All content on Eyewiki is protected by copyright law and the Terms of Service. This content may not be reproduced, copied, or put into any artificial intelligence program, including large language and generative AI models, without permission from the Academy.
Eight-and-a-half syndrome describes a constellation of symptoms that occur due a lesion involving the abducens (cranial nerve (CN) VI) nucleus, the fascicular portion of the facial (CN VII) nerve, and the medial longitudinal fasciculus (MLF). This results in a combination of horizontal gaze palsy, facial nerve palsy, and internuclear ophthalmoplegia (INO).
Neuroanatomy
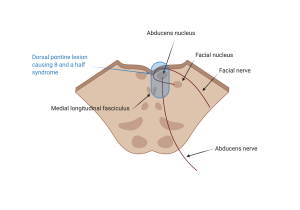
The abducens nucleus resides in the dorsal pons. Medial to the CN VI nucleus lies the MLF, a heavily myelinated nerve tract connecting the paramedian pontine reticular formation (PPRF) and CN VI to the oculomotor nucleus (CN III) on the contralateral side. The facial (CN VII) nucleus also lies nearby in the dorsal pons and the CN VII fascicle moves posteriorly to wrap around the abducens nucleus before exiting the pons. Lesions to the abducens nucleus result in ipsilateral horizontal gaze paresis. Lesions to the MLF result in an internuclear ophthalmoplegia (INO).
One-and-one-half syndrome describes a lesion that involves the abducens nucleus, PPRF, and MLF ipsilaterally. This results in a conjugate horizontal gaze palsy in one direction and an INO in the other direction. Lesions to the facial nerve fascicle result in an ipsilateral lower motor neuron facial palsy (which involves the forehead, compared to upper motor neurone facial nerve palsies which are forehead sparing). Combining a One-and-a-half syndrome with a lesion to the ipsilateral facial nerve fascicle nearby is dubbed “Eight-and-a-half syndrome” (CN 7 + 1.5). Eight-and-a-half syndrome localizes to the dorsal tegmentum of the caudal pons.[1] The etiology is most commonly a vascular or demyelinating lesion.[1]
Disease
Eight-and-a-half syndrome presents with an ipsilateral conjugate horizontal gaze palsy and ipsilateral INO, and an ipsilateral lower motor neuron facial nerve palsy. This leaves the only remaining horizontal eye movement being contralateral abduction.[2] [3]
Etiology
The condition is often caused by a lesion (vascular or demyelinating) in the dorsal tegmentum of the caudal pons. Blood supply to this area is derived from paramedian pontine arteries, which usually supply the corresponding side of the midline.[4] Individual case reports have also reported other causes including cavernomas[5] and neoplasms[6]
Diagnosis
Eight-and-a-half syndrome is largely a clinical diagnosis, however brainstem magnetic resonance imaging (MRI) with and without contrast can provide suggestions regarding the underlying etiology. For example, a lesion that is hyperintense on diffusion weighted imaging (DWI) and hypointense on apparent diffusion coefficient (ADC) imaging may suggest a stroke. Other findings on MRI may be more suggestive of other etiologies, and lesions can sometimes be detected even if only a few millimeters in size.[4]
Prognosis
The overall prognosis is in part based on the underlying etiology. Generally, diplopia and facial palsy in cases of isolated eight-and-a-half syndrome has a good prognosis, with abduction weakness typically persisting longer than adduction weakness.[2]
References
- ↑ 1.0 1.1 Eggenberger E. Eight-and-a-Half Syndrome. Journal of Neuro-Ophthalmology. 1998;18(2):114???116. doi:10.1097/00041327-199806000-00008
- ↑ 2.0 2.1 Bocos-Portillo J, Ojeda JR, Gomez-Beldarrain M, Vazquez-Picon R, Garcia-Monco JC. Eight-and-a-Half Syndrome. JAMA Neurol. 2015;72(7):830. doi:10.1001/jamaneurol.2015.0255
- ↑ Fitzgerald MJT, Gruener G, Mtui E, eds. Clinical Neuroanatomy and Neuroscience. 6th ed. Philadelphia, PA: Saunders Elsevier; 2012:198-215.
- ↑ 4.0 4.1 Sarwal A, Garewal M, Sahota S, Sivaraman M. Eight-and-a-Half Syndrome. Journal of Neuroimaging. 2009;19(3):288-290. doi:10.1111/j.1552-6569.2008.00261.
- ↑ Reyes, Karen & Mesina, Bryan & Sousan, George. (2018). Eight-and-a-half-syndrome: a rare potentially life-threatening disease. GMS Ophthalmology Cases. 8. 10.3205/oc000086.
- ↑ Van Toorn R, Schoeman JF, Donald PR. Brainstem tuberculoma presenting as eight-and-a-half syndrome. Eur J Paediatr Neurol. 2006 Jan;10(1):41-4. doi: 10.1016/j.ejpn.2005.11.003. Epub 2006 Mar 10. PMID: 16529962.