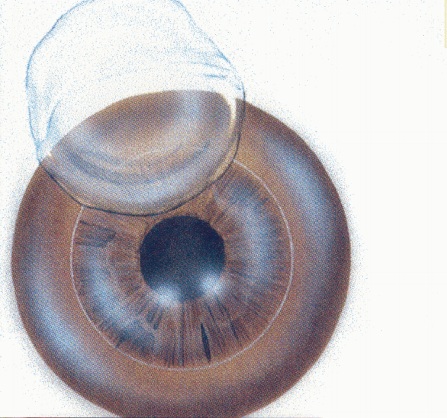
Free Cap after LASIK
All content on Eyewiki is protected by copyright law and the Terms of Service. This content may not be reproduced, copied, or put into any artificial intelligence program, including large language and generative AI models, without permission from the Academy.
Introduction
Free cap is a rare intra-operative complication of LASIK (laser in situ keratomileusis). Ideally in LASIK, a hinged corneal flap is created that allows the excimer laser to be applied on the exposed stromal bed. If the hinge of the corneal flap detaches, the flap becomes a free cap. The occurrence of this complication is most commonly associated with the use of a microkeratome on flat corneas, which predisposes to small flap diameter. Free caps are preventable and treatable. Rarely does the complication lead to severe or permanent decrease in visual acuity.[1]
Free Cap
Incidence
The incidence of free cap during microkeratome LASIK is generally low, ranging from 0.004% to 1.31% depending on the study[1][2][3].
Risk Factors
Risk factors for free cap are generally anatomic or mechanical.
- Use of mechanical microkeratome rather than femtosecond microkeratome [4]
- Flat cornea (<40.00D) [4][5][6]
- Deep orbits
- Inadequate suction
- Decentered ring placement
- Faulty microkeratome blades
- Stopper set for smaller hinge [5]
Prevention
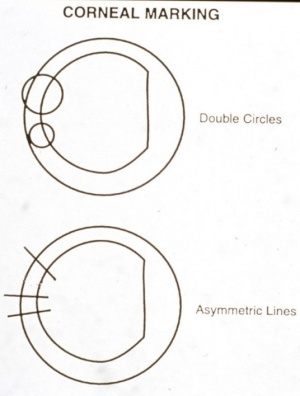
As free caps are avoidable, prevention is critical. Proper selection of ring and stop size based on keratometry values, ensuring adequate suction, and re-docking the microkeratome if necessary are critical preventive measures. [7] Prior testing of the microkeratome and ensuring good verbal anesthesia are important steps. [7] The first step in prevention is selecting suction rings of larger diameter (for example: Hansatome or a larger microkeratome head such as a 9.5mm ring on Nidek MK-2000) for flat corneas less than 42D and avoid flap creation on corneas <38D. [8] For the new surgeon, stop rings can be helpful to prevent a full pass through the cornea.[9] Care must be taken during ring centration, and the stopper of the microkeratome should be calibrated. Placing epithelial reference markings (see figure) can be useful in the event that a free cap does arise to ensure that the flap is reapplied in the proper position.
According to a study by Jacob et al., the incidence of the complication varied significantly when Hansatome (Bausch & Lomb Surgical) was compared to Automated Corneal Shaper® (Chiron Vision Corp.), favoring Hansatome for lower rates of free cap and other microkeratome-related complications.[3] Superiority of Hansatome in preventing free cap complication was confirmed in a study by Nakano et al. [10]. In a different study, Hansatome had equivalent rates of free cap complication compared to Moria LSK2 (Moria SA, Anthony, France)[11].
A comprehensive video guide for novice surgeons performing microkeratome LASIK, emphasizing these preventive and management strategies can be found elsewhere. [7]
Management
If a free cap is created, the surgeon must decide whether to continue with excimer laser ablation or to abort the procedure.
- When to abort: If the stromal bed is irregular, replace the flap without applying laser ablation. Without ablation, generally, there is no change in refractive error or significant loss of visual acuity [12][7]
- When to continue: If the stromal bed is regular and the cap is of normal thickness, the surgeon may proceed with ablation. The free cap should be carefully handled by being placed on a drop of balanced salt solution to prevent desiccation.[7]
The free cap should be placed epithelial side up, often with a bandage contact lens. The endothelial cell pump mechanism typically allows the cap to re-adhere tightly. Pre-marking the cornea allows for placement in the correct axis to avoid postoperative irregular astigmatism.
Complications
- Loss of the disc: One of the most feared complications of the free cap is the loss of the disc after replacement of the disc. To avoid this complication, for approximately 30 minutes after surgery, the lids may be closed using two crossed adhesive strips.[13] Dislocated disc has been reported to be repositioned with good visual outcome as much as four days after the initial surgery.[14]
- Astigmatism: Incorrect flap orientation likely causes irregular astigmatism. Corneal markings placed before the flap is lifted would help to place the free cap back to its original anatomic position. Treatment for this complication includes removing and repositioning the cap if the proper orientation is known, repeating LASIK with a deeper flap after 6+ months, or placing a homoplastic cap about 200 micrometers thick[15].
- Epithelialization of the interface: It is often impossible to differentiate between the epithelial and stromal sides of the disc. If the disc is placed with the epithelial side down, the interface may epithelialize, leading to loss of the disc.
- Epithelial ingrowth
- Flap micro/macrostriae
- Loss of best corrected vision
References
- ↑ 1.0 1.1 Lin RT, Maloney RK. Flap complications associated with lamellar refractive surgery. Am J Ophthalmol. 1999 Feb;127(2):129-36.
- ↑ Boutin, T, Adiguzel Eser, Wallerstein Avi, Cohen M, Harissi-Dagher M. Incidence and outcomes of LASIK free cap. American Society of Cataract and Refractive Surgery. Abstract/Poster. 2011.
- ↑ 3.0 3.1 Jacobs JM, Taravella MJ. Incidence of intraoperative flap complications in laser in situ keratomileusis. J Cataract Refract Surg. 2002 Jan;28(1):23-8.
- ↑ 4.0 4.1 Skuta GL, Cantor LB, Weiss JS, et al. Basic and Clinical Science Course, section 13: Refractive surgery. American Academy of Ophthalmology. 2012 p104.
- ↑ 5.0 5.1 Buratto, Lucio, and Stephen F. Brint. LASIK: Surgical Techniques and Complications. 2nd ed. Thorofare, NJ: SLACK, 2000. Print.
- ↑ Krachmer, Jay H., Mark J. Mannis, and Edward J. Holland. Cornea. 3rd ed. Vol. 2. St. Louis, MO: Mosby/Elsevier, 2011. Print.
- ↑ 7.0 7.1 7.2 7.3 7.4 Paryani M, Israni N, Kochar S, Aggarwal K. Microkera to mechronicles : Management of a free flap. Indian J Ophthalmol. 2023 Jul;71(7):2926-2927.
- ↑ Bowman, R. Wayne. "Complications of Refractive Surgery." University of Texas Southwestern Med Ctr, Dallas, Texas. Jan. 2014. Lecture.
- ↑ Brightbill, Frederick S. Corneal Surgery: Theory, Technique & Tissue, Chapter 96. 3rd ed. St. Louis, MO: Mosby, 1999. Print.
- ↑ Nakano K, Nakano E, Oliveira M, Portellinha W, Alvarenga L. Intraoperative microkeratome complications in 47,094 laser in situ keratomileusis surgeries. J Refract Surg. 2004 Sep-Oct;20(5 Suppl):S723-6.
- ↑ Al-Mezaine HS, Al-Amro SA, Al-Obeidan S. Intraoperative flap complications in laser in situ keratomileusis with two types of microkeratomes. Saudi J Ophthalmol. 2011 Jul;25(3):239-43.
- ↑ Tham VM, Maloney RK. Microkeratome complications of laser in situ keratomileusis. Ophthalmology. 2000 May;107(5):920-4.
- ↑ Buratto, Lucio, and Stephen F. Brint. CUSTOM LASIK: Surgical Techniques and Complications. Thorofare, NJ: Slack, 2003. Print.
- ↑ Cheng AC, Wong VW, Rao SK, Lam DS. Repositioning of free cap four days after LASIK. J Refract Surg. 2007 Jun;23(6):625-7.
- ↑ Kwitko ML, Kremer FB, Lee NT, Wachler BSB, Koch DD, Chu YR, Alphis N, Hovanesian J, Shah S, Maloney R. Induced astigmatism following laser in situ keratomileusis for myopia with a free cap. J Refract Surg. 2000 May-Jun;16(3):375-9.