital decompression for dysthyroid orbitopathy. Ophthalmic Plast Reconstr Surg, 2000. 16(4): p. 271-7.
- ↑ De Santo, L.W., Transantral orbital decompression. The eye and orbit in thyroid disease, 1984.
- ↑ Mainville, N.P. and D.R. Jordan, Effect of orbital decompression on diplopia in thyroid-related orbitopathy. Ophthalmic Plast Reconstr Surg, 2014. 30(2): p. 137-40.
- ↑ Millar, M.J. and A.J. Maloof, The application of stereotactic navigation surgery to orbital decompression for thyroid-associated orbitopathy. Eye (Lond), 2009. 23(7): p. 1565-71.
- ↑ Finn, Avni P. M.D., M.B.A.*; Bleier, Benjamin M.D.†; Cestari, Dean M. M.D.‡; Kazlas, Melanie A. M.D.§; Dagi, Linda R. M.D.§; Lefebvre, Daniel R. M.D.‖; Yoon, Michael K. M.D.‖; Freitag, Suzanne K. M.D.‖. A Retrospective Review of Orbital Decompression for Thyroid Orbitopathy with Endoscopic Preservation of the Inferomedial Orbital Bone Strut. Ophthalmic Plastic and Reconstructive Surgery 33(5):p 334-339, September/October 2017. | DOI: 10.1097/IOP.0000000000000782
- ↑ Bhattacharjee, K., et al., Navigation-guided optic canal decompression for traumatic optic neuropathy: Two case reports.Indian J Ophthalmol, 2018. 66(6): p. 879-882.
- ↑ Yan, W., et al., Incidence of optic canal fracture in the traumatic optic neuropathy and its effect on the visual outcome. Br J Ophthalmol, 2017. 101(3): p. 261-267.
- ↑ Markiewicz, M.R., et al., Reliability of intraoperative navigation in restoring normal orbital dimensions. J Oral Maxillofac Surg, 2011. 69(11): p. 2833-40.
- ↑ Gellrich, N.C., et al., Computer-assisted secondary reconstruction of unilateral posttraumatic orbital deformity. Plast Reconstr Surg, 2002. 110(6): p. 1417-29.
- ↑ Schmelzeisen, R., et al., Navigation-aided reconstruction of medial orbital wall and floor contour in cranio-maxillofacial reconstruction. Injury, 2004. 35(10): p. 955-62.
- ↑ Terpolilli, N.A., et al., Orbit-associated tumors: navigation and control of resection using intraoperative computed tomography. Journal of Neurosurgery JNS, 2016. 124(5): p. 1319-1327.
- ↑ Ali, M.J., et al., Interactive navigation-guided ophthalmic plastic surgery: the techniques and utility of 3-dimensional navigation. Can J Ophthalmol, 2017. 52(3): p. 250-257.
- ↑ Liu, Z., et al., Endoscopic-assisted navigation-guided removal of long-standing metallic foreign body near to the sphenoid. J Craniofac Surg, 2015. 26(2): p. e122-4.
- ↑ Promsopa, C. and U. Prapaisit, Removal of intraconal bullet through endoscopic transnasal surgery with image-guided navigation system 8 months after injury: a case report. Journal of Medical Case Reports, 2019. 13(1): p. 65.
- ↑ Zhao, Y., et al., Removal of Orbital Metallic Foreign Bodies With Image-Guided Surgical Navigation. Ophthalmic Plast Reconstr Surg, 2020. 36(3): p. 305-310.

