Conjunctival Melanocytic Tumors
All content on Eyewiki is protected by copyright law and the Terms of Service. This content may not be reproduced, copied, or put into any artificial intelligence program, including large language and generative AI models, without permission from the Academy.
Disease Entity
Conjunctival melanocytic tumors comprise benign and malignant neoplasms.
Nevi are congenital benign melanocytic tumors that can be further classified into junctional, subepithelial, compound, and blue nevus as well as congenital melanocytosis. In the text, the term “nevus” refers to the most common form of nevi, the compound nevus (a nevus with a junctional and a subepithelial component).
Primary acquired melanosis (PAM) can either be regarded as benign (PAM without atypia) or represent a precancerous lesion (PAM with atypia), whereas a melanoma is per definition a malignant melanocytic tumor.
Diagnosis
Patients usually present for an eye examination when they recognize a new lesion or growth of a preexisting lesion.
Clinical diagnosis
The clinical diagnostic process comprises slit lamp and fundus examination, ultrasound or anterior segment OCT (if necessary), and photo-documentation. Conjunctival melanocytic lesions are typically various shades of brown, but can appear amelanotic or pink. They can be flat- typically a nevus or PAM- or nodular which is more worrisome for a melanoma.
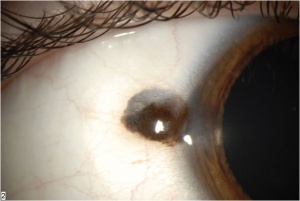
Nevi (Fig.1A) exhibit usually cysts (that can be detected on slit lamp examination and with sonography/anterior segment OCT) and are reported by the patient to exist for a long time (as they are congenital). Conjunctival nevi are the most common melanocytic conjunctival tumors. They are more common in Caucasians and appear within the first two decades of life. They are typically located in the interpalpebral conjunctiva near the limbus and rarely involve the cornea. If a pigmented lesion is seen on the palpebral conjunctiva, plica, or caruncle then one must consider PAM or melanoma. Nevi can change color and size during adolescence but if change is seen in an adult then this should raise suspicion for malignancy. The overall risk of malignant transformation is 1%.
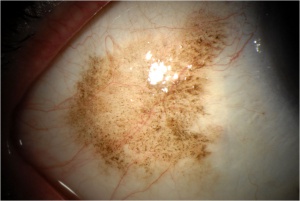
PAM (Fig. 2A)
usually occurs in middle-aged or elderly individuals (mostly Caucasians) and is almost always unilateral. PAM appears clinically as a flat and variably brown conjunctival lesion ranging from light tan to dark brown colored. The lesion may involve any area of the conjunctiva and can be continuous or separated by normal conjunctiva. It is important to evert the eyelids as PAM can hide in the fornix and on the palpebral conjunctiva. In some cases with diffuse PAM, the eyelid epidermis may be involved.
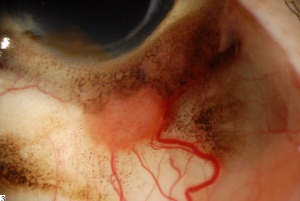
Conjunctival melanomas (Fig. 3) may arise from PAM (most common), nevi, or de novo. According to one study, 71% of conjunctival melanomas were associated with PAM with atypia and 17% arose from a nevus. When conjunctival melanoma arises from a nevus or de novo it appears as a solitary pigmented or amelanotic smooth vascular nodule, commonly in the limbal area. Increased vascularity and adherence to the underlying sclera may be present. Melanomas are more frequently observed in Caucasians and exhibit a nodular or diffuse growth. Suspicious need to be completely excised and submitted for histopathological investigation. Once the diagnosis is confirmed, systemic work-up is required.
Inspection of all ocular structures is mandatory as multicentric lesions can occur, especially if associated with PAM. Lesions consisting of PAM and melanoma are also not uncommon (especially as a melanoma can arise in PAM), thus all suspicious lesions have to be excised and submitted for histopathological investigation.
Histologic diagnosis
A nevus (Fig. 1B, C) typic
ally consists of nests of nevus cells that are present in the junctional and subepithelial area of the conjunctiva. Conjunctival inclusion cysts are characteristic for nevi and may be observed clinically.
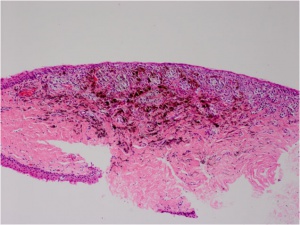
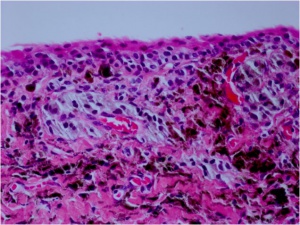
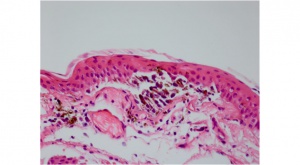
A PAM (Fig. 2B) without atypia is best characterized by minimal melanocytic hyperplasia along the basal epithelial layer of the conjunctival. PAM with atypia shows usually isolated or confluent nests of atypical melanocytes. Pagetoid spread can also be observed. The melanocytes exhibit varying signs of atypia as large abnormal cells, prominent nucleoli, a high nuclear-cytoplasmic ratio, and mitotic figures.
A conjunctival malignant melanoma shows invasion of melanoma cells into the subepithelial layers. The cells exhibit the above named signs of atypia. Remnants of PAM or nevus may be found in or contiguous to the melanoma.
There are some lesions that cannot be unequivocally assigned to a nevus, PAM, melanoma. These lesions are best classified as “Indeterminate melanocytic proliferations of the conjunctiva”.
The American Academy of Ophthalmology's Pathology Atlas contains virtual microscopy images of the following:
Differential diagnosis
- Complexion associated melanosis
- Nevus
- Primary acquired melanosis
- Pigmented Axenfeld loop
- Malignant melanoma
- Secondary pigmentation
- Extension of a pigmented intraocular tumor to subconjunctival region
- Conjunctival foreign body
- Conjunctival argyrosis
- Exogenous pigmentation (e.g. mascara)
Management
Treatment
Nevi may be excised when growth or change in color is noted. These changes do not necessarily - but can - indicate the development of a melanoma as hormonal changes, inflammation or even growth of the mucinous inclusion cysts can be mostly accused for these changes. In most cases nevi can just be followed including photo-documentation.
Lesions suspicious for PAM should be carefully biopsied (incisional, excisional, or map biopsy using a “dry” technique) allowing for histological examination. Dependent on the clinical impression, the surgical margins can be treated with cryotherapy. Treatment with topical mitomycin or interferon alpha 2b can be considered for histology-proven PAM with atypia including residual lesions - but only for lesions confined to the epithelium as these local treatment strategies are not proper for melanomas.
The primary treatment of conjunctival melanoma is excision of the entire tumor with wide surgical margins of 3-5mm. If there is scleral involvement then scleroconjunctivectomy should be considered. A "dry" technique (throw the BSS of the surgical field) should be employed so that cells are not spread to other areas of conjunctiva. A "no touch" technique should also be used taking care not to touch any cancerous cells with surgical instruments which could also spread cells. Most surgeons will also add an adjuvant therapy to primary excision including cryotherapy in a double freeze thaw fashion to the base and edges. Areas of PAM with atypia must be treated as they can be origin of a recurrence of the melanoma. MMC can be added after surgery to help prevent a recurrence although there are severe side effects that must be discussed with the patient. If a wide excision is performed, a membrane graft will be needed in the form of either amniotic membrane available off the shelf or a mucous membrane graft from the oral mucosa. Sentinel lymph node biopsy should be considered for lesions thicker than 2 mm. Given that conjunctival melanoma is genetically similar to cutaneous melanoma, targeted therapies such as BRAF inhibitors and KIT inhibitors may be effective in the treatment of patients with metastatic conjunctival melanoma.
Follow up
Nevi are usually stationary but can exhibit growth due to hormonal changes or local inflammation. They should be observed for growth or change in color. PAM without atypia may be followed by observation.
PAM with atypia require - after treatment - periodical follow-up by an experienced ophthalmologist to rule out recurrence or progression into melanoma.
Patients with conjunctival melanoma should be periodically followed and investigated for local recurrence. Systemic work-up is also mandatory as the mortality is about 25%.
Prognosis
Nevi are congenital lesions and only a small percentage progress into malignant melanoma.
PAM with atypia has a high likelihood to progess into malignant melanoma in contrast to PAM without atypia.
Conjunctival melanomas have a risk (20-50%) of local recurrence. Melanoma-related mortality at 10 years ranges from 13 to 38%. Lesions that involve the fornix or the palpebral conjunctiva have a higher risk for metastasis and locally aggressive disease than bulbar lesions. Caruncular disease has the worst outcome, may infiltrate the orbit, and is associated with 50% mortality at 3 years. An increased mortality is also seen with lesions thicker than 2 mm. Melanomas arising de novo seem to carry a higher risk of metastasis and death compared with those cases arising from PAM or nevus.
Additional Resources
- www.atlasophthalmology.com
- www.eyecancer.com
- Boyd K, Vemulakonda GA. Nevus. American Academy of Ophthalmology. EyeSmart/Eye health. https://www.aao.org/eye-health/diseases/nevus-list. Accessed March 19, 2019.
References
- Damato B, Coupland SE. Management of conjunctival melanoma. Expert Rev Anticancer Ther. 2009;9(9):1227-39.
- Grossniklaus HE, Margo CE, Solomon AR. Indeterminate melanocytic proliferations of the conjunctiva. Trans Am Ophthalmol Soc. 1999;97:157-70.
- Shields CL. Conjunctival melanoma: risk factors for recurrence, exenteration, metastasis, and death in 150 consecutive patients. Trans Am Ophthalmol Soc. 2000;98:471-92.
- Shields JA, Shields CL, Mashayekhi A, Marr BP, Benavides R, Thangappan A, Phan L, Eagle RC Jr. Primary acquired melanosis of the conjunctiva: experience with 311 eyes. Trans Am Ophthalmol Soc. 2007;105:61-72.
- Shields CL, Markowitz JS, Belinsky I, Schwartzstein H, George NS, Lally SE, Mashayekhi A, Shields JA. Conjunctival melanoma outcomes based on tumor origin in 382 consecutive cases. Ophthalmology. 2011;118(2):389-395.
- Spencer WH. Ophthalmic Pathology. An Atlas and Textbook (4th edition). Philadelphia: WB Saunders; 1996.
- Yanoff M, Sassani JW. Ocular Pathology (6th edition). Elsevier; 2009.
- Ocular Pathology Atlas. American Academy of Ophthalmology Web site. https://www.aao.org/resident-course/pathology-atlas. Published 2016. Accessed January 4, 2017.