Intense Pulsed Light (IPL) Therapy
All content on Eyewiki is protected by copyright law and the Terms of Service. This content may not be reproduced, copied, or put into any artificial intelligence program, including large language and generative AI models, without permission from the Academy.
Intense pulsed light (IPL) therapy is a relatively new treatment for evaporative dry eye and rosacea.
Using filters in the IPL handpiece, the light spectrum emitted from the flash lamp can be absorbed by oxyhemoglobin. The light is converted to heat-inducing ablation of vascular structures. This process of photothermolysis is one of the proposed mechanisms of action of IPL for dry eye, where wavelengths selectively destroy blood vessels by targeting chromophores within the blood vessels. The destruction of telangiectasias along the eyelid inhibits access of inflammatory mediators to the meibomian glands. Other potential mechanisms include a mild local warming effect to allow better expression of meibum and destruction of bacteria that cause inflammation at the level of the meibomian glands.
IPL emits pulsed light at a wavelength in the range 500 – 1200 nm. Longer wavelengths (1000 nm) penetrate more deeply and can be used for telangiectasias situated deeper in the dermis and for large vessels. Lower wavelengths (500 to 600 nm) effectively treat smaller-caliber vessels but interact more readily with epidermal and dermal melanin. Therefore, shorter wavelength filters should be reserved for treating fair-skinned individuals (Fitzpatrick skin phototypes I – II). Energy density choice depends on the target type, requiring fluences ranging from 25 – 45 J/cm2. Larger vessels require more energy to heat up and smaller vessels heat more quickly. Pulses are delivered as single, double or triple pulses; each pulse lasting 2 – 25 ms for larger vessels and 2.5 – 5 ms for smaller vessels. Longer pulse widths are gentler, while shorter bursts of energy produce a stronger reaction. Using a pulse duration (generally between 0.5 – 88.5 ms) that is shorter than the thermal relaxation time of the target structures may spare surrounding tissue from excess heating. Different intervals between pulses range within 10 – 500 ms; the delay between pulses allows the non-target tissues to cool down while the heat is retained in the target of interest[1]. The micro pulses allow the epidermis cells and smaller vessels to cool down between pulses. At the same time, the heat is retained in the larger vessels, resulting in selective thermal damage[2].
IPL is used to treat facial skin damage, including wrinkles, coarseness, laxity, and dyspigmentation[3]. IPL increases the synthesis of collagen I and III, procollagen, collagenase, and elastin and increased hyaluronate receptor expression, thus supporting the role of IPL in dermal collagen remodeling and improving skin texture[4]. The reduction in the mechanical integrity of the upper dermal connective tissue is related to rosacea, allowing a passive dilation of the vasculature manifesting as erythema and telangiectasia, and extravascular leakage of inflammatory mediators causing inflammatory papules and pustules[5]. IPL improves rosacea by ablating these abnormal vessels and might also improve the dermal connective tissue disorganization and elastosis by the process of collagen remodeling. This would improve the vascular component of rosacea (erythema and telangiectasia), possibly followed by a reduction in the appearance of inflammatory lesions. It is also plausible that collagen remodeling is responsible for the longevity of the effects induced by IPL[5].
Treatment procedure
IPL treatment uses a wavelength band range from 550 to 1200 nm. The intensity of the treatment may be adjusted to 10 J/cm2, on a contact surface of cool Sapphire, 48 x13 mm (6.2 cm2), representing an energy density of 62 Joules in each flash. The parameters of the number of micropulses, size, and the time interval between them in each flash may be adjusted according to the degree of skin pigmentation.
The procedure begins protecting the eye with opaque goggles and applying ultrasound gel on the patient's periocular area, eyelids (canthal to canthal), and the facial cheek area to spread the energy conduct the light providing a high degree of protection and efficacy. The IPL treatment is carried out in two steps into the periocular area, and the cheek area:
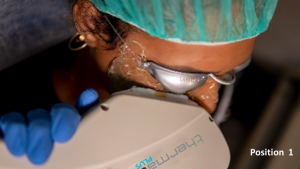
- For the periocular area, 6 flashes are applied in each eye as shown in the left image 3 flashes on the skin of the lower eyelid (position 1) and 3 flashes on the canthal area (position 2), taking care to avoid overlap the same area alternating each flash between positions 1 and 2.
- For the cheek area, 8 flashes on the skin of the four positions showed in the right image from position 1 to 4, also avoiding overlap the same area, and repeating once again from 1 to 4 position.
| IPL treatment zones, where the handpiece is applied on the skin | |||
|---|---|---|---|
 |
 |
 |

|
| Periocular area | Cheek area | ||
The same procedure is performed on the other side of the face. At the end of each session, the protective goggles and gel are removed.
The mechanical expression of the Meibomian glands may be performed. With the patient sitting on the slit lamp and using a cotton swab, the meibomian glands ofthe lower and upper eyelids weresqueezing toward the eyelid margin, until the mebium release was visualized.
Finally, sun protection cream is applied to avoid exposure to the sun for the first 48 hours. The subjects may receive four separate treatment sessions, the first day (D1), after 14 days (D14), after 28 days (D28), and after 49 days (D49). The room temperature and relative humidity may be stable during treatments 22± 0.5 ºC and of 60±3%, respectively.
Meibomian gland dysfunction
Introduction
Meibomian gland dysfunction (MGD) is a common condition associated with Dry eye disease (DED), representing the leading cause of the evaporative component. MGD increases the DED severity with a clinically adverse impact on patient's life quality[6]. The prevalence of MGD varies geographically and by age, with reports of 5%–20% in Western countries to 45%–70% in Asian ones [7].
The pathogenesis of MGD and DED has been described as a vicious cycle in which inflammation is the essential factor[7]. MGD is triggered by different factors (skin disorders, eyelid inflammation, and microbial infections), resulting in ductal epithelium hyperkeratinization and increased meibum viscosity. The glandular ductus is filled with viscous meibum, which contains keratinized cellular material, resulting in intraglandular cystic dilatation and atrophy[8]9. As a consequence, the lower outflow of the meibum induces the proliferation of commensal bacteria[9], releasing fatty acids and mono and diglycerides into the tear film, provoking more inflammation and irritation of the ocular surface[10]. The result is the instability of the tear film. This increases exposure of the corneal surface and its subepithelial nerve plexus, stimulating more inflammation [11]. This results in a vicious DED cycle that feeds back to the MGD cycle.
Different treatments have been proposed; the use of preservative-free artificial tears, anti-inflammatories, and cyclosporine; antibiotics to control the ocular surface microbiota or the presence of Demodex; dietary supplements with Omega-3 fatty acids to improve the lipid composition of the meibomian glands and tear film; warm compresses, and lid hygiene; radiofrequency to decrease the viscosity of the meibum, mechanical expression of the Meibomian glands, and intraductal probing[12]. The truth is that no one achieves a fully effective long-term improvement. Intense pulsed light (IPL) can successfully treat DED symptoms and signs by decreasing symptoms due to MGD, tear film abnormality, and tear inflammatory markers[13]. However, long term studies appear to show that the result is temporary with effects gone after nine months [14].
IPL mechanism of action
IPL can benefit dry eye by improving the dysfunction of the meibomian glands[15][16][17][18][19][20][13].
The exact IPL mechanism is unknown. At present, various effects have been proposed trying to explain this technology. The most important are:
- warming the meibomian glands to facilitate the expression and release of the meibum inside[21];
- improving the function of the Meibomian glands[22];
- inducing intravascular thrombosis of the small blood vessels surrounding the Meibomian glands and telangiectasia of the eyelid margin, reducing the levels of proinflammatory mediators that contribute to dry eye[13][15];
- reducing tear osmolarity, helping to control the inflammation of the ocular surface, which is one of the key factors in dry eye pathogenesis[15][23][18];
- reducing the load of Demodex mites that stimulate secondary inflammation[24];
- improving cellular functions such as collagen synthesis, fibroblasts regeneration, and motility in immunoregulatory cells[25][26];
- inducing a neurotrophic effect on the cornea and ocular surface and a neuroimmunomodulatory effect on the meibomian glands[27][28].
Evidence
The medical literature currently suggests improvements in the signs and symptoms of MGD after IPL therapy.[29] Toyos[15] treated with IPL showing improvement of DED symptomatology in 93% of cases and clinical signs in 87%. Vora and Gupta[30] reported improvement of lid margin edema, in the meibum quality score, and found a significant increase in the oil flow score and tear film break-up time, and a decrease in ocular surface disease index scoring. Craig et al[31] demonstrated that IPL alone was effective in improving the lipid layer and patient symptoms. Vegunta et al.[17] showed that the combination of IPL and MG expression improved dry eye symptoms in 89% of patients, and meibomian gland function in 77% of patients. Arita et al[32] showed the combination of IPL and Meibomian gland expression (MGX), improving homeostasis of the tear film and ameliorating ocular symptoms in patients with refractory MGD, compared with a control group with MGX alone. Karaca et al[33]referred amelioration of symptoms just 2 hours after the IPL and speculated with a neurological effect of the IPL. Cheng and Xue[34][23] referred good results after IPL treatment showing the improvement related to the microstructures of the meibomian glands with in vivo non-invasive confocal microscopy (INICM). Zhang-Nunes et al[35] showed efficacy using of augmented BroadBand Light (BBL) for MGD. However, the only prospective, randomized, and masked study available reports that results are temporary with effects gone after nine months [14]
Rosacea
Introduction
Rosacea is a common chronic skin disease on the central face, affecting cheeks, nose, chin, and forehead[36]. Manifestations include persistent facial erythema, papules, pustules, telangiectasia, and repetitive flushing. For the rosacea diagnosis, at least one of the primary features must be present on the face: flushing (transient erythema), nontransient erythema, papules and pustules, and telangiectasia. Secondary features may appear, including burning sensation, dry appearance of the skin, edema, ocular manifestations, phymatous changes, or different location other than the face[37]. It can present phymatous changes through hypertrophy of the sebaceous glands and fibrosis, the most common of which is rhinophyma[36]. The earliest clinical presentation of vascular rosacea is a recurring blush, followed by erythema, which becomes constant, and eventually telangiectasias[36].
Rosacea is classified into 4 subtypes: erythematotelangiectatic, papulopustular, phymatous, and ocular rosacea[37]: Ocular rosacea, affecting the eyes, is estimated to occur in up to three-quarters of patients with rosacea, and frequently produces a foreign-body sensation, dryness, burning, itching, redness, photophobia, tearing, and blurred vision[38]. Signs include blepharitis, meibomitis, keratitis, corneal neovascularization, and ulceration[38]. The spectrum of presentation varies from mild to severe, affecting any age group, typically most severe in the 30 to 50 years, being women more commonly affected than men[39]. It is characterized by episodes of exacerbation and remission. The prevalence ranges from 1% to 22% depending on the definition and population characteristics[39].
The pathophysiology of rosacea remains unclear, appearing involved in genetic factors, dysregulation of the immune system, vascular and neuronal dysfunction, and microorganisms, especially Demodex folliculorum. Triggers factors may exacerbate the symptomatology, such as heat, stress, ultraviolet light, wind, spicy food, hot beverages, smoking, alcohol, oral contraceptive pills or other hormonal influences, and corticosteroids[40]. The skin barrier is affected in rosacea, resulting in excessive transepidermal water loss, making the skin dry, inclined to scaling and peeling, and sensible to burning and stinging[41] Flushing and erythema are vascular elements representing an increased number of erythrocytes in inflamed vessels. Chronic extravascular fluid accumulation in the superficial dermis causes damage to the lymphatic vessels and subsequent edema. In addition, neutrophil elastase released at the site of inflammation degrades the extracellular matrix and Type IV collagen in the capillary walls, reducing the integrity of blood vessels[42]. Reduction in the integrity of the dermal connective tissue allows passive dilation of the vasculature, causing the telangiectatic component[43].
There are many treatment options for rosacea, such as topical metronidazole, azelaic acid cream, and non-irritating benzoyl peroxide; or systemic oral antibiotics, including tetracyclines, doxycycline, and minocycline. However, there are needs for other alternatives because of antibiotic resistance, irritation after the use of topic treatments[39], and the unlikely reduction of telangiectasia and centrofacial erythema[44][45]. Intense pulsed light (IPL) can successfully treat the clinical manifestations of rosacea that fail to respond to medical therapies, resolving telangiectasia and erythema, though longterm outcomes are less certain [46]. IPL is a relatively new technology that has been developed for treating vascular and pigmented lesions. It emits polychromatic light in millisecond pulse duration for delivering selective energy to target blood vessels[47], which is the target of rosacea treatment[48]. IPL has shown benefits treating facial rosacea, especially by improving the dysfunction of the meibomian glands and dry eye that these patients usually present[15][16][17][18][19][20][13]. The clinical improvement gets reflected by a decrease in symptoms due to MGD, tear film abnormality, and tear inflammatory markers[13].
Rosacea affects the physical aspect and can have critical psychosocial impacts, with a loss of self-confidence and distress in social or work circumstances. Patients with rosacea have higher rates of depression, anxiety, and decreased self-esteem[49][50][51][52][53].
IPL mechanism of action
IPL can benefit rosacea by improving the dysfunction of the meibomian glands and dry eye[15][16][17][18][19][20][13], and clearing telangiectasia, and reducing erythema[5][25][37][47][54][55].
The exact IPL mechanism is unknown. At present, various effects have been proposed trying to explain this technology. The mechanisms of action of the IPL is considered by a mixed effect on the inflammatory status, and in the microcirculation of the skin:
- Inflammatory status: patients with DED present high inflammatory molecules in tears and on the ocular surface[13][56]. IPL has the potential to interfere with this inflammatory cycle by upregulation of anti-inflammatory cytokines, downregulation of proinflammatory cytokines, or both[25]. IPL significantly reduces inflammatory lesions on the skin, presumably by downregulation of tumor necrosis factor-a (TNF-a), one of the cytokines responsible for the acute phase of inflammation[57]. TNF-a and IL-1 upregulate several types of MMPs[58], and since IPL downregulates TNF-a, it means that IPL, indirectly, diminishes the levels of these MMPs. In similar ways, corticosteroids may relieve dry eye symptoms[59] by lowering the cellular levels of cytokines, chemokines, and MMPs[60].
- Microcirculation of the skin: IPL affects the circulation of small blood vessels[16]. The light energy is absorbed for the haemoglobin, transforming into heat. It induces localized destruction by an internal micro-thrombosis[6][25] eliminating abnormal small blood vessels around the meibomian glands and telangectasic vessels in lids and eyelid margins. This represents a reduction in the reservoir of inflammatory mediators and, consequently, eliminates a major source of inflammation from the eyelids and meibomian glands[59].
Evidence
Seo et al[61] analyzed 17 patients suffering from MGD due to facial rosacea who were treated with IPL and meibomian gland expression with a followup of 12 months. Four sessions were carried out at intervals of 3 weeks each, showing a significant improvement in ocular symptoms. Symptom improvements were noted 3 weeks after the first IPL session and were maintained until the last visit, which was about 10 months after the last IPL session. In the study, improvements were noted in the lower lid margin vascularity, meibum expressibility and quality, and ocular symptoms persisted up to the final examination (Wilcoxon, P < 0.050 for all). However, the improvements of TBUT, staining score, and NIKBUT after IPL were not maintained at 6 and 12 months after baseline. Longterm effects beyond this time frame are not well established, so there may be a need to repeat IPL sessions frequently, which would be a major drawback, as has been pointed out by other authors’[16][17][30]. For example, the only prospective, randomized, and masked study on IPL in MGD by Rong et al reported that results were temporary with effects gone after nine months.[14].
Schroeter[62] reported 60 patients with a 75 – 87% clearance of facial telangiectases with an average of 4.1 treatments. Angermeier[63] described 153 patients with a 75 – 100% clearance 2 months after treatment with 1-4 sessions. Taub[58] reported 83% redness reduction, 75% flushing reduction, improvement of skin texture, and 64% acneiform breakouts reduction with an average of 3.6 treatments IPL sessions at 3-week intervals. Mark[15] presented a reduction of blood flow by 30%, the intensity of erythema by 21%, and telangiectasia by 29% after five IPL sessions.
References
- ↑ Kassir R, Kolluru A, Kassir M. Intense Pulsed Light for the Treatment of Rosacea and Telangiectasias. J Cosmet Laser Ther. 2011;13(5):216-222.
- ↑ Dierickx CC, Casparian JK, Venugopalan V, Farinelli WA, Anderson RR. Thermal Relaxation of Port-Wine Stain Vessels Probe in Vivo: The Need for 1–10 Millisecond Laser Pulse Treatment. J Invest Dermatol. 1995;105:709 – 714.
- ↑ Bitter P. Non-Invasive Photorejuvenation of Photodamaged Skin Using Serial, Full Face Intense Pulsed Light Treatments. Dermatol Surg 2000; 26:835–43.
- ↑ Zelickson B, Kist D. Effect of Pulsed Dye Laser and Intense Pulsed Light Source on the Dermal Extracellular Matrix Remodelling. Lasers Surg Med 2000; 12 (Suppl.):17.
- ↑ Jump up to: 5.0 5.1 5.2 Papageorgiou P, Clayton W, Norwood S, Chopra S, Rustin M. Treatment of Rosacea with Intense Pulsed Light: Significant Improvement and Long-lasting Results. Br J Dermatol. 2008;159:628-632.
- ↑ Jump up to: 6.0 6.1 Ding J, Sullivan DA. Aging and Dry Eye Disease. Exp Gerontol. 2012;47(7):483–490.
- ↑ Jump up to: 7.0 7.1 Baudouin C, Messmer EM, Aragona P, et al. Revisiting the Vicious Circle of Dry Eye Disease: A Focus on the Pathophysiology of Meibomian Gland Dysfunction. Br J Ophthalmol. 2016;100(3):300–306.
- ↑ Nichols KK, Foulks GN, Bron AJ et al. The International Workshop on Meibomian Gland Dysfunction: Executive Summary. Investigative Ophthalmology and Visual Science, 2011;52(4):, 1922–1929.
- ↑ Borchman D, Foulks GN,Yappert MC,Milliner SE. Differences in Human Meibum Lipid Composition with Meibomian Gland Dysfunction Using NMR and Principal Component Analysis. Investigative Ophthalmology & Visual Science, 2012; 53 (1): 337–347.
- ↑ Graham JE, Moore JE, Jiru X, et al. Ocular Pathogen or Commensal: A PCR-Based Study of Surface Bacterial Flora in Normal and Dry Eyes. Investigative Ophthalmology and Visual Science, 2007; 48(12):5616–5623.
- ↑ Benítez Del Castillo JM, Wasfy MA, Fernandez C, Garcia-Sanchez J. An in Vivo Confocal Masked Study on Corneal Epithelium and Subbasal Nerves in Patients with Dry Eye. Invest Ophthalmol Vis Sci. 2004;45(9):3030-3035.
- ↑ Geerling G, Tauber J, Baudouin C, et al. The International Workshop on Meibomian Gland Dysfunction: Report of the Subcommittee on Management and Treatment of Meibomian Gland Dysfunction. Invest Ophthalmol Vis Sci. 2011;52(4):2050–2064.
- ↑ Jump up to: 13.0 13.1 13.2 13.3 13.4 13.5 13.6 Liu R, Rong B, Tu P, et al. Analysis of Cytokine Levels in Tears and Clinical Correlations After Intense Pulsed Light Treating Meibomian Gland Dysfunction. Am J Ophthalmol. 2017;183:81-90.
- ↑ Jump up to: 14.0 14.1 14.2 Rong, Y. Tang, P. Tu, R. Liu, J. Qiao, W. Song, et al. Intense pulsed light applied directly on eyelids combined with meibomian gland expression to treat meibomian gland dysfunction. Photomed Laser Surg, 36 (2018), pp. 326-332.
- ↑ Jump up to: 15.0 15.1 15.2 15.3 15.4 15.5 15.6 Toyos R, McGill W, Briscoe D. Intense Pulsed Light Treatment for Dry Eye Disease Due to Meibomian Gland Dysfunction; a 3-Year Retrospective Study. Photomed Laser Surg. 2015;33(1):41-46.
- ↑ Jump up to: 16.0 16.1 16.2 16.3 16.4 Craig JP, Chen YH, Turnbull PR. Prospective Trial of Intense Pulsed Light for the Treatment of Meibomian Gland Dysfunction. Invest Ophthalmol Vis Sci. 2015;56(3):1965-1970. Published 2015 Feb 12.
- ↑ Jump up to: 17.0 17.1 17.2 17.3 17.4 Vegunta S, Patel D, Shen JF. Combination Therapy of Intense Pulsed Light Therapy and Meibomian Gland Expression (IPL/MGX) Can Improve Dry Eye Symptoms and Meibomian Gland Function in Patients With Refractory Dry Eye: A Retrospective Analysis. Cornea. 2016;35(3):318-322.
- ↑ Jump up to: 18.0 18.1 18.2 18.3 Dell SJ, Gaster RN, Barbarino SC, Cunningham DN. Prospective Evaluation of Intense Pulsed Light and Meibomian Gland Expression Efficacy on Relieving Signs and Symptoms of Dry Eye Disease Due to Meibomian Gland Dysfunction. Clin Ophthalmol. 2017;11:817-827.
- ↑ Jump up to: 19.0 19.1 19.2 Jiang X, Lv H, Song H, et al. Evaluation of the Safety and Effectiveness of Intense Pulsed Light in the Treatment of Meibomian Gland Dysfunction. J Ophthalmol. 2016;2016:1910694.
- ↑ Jump up to: 20.0 20.1 20.2 Gupta PK, Vora GK, Matossian C, Kim M, Stinnett S. Outcomes of Intense Pulsed Light Therapy for Treatment of Evaporative Dry Eye Disease. Can J Ophthalmol. 2016;51(4):249-253.
- ↑ Wei Y, Asbell PA. The Core Mechanism of Dry Eye Disease Is Inflammation. Eye Contact Lens. 2014;40:248-256.
- ↑ Yin Y, Liu N, Gong L, Song N. Changes in the Meibomian Gland after Exposure to Intense Pulsed Light in Meibomian Gland Dysfunction (MGD) Patients. Curr Eye Res. 2018;43:308-313.
- ↑ Jump up to: 23.0 23.1 Xue AL, Wang MTM, Ormonde SE, Craig JP. Randomised Double-Masked Placebo-Controlled Trial of the Cumulative Treatment Efficacy Profile of Intense Pulsed Light Therapy for Meibomian Gland Dysfunction. Ocul Surf. 2020;18(2):286-297.
- ↑ Prieto VG, Sadick NS, Lloreta J, Nicholson J, Shea CR. Effects of Intense Pulsed Light on Sun-Damaged Human Skin, Routine, and Ultrastructural Analysis. Lasers Surg Med. 2002;30:82-85.
- ↑ Jump up to: 25.0 25.1 25.2 25.3 Byun JY, Choi HY, Myung KB, Choi YW. Expression of IL-10, TGF-B1 and TNF-α in Cultured Keratinocytes (HaCaT Cells) after IPL Treatment or ALA-IPL Photodynamic Treatment. Ann Dermatol. 2009;21(1): 12–17.
- ↑ Cuerda-Galindo E, Díaz-Gil G, Palomar-Gallego MA, Linares-GarcíaValdecasas R. Increased Fibroblast Proliferation and Activity after Applying Intense Pulsed Light 800-1200 Nm. Ann Anat. 2015;198:66-72.
- ↑ Choi EY, Kang HG, Lee CH, et al. Langerhans Cells Prevent Subbasal Nerve Damage and Upregulate Neurotrophic Factors in Dry Eye Disease. PLoS One. 2017;12(4):E0176153.
- ↑ Awad SS, El-Din WH, Low Energy IPL Therapy for the Management of Recalcitrant Postherpetic Neuralgia. Laser Therapy. 2008;17(1):23-28.
- ↑ Wladis EJ, Aakalu VK, Foster JA, Freitag SK, Sobel RK, Tao JP, Yen MT. Intense Pulsed Light for Meibomian Gland Disease: A Report by the American Academy of Ophthalmology. Ophthalmology. 2020 Sep;127(9):1227-1233. doi: 10.1016/j.ophtha.2020.03.009. Epub 2020 Apr 21. PMID: 32327256.
- ↑ Jump up to: 30.0 30.1 Vora G, Gupta P. Intense Pulsed Light Therapy for the Treatment of Evaporative Dry Eye Disease. Curr Opin Ophthalmol. 2015;26:314–318.
- ↑ Craig J, Chen Y, Turnbull P. Prospective Trial of Intense Pulsed Light for the Treatment of Meibomian Gland Dysfunction. Invest Ophthalmol Vis Sci. 2015;56(3):1965–1970.
- ↑ Arita R, Fukuokab S, Morishigec N. Therapeutic Efficacy of Intense Pulsed Light in Patients with Refractory Meibomian Gland Dysfunction. The Ocular Surface 2019;17 (1):104-110.
- ↑ Karaca EE, Evren Kemer Ö, Özek D. Intense Regulated Pulse Light for the Meibomian Gland Dysfunction. Eur J Ophthalmol. 2020;30(2):289-292.
- ↑ Cheng S, Jiang F, Chen H, Gao H, Huang Y. Intense Pulsed Light Therapy for Patients with Meibomian Gland Dysfunction and Ocular Demodex Infestation. Current Medical Science, 2019;39(5):800-809.
- ↑ Zhang-Nunes S, Guo S, Lee D, Chang J, Nguyen A. Safety and Efficacy of an Augmented Intense Pulse Light Protocol for Dry Eye Syndrome and Blepharitis. Photobiomodul Photomed Laser Surg. 2021 Mar;39(3):178-184. doi: 10.1089/photob.2020.4913. Epub 2020 Dec 24. PMID: 33370543.
- ↑ Jump up to: 36.0 36.1 36.2 Van Zuuren EJ, Fedorowicz Z, Carter B, van Der Linden MM, Charland L. Interventions for Rosacea. Cochrane Database Syst Rev. 2015;2015(4):CD003262.
- ↑ Jump up to: 37.0 37.1 37.2 Wilkin J, Dahl M, Detmar M, Drake L, Liang MH, Odom R, Powell F. National Rosacea Society Expert Committee. Standard Grading System for Rosacea: Report of the National Rosacea Society Expert Committee on the Classification and Staging of Rosacea. J Am Acad Dermatol. 2004;50:907–12.
- ↑ Jump up to: 38.0 38.1 Vieira AC, Mannis MJ. Ocular Rosacea: Common and Commonly Missed. J Am Acad Dermatol 2013;69:Suppl 1:S36-S41.
- ↑ Jump up to: 39.0 39.1 39.2 Tan J, Berg M. Rosacea: Current State of Epidemiology. J Am Acad Dermatol. 2013;69:S27–35.
- ↑ Two AM, Wu W, Gallo RL, Hata TR. Rosacea: Part I. Introduction, Categorization, Histology, Pathogenesis, and Risk Factors. J Am Acad Dermatol 2015;72:749-758.
- ↑ Two AM, Wu W, Gallo RL, Hata TR. Rosacea: Part II. Topical and Systemic Therapies in the Treatment of Rosacea. J Am Acad Dermatol 2015;72:761-770.
- ↑ Rice WG, Weiss SJ. Regulation of Proteolysis at the Neutrophilsubstrate Interface by Secretory Leukoprotease Inhibitor. Science. 1990;249:178 – 181.
- ↑ Motley RJ, Barton S, Marks R. The Signifi Cance of Telangiectasia in Rosacea. In: Acne and Related Disorders: An International Symposium. Wales: Martin Dunitz: Cardiff; 1989:339 – 344.
- ↑ Tanghetti E, Del Rosso JQ, Thiboutot D, et al. Consensus Recommendations from the American Acne & Rosacea Society on the Management of Rosacea, Part 4: A Status Report on Physical Modalities and Devices. Cutis. 2014;93(2):71-76.
- ↑ Wat H, Wu DC, Rao J, Goldman MP. Application of Intense Pulsed Light in the Treatment of Dermatologic Disease: A Systematic Review. Dermatol Surg. 2014;40:359-377.
- ↑ Mark KA, Sparacio RM, Voigt A, Marenus K, Sarnoff DS. Objective and Quantitative Improvement of Rosacea-Associated Erythema after Intense Pulsed Light Treatment. Dermatol Surg. 2003;29:600–04.
- ↑ Jump up to: 47.0 47.1 Babilas P, Schreml S, Eames T, Hohenleutner U, Szeimies RM, Landthaler M. Split-Face Comparison of Intense Pulsed Light with Short- and Long-Pulsed Dye Lasers for the Treatment of Port-Wine Stains. Lasers Surg Med. 2010;42:720–27.
- ↑ Sa J, Dj S. Overview of Lasers and Their Properties. Dermatologic Therapy. 2000;13:2–16.
- ↑ Levy LL, Emer JJ. Emotional Benefit of Cosmetic Camouflage in the Treatment of Facial Skin Conditions: Personal Experience and Review. Clin Cosmet Investig Dermatol. 2012;5:173-182.
- ↑ Wilkin JK. Rosacea: Pathophysiology and Treatment. Arch Dermatol 1994; 130:359–62.
- ↑ Gupta A, Chaudhry M. Rosacea and Its Management: An Overview. J Eur Acad Dermatol Venereol 2005; 19:273–85.
- ↑ Halioua B, Cribier B, Frey M, Tan J. Feelings of Stigmatization in Patients with Rosacea. J Eur Acad Dermatol Venereol 2017;31:163-168.
- ↑ Bewley A, Fowler J, Schöfer H, Kerrouche N, Rives V. Erythema of Rosacea Impairs Quality of Life: Results of a Meta-Analysis. Dermatol Ther (Heidelb) 2016;6:237-247.
- ↑ Liu J, Liu J, Ren Y, Li B, Lu S. Comparative Efficacy of Intense Pulsed Light for Different Erythema Associated with Rosacea. J Cosmet Laser Ther. 2014;16:324-327.
- ↑ Deaver Peterson J, Katz TM. Open-Label Study Assessing the Efficacy and Tolerability of Topical Skin Care and Sun Protection Alone and in Combination with Intense Pulsed Light Therapy. J Cosmet Dermatol. 2019;18(6):1758-1764.
- ↑ Stevenson W, Chauhan S, Dana R. Dry Eye Disease: An Immune-Mediated Ocular Surface Disorder. Arch Ophthalmol. 2012;130(1):90–100.
- ↑ Taylor M, Porter R, Gonzalez M. Intense Pulsed Light May Improve Inflammatory Acne through TNF-a down-Regulation. J Cosmet Laser Ther. 2014;16(2):96–103.
- ↑ Jump up to: 58.0 58.1 Li D, Shang T, Kim H, Solomon A, Lokeshwar B, Pflugfelder S. Regulated Expression of Collagenases MMP-1, -8, and -13 and Stromelysins MMP-3, -10, and -11 by Human Corneal Epithelial Cells. Invest Ophthalmol Vis Sci. 2003;44:2928–2935.
- ↑ Jump up to: 59.0 59.1 Dell SJ. Intense Pulsed Light for Evaporative Dry Eye Disease. Clin Ophthalmol. 2017;11:1167-1173.
- ↑ Byun Y, Kim T, Kwon S, et al. Efficacy of Combined 0.05% Cyclosporine and 1% Methylprednisolone Treatment for Chronic Dry Eye. Cornea. 2012;31(5):509–513.
- ↑ Seo KY, Kang SM, Ha DY, Chin HS, Jung JW. Long-Term Effects of Intense Pulsed Light Treatment on the Ocular Surface in Patients with Rosacea-Associated Meibomian Gland Dysfunction. Cont Lens Anterior Eye. 2018;41(5):430-435.
- ↑ Schroeter CA, Haaf-von Below S, Neuman HA. Effective Treatment of Rosacea Using Intense Pulsed Light Systems. Dermatol Surg 2005; 31:1285–9.
- ↑ Angermeier MC. Treatment of Facial Vascular Lesions with Intense Pulsed Light. J Cutan Laser Ther. 1999;1(2):95 – 100.

