PresbyLASIK
All content on Eyewiki is protected by copyright law and the Terms of Service. This content may not be reproduced, copied, or put into any artificial intelligence program, including large language and generative AI models, without permission from the Academy.
Background
Presbyopia is an age-related loss of accommodation[1], whose physiopathology is not completely well understood. It’s the most frequent refractive error over 40’s[2] and is estimated that in 2050 there will be 1.782 billion people with presbyopia[3].
Classically corrected with reading glasses, the growing expectation of patients regarding spectacle independence led to the development of different surgical options.
These surgical correction techniques can be divided in two categories[1]:
Static Methods: increasing the depth of focus
- Monovision
- Corneal Inlays
- PresbyLASIK
- Conductive keratoplasty
- Multifocal intraocular lens (MFIOL)
- Extended Depth of Focus (EDOF) Lens
Dynamic Methods: restoring accommodation
- Scleral implants
- Accommodative IOL
Basic Concepts
Accommodation is an active process, dependent on the elastic properties of the lens. The cornea, in comparison, is a more static tissue with low depth of focus[4]. Enhancing corneal depth of focus through the creation of multifocal corneal surface is the basic mechanism of PresbyLASIK – a term introduced by Ruiz in 1996[5].
The technology of current excimer laser devices and femtosecond lasers enabled huge amount of flexibility in ablation patterns, including a range of multifocal corneal ones. As stated before, all of them based on modifying spherical aberration to increase focal amplitude.
The principles of each algorithm may be based on the dioptric power of refractive error and presbyopia correction calculation, corneal asphericity quotient (Q-value), and higher-order spherical aberrations changes or optical and transition zone manipulation[6].
Subtypes
Multifocal Transition Profile
Multifocal Transition Profile generates a transitional vertical multifocal ablation based on the creation of an intentional decentration of a hyperopic ablation profile[7]. It’s not currently being used, because it’s associated with significant vertical coma in corneal anterior surface[8].
Central PresbyLASIK
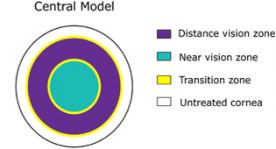
Central PresbyLASIK produces a small central optical area with higher curvature (hyperpositive area) for near vision, surrounded by a flatter area for far vision (Fig. 1)
It is pupil dependent and can be applied at the centre of the cornea in myopic and hyperopic profiles[1]. It’s also possible to use after initial myopic or hyperopic laser treatment for far vision[9][10].
The most important technical limitation is establishing the most adequate axis: the visual or optical axis, or the cornea vertex[1][2]. A lack of adequate alignment will induce coma aberrations.
It is the most commonly used PresbyLASIK technique[11]. There are mainly three different technologies available, all of them with published outcomes in hyperopic patients:
CustomVue™ VISX (AMO Development LLC, Milpitas, California, USA)
Combines the wavefront-guided hyperopic treatment with a presbyopic shape - steepens the central cornea for near vision while treating the periphery for distance[12].
Supracor™ (Technolas Perfect Vision GmbH, München, Germany)
Creates a hyperpositive area in the central 3.0mm zone, giving an addition of approximately 2 diopters[13] [14](Fig. 2).
It may be used symmetrically (for patients that demand good near vision) or asymmetrically (for patients that demand good near and distance vision)[5].
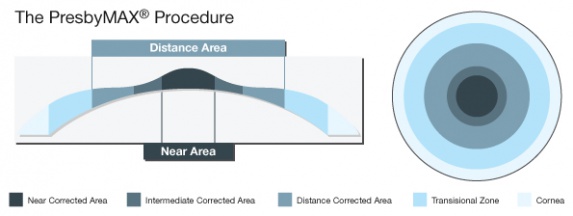
PresbyMAX™ (SCHWIND eye-tech-solutions GmbH, Kleinostheim, Germany)
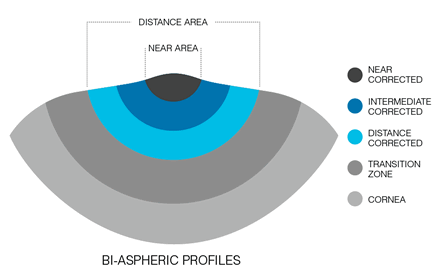
Creates a biaspheric multifocal corneal surface with a central hyperpositive area (to achieve +0,75 to +2,50D near correction) surrounded by an area in which the ablation is calculated to correct the distance refractive error. It’s the only technology of central PresbyLASIK with published results in myopic and emmetropic eyes[15][16] (Fig. 3).
Peripheral PresbyLASIK
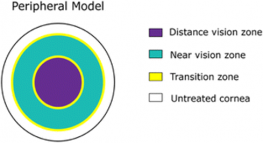
In Peripheral PresbyLASIK the peripheral cornea is ablated to create negative asphericity. The centre of the cornea is left for far vision and the middle periphery for near vision (for example, Nidek Advanced Vision, Nidek co. LTD, Gamagori, Japan) - fig. 4
The major limitation of this technique is in myopic correction, because it’s necessary to remove a significant amount of corneal tissue to create a hyperprolate shape[1][2]. For this reason, it’s more adequate for hyperopic eyes. Moreover, this method also requires an efficient excimer laser beam profile capable of compensating the loss of energy that happens while ablating the peripheral cornea.
As central PresbyLASIK, it’s pupil dependent too and has the same technical limitation related to establishment of the axis.
Laser Blended Vision® - Presbyond®
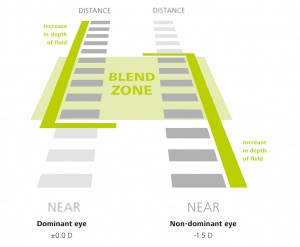
Laser Blended Vision® - Presbyond®(Carl Zeiss Meditec, Inc., Jena, Germany) approach induces a certain amount of spherical aberration to each eye, increasing the depth of focus[17] within a limited range to avoid visual quality degradation and makes the nondominant eye slightly myopic (-1,50D) - micro-monovision[18] (Fig. 5).
It can be performed on emmetropic, myopic and hyperopic presbyopes.
Patient Selection
Patient selection is crucial for having good results – patient expectations, job and hobbies must be considered[13][19].
Indications
Patients with early presbyopia (40-55 years of age) seems to be the ideal candidates for PresbyLASIK, whose lenses are still transparent and in whom intraocular surgery may be more risky than corneal refractive surgery. Other patients who could be good candidates for multifocal corneal ablations are pseudophakic with a previously implanted monofocal IOL.
Contraindications[20]
- Thin corneas or possible keratoconus precluding qualification for excimer laser surgery.
- Previous incisional corneal surgery, resulting in high levels of corneal aberrations due to irregular astigmatism.
- Ocular comorbidities (as glaucoma or maculopathy) potentially leading to contrast sensitivity or visual loss.
- Patients over 60 years old (better candidates for intraocular refractive surgery)
Outcomes
The majority of PresbyLASIK treatments have been performed in hyperopic patients – these patients[5][9][10][13][14][21], despite not having relevant different outcomes from myopic ones, are typically more satisfied[22].
Comparing central and peripheral PresbyLASIK, most papers report relatively good results for both uncorrected near and distance visual acuity (UNVA and UDVA) and a good degree of spectacle independence (from 72% to 93%)[9][10][14][15][16][21][22][23][24][25][26][27][28].
Central model is more advisable to achieve multifocality due to the physiologic pupil miosis during accommodation, and most papers corroborate that, revealing better UNVA in central models. On the other hand, peripheral presbyLASIK theoretically should provide better distance vision but that’s not corroborated by study results. However, both were associated with a relevant loss of at least two lines of distance visual acuity (2%-28%), a significant decrease in contrast sensivity and an important level of retreatment (6,75%-28,6%), which of course is undesirable[1].
It should still be noted that they may be supplemented with a relative degree of micro-monovision but a comparative study between this option and symmetrically presbyLASIK on both eyes[2].
Relatively to Laser Blended Vision® (combination of induced asphericity and micro-monovision), results reveal good near and distance vision and a superior safety profile is not currently available [11][17][29][30][31].
Limitations
We need to be aware that one of the most important limitation of PresbyLASIK is the lack of strong scientific evidence, namely the lack of reports with long follow-up and the absence of standardized outcome measures[1][32].
Another important issue is that even with good results in mild presbyopia, the truth is that the disease continues to evolve and efficacy diminishes over time. In addition, when these patients are undergo lens surgery, accurate IOL power calculation is more difficult and the possibility of multifocal IOL implantation are limited due to the multifocal corneal ablation.
Conclusions
Multifocal corneal ablation is one option for correction of presbyopia but application of this technique remains limited due to the temporary benefit of the procedure and the relatively high associated incidence of visual quality loss. Achieving a stable multifocal cornea with long term results remains a challenge.
References
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 1.6 Vargas-Fragoso, V, Alió JL. Corneal compensation of presbyopia: PresbyLASIK: an updated review. Eye Vis. 2017;4(1):11. doi:10.1186/s40662-017-0075-9.
- ↑ 2.0 2.1 2.2 2.3 Bilbao-Calabuig, R, Llovet-Osuna F. Non-lens-based surgical techniques for presbyopia correction. Arch la Soc Española Oftalmol (English Ed. 2017;92(9):426-435. doi:10.1016/j.oftale.2017.04.004.
- ↑ Frick KD, Joy SM, Wilson DA, Naidoo KS, Holden BA. The Global Burden of Potential Productivity Loss from Uncorrected Presbyopia. Ophthalmology. 2015;122(8):1706-1710. doi:10.1016/j.ophtha.2015.04.014.
- ↑ Moussa K, Jehangir N, Mannis T, Wong WL, Moshirfar M. Corneal Refractive Procedures for the Treatment of Presbyopia. Open Ophthalmol J. 2017;11(1):59-75. doi:10.2174/1874364101711010059.
- ↑ 5.0 5.1 5.2 Soler Tomás JR, Fuentes-Páez G, Burillo S. Symmetrical Versus Asymmetrical PresbyLASIK. Cornea. 2015;34(6):651-657. doi:10.1097/ICO.0000000000000339.
- ↑ Pinelli R, El-Shawaf H CD. P-Curve presbyopic LASIK. A new concept in refractive surgery. Cataract Refract Surg Today. 2010:54-56.
- ↑ Gobin L, Trau R, Tassignon MJ. Treatment for combined hypermetropia and presbyopia with a gaussian broad beam Excimer Laser]. Bull Soc Belge Ophtalmol. 2008;(307):27-36. http://www.ncbi.nlm.nih.gov/pubmed/18546924.
- ↑ Alió JL, Amparo F, Ortiz D, Moreno L. Corneal multifocality with excimer laser for presbyopia correction. Curr Opin Ophthalmol. 2009;20(4):264 271.doi:10.1097/ICU.0b013e32832a7ded.
- ↑ 9.0 9.1 9.2 Alió JL, Chaubard JJ, Caliz A, Sala E, Patel S. Correction of presbyopia by technovision central multifocal LASIK (presbyLASIK). J Refract Surg. 2006;22(5):453-460. doi:10.1016/S0084-392X(08)70034-0.
- ↑ 10.0 10.1 10.2 Saib N, Abrieu-Lacaille M, Berguiga M, Rambaud C, Froussart-Maille F, Rigal-Sastourne J-C. Central PresbyLASIK for Hyperopia and Presbyopia Using Micro-monovision With the Technolas 217P Platform and SUPRACOR Algorithm. J Refract Surg. 2015;31(8):540-546. doi:10.3928/1081597X-20150727-04.
- ↑ 11.0 11.1 Wang Yin GH, McAlinden C, Pieri E, Giulardi C, Holweck G, Hoffart L. Surgical treatment of presbyopia with central presbyopic keratomileusis: One-year results. J Cataract Refract Surg. 2016;42(10):1415-1423. doi:10.1016/j.jcrs.2016.07.031.
- ↑ Tamayo G. Surgical Techniques in Ophthalmology: Refractive Surgery.; 2008.
- ↑ 13.0 13.1 13.2 Ang RET, Cruz EM, Pisig AU, Solis MLPC, Reyes RMM, Youssefi G. Safety and effectiveness of the SUPRACOR presbyopic LASIK algorithm on hyperopic patients. Eye Vis. 2016;3(1):33. doi:10.1186/s40662-016-0062-6.
- ↑ 14.0 14.1 14.2 Ryan A, O’Keefe M. Corneal approach to hyperopic presbyopia treatment: Six-month outcomes of a new multifocal excimer laser in situ keratomileusis procedure. J Cataract Refract Surg. 2013;39(8):1226-1233. doi:10.1016/j.jcrs.2013.03.016.
- ↑ 15.0 15.1 Baudu P, Penin F, Arba Mosquera S. Uncorrected Binocular Performance After Biaspheric Ablation Profile for Presbyopic Corneal Treatment Using AMARIS with the PresbyMAX Module. Am J Ophthalmol. 2013;155(4):636-647.e1. doi:10.1016/j.ajo.2012.10.023.
- ↑ 16.0 16.1 Luger MHA, McAlinden C, Buckhurst PJ, Wolffsohn JS, Verma S, Arba Mosquera S. Presbyopic LASIK Using Hybrid Bi-Aspheric Micro-Monovision Ablation Profile for Presbyopic Corneal Treatments. Am J Ophthalmol. 2015;160(3):493-505. doi:10.1016/j.ajo.2015.05.021.
- ↑ 17.0 17.1 Reinstein DZ, Carp GI, Archer TJ, Gobbe M. LASIK for Presbyopia Correction in Emmetropic Patients Using Aspheric Ablation Profiles and a Micro-monovision Protocol With the Carl Zeiss Meditec MEL 80 and VisuMax. J Refract Surg. 2012;28(8):531-541. doi:10.3928/1081597X-20120723-01.
- ↑ Gifford P, Kang P, Swarbrick H, Versace P. Changes to Corneal Aberrations and Vision after PresbyLASIK Refractive Surgery Using the MEL 80 Platform. J Refract Surg. 2014;30(9):598-603. doi:10.3928/1081597X-20140709-01.
- ↑ Schlote T, Heuberger A. Multifocal Corneal Ablation (Supracor) in Hyperopic Presbyopia: 1-Year Results in a Cross-Sectional Study. Eur J Ophthalmol. 2017;27(4):438-442. doi:10.5301/ejo.5000871.
- ↑ Tamayo G. The dawn of presby-LASIK. Cataract Refract Surg Today. 2010;Jul/Aug:64-66.
- ↑ 21.0 21.1 Jackson WB, Tuan KA, Mintsioulis G. Aspheric Wavefront-guided LASIK to Treat Hyperopic Presbyopia: 12-Month Results With the VISX Platform. J Refract Surg. 2011;27(7):519-529. doi:10.3928/1081597X-20101110-02.
- ↑ 22.0 22.1 El Danasoury AM, Gamaly TO, Hantera M. Multizone LASIK with peripheral near zone for correction of presbyopia in myopic and hyperopic eyes: 1-year results. J Refract Surg. 2009;25(3):296-305.
- ↑ Uthoff D, Pölzl M, Hepper D, Holland D. A new method of cornea modulation with excimer laser for simultaneous correction of presbyopia and ametropia. Graefe’s Arch Clin Exp Ophthalmol. 2012;250(11):1649-1661. doi:10.1007/s00417-012-1948-1.
- ↑ Luger MHA, Ewering T, Arba-Mosquera S. One-Year Experience in Presbyopia Correction With Biaspheric Multifocal Central Presbyopia Laser In Situ Keratomileusis. Cornea. 2013;32(5):644-652. doi:10.1097/ICO.0b013e31825f02f5.
- ↑ Chan TCY, Kwok PSK, Jhanji V, Woo VCP, Ng ALK. Presbyopic Correction Using Monocular Bi-aspheric Ablation Profile (PresbyMAX) in Hyperopic Eyes: 1-Year Outcomes. J Refract Surg. 2017;33(1):37-43. doi:10.3928/1081597X-20161006-03.
- ↑ Pinelli R, Ortiz D, Simonetto A, Bacchi C, Sala E, Alió JL. Correction of presbyopia in hyperopia with a center-distance, paracentral-near technique using the Technolas 217z platform. J Refract Surg. 2008;24(5):494-500.
- ↑ Gordon M. Presbyopia Corrections with the WaveLight ALLEGRETTO: 3-Month Results. J Refract Surg. 2010;26(10):S824-S826. doi:10.3928/1081597X-20100921-10.
- ↑ Epstein RL, Gurgos MA. Presbyopia treatment by monocular peripheral presbyLASIK. J Refract Surg. 2009;25(6):516-523.
- ↑ Reinstein DZ, Archer TJ, Gobbe M. LASIK for Myopic Astigmatism and Presbyopia Using Non-Linear Aspheric Micro-Monovision with the Carl Zeiss Meditec MEL 80 Platform. J Refract Surg. 2011;27(1):23-37. doi:10.3928/1081597X-20100212-04.
- ↑ Reinstein DZ, Archer TJ GM. spheric ablation profile for presbyopic corneal treatment using the MEL80 and CRS Master Laser Blended Vision module. J Emmetropia. 2011;2(3):161-175.
- ↑ Courtin R, Saad A, Grise-Dulac A, Guilbert E, Gatinel D. Changes to Corneal Aberrations and Vision After Monovision in Patients With Hyperopia After Using a Customized Aspheric Ablation Profile to Increase Corneal Asphericity (Q-factor). J Refract Surg. 2016;32(11):734-741. doi:10.3928/1081597X-20160810-01.
- ↑ Pallikaris IG, Panagopoulou SI. PresbyLASIK approach for the correction of presbyopia. Curr Opin Ophthalmol. 2015;26(4):265-272. doi:10.1097/ICU.0000000000000162.