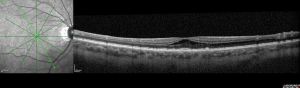
Stellate Nonhereditary Idiopathic Foveomacular Retinoschisis (SNIFR)
All content on Eyewiki is protected by copyright law and the Terms of Service. This content may not be reproduced, copied, or put into any artificial intelligence program, including large language and generative AI models, without permission from the Academy.
Disease Entity
Stellate nonhereditary idiopathic foveomacular retinoschisis (SNIFR) is a stellate foveal retinoschisis in patients without evidence of a hereditary or predisposing condition. The incidence of SNIFR in all pathologies causing foveomacular retinoschisis has been reported to be as high as 2%.[1] The condition is typically unilateral and has a female predominance, although bilateral and male cases have been documented. In a retrospective case series of 17 patients with SNIFR, 16 were female with an average age of 61.[2] In another study of 24 patients, 15 were female with an average age of 63.[1]
Pathophysiology
Although the mechanism remains unknown, authors have postulated an incomplete posterior vitreous detachment causing traction on Muller cells resulting in the schisis cavities.[1]
Diagnosis
History
Often patients are asymptomatic or have mild metamorphopsia and blurred vision.
Physical examination
Visual acuity (VA) typically ranges from 20/20 to 20/50, although few cases have been reported with poorer vision. Patients’ refractive error can range from hyperopia to myopia, but usually falls within the normal range. On fundoscopic examination, patients may have radial spoking around the fovea and schisis extending into the periphery. Most eyes with SNIFR may also have either an attached posterior hyaloid or an incomplete separation.[1][2]
Diagnostic procedures
Ocular coherence tomography (OCT): Cavities in the outer plexiform layer centrally in fovea and macula, and variable splitting of inner plexiform layer toward the periphery.[1][2]
Fluorescein angiography (FA): Typically shows no leakage and mild staining. [1][2][3]
Laboratory test
There are no laboratory tests to evaluate for SNIFR.
Differential diagnosis
- X-linked retinoschisis
- Niacin- and taxane-derived medication induced schisis
- Myopic degeneration
- Optic pit maculopathy
- Glaucoma
- Myotonic dystrophy
- Enhanced S-cone syndrome
- Autosomal dominant retinoschisis
Management
Most cases of SNIFR do not require any treatment as patients usually are asymptomatic or have minimal symptoms. One case reported performing pars plana vitrectomy, internal limiting membrane peeling, and C3F8 gas instillation for a 46-year-old female with a VA of 20/100 and foveal outer retinal defect with SNIFR. Final visual acuity was not reported, however, the schisis appeared resolved on OCT at post-operative month 12.[4] Topical dorzolamide drops have also been used, but further studies are needed to evaluate their effectiveness.[5]
References
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 Bloch E, Flores-Sánchez B, Georgiadis O, et al. AN ASSOCIATION BETWEEN STELLATE NONHEREDITARY IDIOPATHIC FOVEOMACULAR RETINOSCHISIS, PERIPHERAL RETINOSCHISIS, AND POSTERIOR HYALOID ATTACHMENT. Retina Phila Pa. 2021;41(11):2361-2369. doi:10.1097/IAE.0000000000003191
- ↑ 2.0 2.1 2.2 2.3 Ober MD, Freund KB, Shah M, et al. Stellate nonhereditary idiopathic foveomacular retinoschisis. Ophthalmology. 2014;121(7):1406-1413. doi:10.1016/j.ophtha.2014.02.002
- ↑ Montano M, Alfaro DV, Quiroz-Reyes MA, et al. STELLATE UNILATERAL NONHEREDITARY IDIOPATHIC FOVEOMACULAR RETINOSCHISIS: A MULTIMODAL IMAGING ANALYSIS AND CASE REPORT. Retin Cases Brief Rep. 2022;16(4):439-443. doi:10.1097/ICB.0000000000001001
- ↑ Moraes BRM, Ferreira BFA, Nogueira TM, Nakashima Y, Júnior HPP, Souza EC. VITRECTOMY FOR STELLATE NONHEREDITARY IDIOPATHIC FOVEOMACULAR RETINOSCHISIS ASSOCIATED WITH OUTER RETINAL LAYER DEFECT. Retin Cases Brief Rep. 2022;16(3):289-292. doi:10.1097/ICB.0000000000000966
- ↑ Ajlan RS, Hammamji KS. STELLATE NONHEREDITARY IDIOPATHIC FOVEOMACULAR RETINOSCHISIS: RESPONSE TO TOPICAL DORZOLAMIDE THERAPY. Retin Cases Brief Rep. 2019;13(4):364-366. doi:10.1097/ICB.0000000000000599