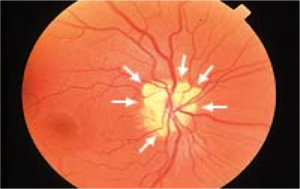
Optic Disc Drusen
All content on Eyewiki is protected by copyright law and the Terms of Service. This content may not be reproduced, copied, or put into any artificial intelligence program, including large language and generative AI models, without permission from the Academy.
Disease Entity
- Consist of refractive, hyaline-like calcified nodules made of mucoproteins and mucopolysaccharides that are located within the optic nerve head[1]
- Prevalence 3.4-24/1000[2]
- Males = Females
- Caucasians > Other races
- >70% bilateral, but asymmetric[3]
- Autosomal dominant inheritance with incomplete penetrance is suspected[4]
Etiology
Disc drusen are composed of small proteinaceous material that become calcified with advancing age. These deposits can be considered small tumors that develop within the optic nerve head, and may lead to an elevated disc (and therefore this condition is sometimes referred to as pseudopapilledema). They can be associated with retinitis pigmentosa, angioid streaks, Usher syndrome, Noonan syndrome and Alagille syndrome.[3] They also may lead to a loss of visual field or, in rare cases, central acuity or anterior ischemic optic neuropathy[5].
Pathophysiology
Pathogenesis is thought to be related to possibly inherited dysplasia of the optic disc with blood supply comprise, causing slowed axoplasmic flow and leading to the formation of calcific excrescences.
Diagnosis
Diagnosis is made by clinical examination of the optic nerve head in addition to ancillary imaging studies (see below). Pseudopapilledema vs. true papilledema must be distinguished.
History
Patients are usually asymptomatic. Rarely, they can have transient visual obscurations (approximately 9% of patients)[6]. Visual field loss may also be seen gradually, and it has been estimated that a quarter of patient of patients with optic disc drusen have a visual field defect other than an enlarged blind spot[7]
Physical Examination
If the optic disc drusen are superficial, this can aid in diagnosis during the dilated fundus exam. The optic nerve usually has a "lumpy-bumpy" appearance.
Signs
- Elevated, often small, optic disc with indistinct and irregular disc margins
- Drusen seen as round, white/yellow refractile bodies on the surface of the nerve or buried beneath it
- Anomalous vascular branching pattern (tortousity, optociliary shunt vessels)
- Nasal margin is most common site of drusen
- Spontaneous venous pulsations often seen
- Afferent pupillary defect if there is asymmetric nerve involvement
Symptoms
- Asymptomatic (most commonly)
- Transient visual obscurations
- Visual field defects
Clinical Diagnosis
- Fundus exam, with signs described above
- B-Scan (see below) and A-scan ultrasonography
- Fluorescein angiography (FA)
- Fundus autofluorescence (FAF)
- It is important to distinguish true papilledema from pseudopapilledema:
Assess the following:
- Is the optic disc hyperemic?
- In true disc edema, there is congestion of the disc microvasculature, with reddish hue of the disc.
- Are there microvascular abnormalities on the surface of the disc?
- True edema is associated with dilation and telangiectasias of the surface disc capillaries and may be demonstrate flame hemorrhages on or adjacent to the disc.
- At what depth in the retina does the blurring of the disc margin originate?
- In true disc edema, there is obscuration of both the retinal vessels and the disc margin, since the edema is at the level of the disc and peripapillary nerve fiber layer. In contrast, most cases of pseudopapilladema, the blurring usually results from abnormalities that are located deep to the retinal blood vessels; thus, the vessels are clearly visible as they cross the disc margin.
Diagnostic procedures
- B-/A-scan ultrasonography: optic nerve head with ODD is elevated and highly reflective. When decreasing the gain setting, calcified drusen maintain high signal intensity, whereas with papilladema, the signal intensity decreases.
- FAF/FAF: Superficial optic disc drusen will demonstrate autoflourescence. Early frames on the FA will demonstrate focal blockage of fluorescence. There may also be nodular late staining without leakage from disc surface capillaries. Papilledema in contrast shows early diffuse hyperfluorescence, with late leakage overlying and adjacent to the disc.
- CT scan: Superior to MRI for detection of drusen. Calcium produces bright signal at junction of the posterior globe and optic nerve on a CT scan.
- Optical coherence tomography (OCT): Although not necessary for diagnosis, OCT is helpful in detecting early nerve fiber layer thinning in cases of optic nerve head drusen, and can be predictive of visual field loss[7].
Differential diagnosis
- Papilledema
- Pseudopapilledema from another etiology
- Pseudotumor cerebri
- Tilted disc
- Myelinated NFL
- Crowded disc associated with hyperopia
Management
Optic disc drusen does not require treatment, and patients generally have good visual prognosis. There is currently no effective treatment for patients who have gradual loss of visual fields (some studies have suggested IOP lowering medications).
Surgery
There is currently no surgical treatment for optic disc drusen.
Complications
Rarely, the following vascular complications may occur:
- Flame disc hemorrhages
- Non-arteritic anterior ischemic optic neuropathy (NAION)
- Central retinal artery occlusion (CRAO)
- Peripapillary neovascular membranes[8]
Additional Resources
- Porter D, Vemulakonda GA. Drusen. American Academy of Ophthalmology. EyeSmart/Eye health. https://www.aao.org/eye-health/diseases/drusen-list. Accessed March 08, 2019.
- Patient Information Brochure. North American Neuro Ophthalmology Society (NANOS). https://www.nanosweb.org/drusen_information_brochure/ . Accessed March 3, 2025
References
- ↑ Friedman AH, Henkind P, Gartner S. Drusen of the optic discl. A histopathological study. Trans Ophthalmol Soc U K. 1975 Apr;95(1):4-9.
- ↑ Auw-Haedrich C1, Staubach F, Witschel H. Optic disk drusen. Surv Ophthalmol. 2002 Nov-Dec;47(6):515-32.
- ↑ 3.0 3.1 Golnik, K. Congenital anomalies and acquired abnormalities of the optic nerve, (Version 14.3). 2016. UptoDate (On-Line Serial).
- ↑ Antcliff RJ, Spalton DJ. Are optic disc drusen inherited?. Ophthalmology. 1999. 106 (7): 1278–81.
- ↑ Purvin V, King R, Kawasaki A, Yee. Anterior ischemic optic neuropathy in eyes with optic disc drusen". Arch. Ophthalmol. 2004. 122 (1): 48–53.
- ↑ American Academy of Ophthalmology. Basic and Clinical Science Course. Neuro- Ophthalmology. The Patient With Decreased Vision: Classification and Management. Optic Disc Drusen. 2007-2008;129.
- ↑ 7.0 7.1 Lee KM, Woo SJ, Hwang JM.PLoS One. Factors associated with visual field defects of optic disc drusen. 2018 Apr 30;13(4):e0196001.
- ↑ Delas B, Almudi L, Carreras A, Asaad M. Bilateral choroidal neovascularization associated with optic nerve head drusen treated by antivascular endothelial growth factor therapy. Clin Ophthalmol. 2012;6:225-30.