Fetal Alcohol
All content on Eyewiki is protected by copyright law and the Terms of Service. This content may not be reproduced, copied, or put into any artificial intelligence program, including large language and generative AI models, without permission from the Academy.
Fetal Alcohol Syndrome: An Ophthalmologic Perspective
Disease Entity
Fetal Alcohol Syndrome (FAS) is an irreversible congenital condition that is a result of maternal alcohol use during pregnancy[1]. Classic signs include: abnormal facial features (short horizontal palpebral fissure/blepharophimosis, thin vermillion border, and smooth philtrum), growth retardation, and neurobehavioral impairment[2]. These signs range greatly in severity, and can include any combination of the classic signs.
FAS is a syndrome that falls under a larger group of conditions known as Fetal Alcohol Spectrum Disorder (FASD). FASD includes:
- Alcohol-Related Neurodevelopmental Disorder (ARND): may have intellectual disabilities and problems with behavior and learning.
- Alcohol-Related Birth Defects (ARBD): may have problems with the heart, kidney, bones, or hearing.
- Neurobehavioral Disorder Associated with Prenatal Alcohol Exposure (ND-PAE)[3]: mother must have consumed more than minimal levels of alcohol before the child’s birth AND the child will have problems in 3 areas: 1) thinking and memory, 2) behavior, mood, and shifting attention between tasks, and 3) trouble with day-to-day living and playing with others.
- FAS: the most severe end of the spectrum involving central nervous system (CNS) problems, facial features, and growth problems.
Etiology
Alcohol is a known CNS teratogen that causes reduced brain volume and irregular brain and facial structure[4]. Alcohol crosses the placenta and, although there are many hypotheses, the exact mechanism by which alcohol induces CNS and structural changes is still unclear[4]. Some proposed mechanisms include: direct cytotoxic effect to embryonic cells (specifically the anterior neural ridge which organizes the prosencephalon), epigenetic changes leading to disrupted neural plasticity, and disruption of retinoic acid-based cell signaling[4][5][6][7].
Epidemiology
The estimated prevalence of FASD is 7.7 per 1,000 individuals worldwide, with ARND being more common than FAS[8]. The Centers for Disease Control and Prevention (CDC) studies show up to 1 in 20 U.S. school-aged children may have fetal alcohol spectrum disorders (FASDs)[9] . Estimates of the prevalence of FASD in the US and Western Europe range from 0.6 to 5.0% among school-aged children[10]. The estimated lifetime cost on average for an individual with FAS in 2002 was 2 million US dollars[11]. It is estimated that the cost to the United States for FAS alone is over $4 billion annually.
Ocular Specific Pathology
Up to 90% of newborns with maternal alcohol misuse during pregnancy have ocular damage or abnormalities[12] [13]. Both periocular and intraocular structures can be affected[14].
Periocular[14][15][16][17]
- Blepharophimosis (short horizontal palpebral fissures, i.e. decreased distance between the medial and lateral canthi) is commonly found and easy to measure[16].
- Blepharoptosis (drooping of upper eyelid) is non-specific, but can be seen in some FAS patients[13].
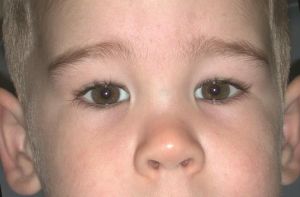
- Epicanthus or epicanthal folds (vertical fold of skin on the lateral nose, figure 1), a finding reported in up to 80% of infants exposed to alcohol having epicanthus[16][18].
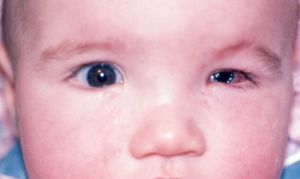
- Microphthalmia (abnormal and small eyes, figure 2) is commonly found in FAS and can aid in diagnosis of FAS[13][16][19].
- Telecanthus (increased distance between the medial eye canthi) is commonly found in FAS[16][20].
Intraocular
- Cornea and anterior chamber: findings resembling Axenfeld-Rieger syndrome and Peter's anomaly, glaucoma, uveal coloboma.
- Lens: cataract has been seen with FAS.
- Optic nerve: hypoplasia (in experimental models, this is due to reduced densities of ganglion cells and their axons along with damage to glial cells and myelin sheaths) or optic atrophy has been found in up to 48% of Swedish children with FAS[12][16][21][22].
- Retina: persistent fetal vasculature and dysmorphogenesis of the retina have been reported, increased tortuosity of the retinal vessels, found in up to 49% of Swedish children with FAS[13][16][21].
Eye Movement and Eye Function (motor control and executive function)[23]
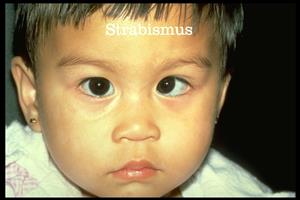
- Strabismus (abnormal alignment of eyes, figure 3) is non-specific, but commonly found in FAS[13].
- Prolonged reaction times, excessive direction errors, and no expression of saccades[23].
- Nystagmus[24].
- Amblyopia[24].
- Decreased vision in up to 65% of Swedish children with FAS with acuity < 0.2 (20/32 Snellen equivalent)[12].
- Possible dysfunction of frontal lobes[23]
Diagnosis
Clinical
Early detection and diagnosis leads to significantly less comorbidities and symptoms in later life of FAS patients[25]. FAS is diagnosed clinically and requires at least 2 of the following findings[26]:
- characteristic facial features (short horizontal palpebral fissure
- thin vermillion border, smooth philtrum)
- signs of growth retardation (height and/or weight <10th percentile)
- clear evidence of brain involvement
- neurobehavioral involvement
Documented maternal alcohol use is not necessary but can help support a diagnosis FAS if present[26]. FAS is often missed in newborns and can have a diagnostic delay as late as early adulthood. Facial features characteristic of FAS typically diminish with age, which reduces the chance of detecting classic dysmorphology in adult evaluations.[27] While there are ongoing efforts in search of more sensitive biomarkers to aide in the diagnosis of FAS, diagnosis remains clinical and relies on a multidisciplinary approach[28].
Ocular Signs and Symptoms
The only ophthalmologic diagnostic criteria for FAS is short palpebral fissures, but there are many periocular and intraocular signs that can point to a diagnosis of FAS. See above: Ocular Specific Pathology.
Ocular signs present earlier than signs of growth retardation and brain and neurobehavioral involvement and thus can be useful in aiding the early diagnosis of FAS. Ophthalmologic abnormalities such as refractive errors, strabismus, and fundus abnormalities seem to remain unchanged and persistent throughout childhood and adolescence[27][29].
Detection through ophthalmologic exam
With the rising prevalence of FAS, there is an opportunity for the field of ophthalmology to drastically reduce the morbidity of FAS patients through potentially earlier diagnosis and management with a thorough eye exams. Some studies suggest a full ophthalmic exam in all children who are suspected of having FAS[16]. This exam includes: inspection of periocular features (supplemented with morphometric analysis if needed), visual acuity (with visual evoked potentials if needed), slit lamp exam, and ophthalmoscopic exam with particular attention to the optic disc for signs of hypoplasia and the retina vasculature for signs of tortuosity[16][30]. Visual acuity can also be used to aid in diagnosis as children with FAS tend to have reduced best-corrected visual acuity[12]. Eye movement tasks and eye tracking measures are other potential tools for assessing FAS in children as well as measuring executive function in FAS patients[23][31]. Providing an FAS diagnosis earlier in life through an eye exam could help provide earlier management of this disease overall and reduce both ocular comorbidities (vision loss) and cognitive/neurobehavioral comorbidities.
Comorbidities
A 2016 meta-analysis showed that the five most prevalent comorbidities of FAS were: expressive language disorder, chronic otitis media, conduct disorder, receptive language disorder, and abnormal function of peripheral nervous system and special senses[32]. There also tend to be higher rates of mental disorders in people with FAS[33] and those with FAS are at higher risk of violent behavior, criminality, and criminalization than the average population[34].
Differential Diagnosis[35]
Syndromes that may appear similar to FAS include: Williams Syndrome, DiGeorge Syndrome, Velocardiofacial Syndrome, Noonan Syndrome, Fetal Hydantoin Syndrome, Fetal Valproate, Dubowitz syndrome, fetal toluene embryopathy and Maternal Phenylketonuria (PKU)[35][36].
Management
Primary Prevention
FAS is an irreversible congenital disorder that can only be prevented by decreasing alcohol intake during the whole pregnancy. Though research exploring ways to mitigate the effects of alcohol on a developing fetus suggests that antioxidants present in cruciferous vegetables like broccoli may help reduce the stress of alcohol on neural crest cells[37]. Ongoing research suggests there may be a role for supplements including choline, natural antioxidants and other nutritional agents during embryogenesis to prevent the development of FASD.[38] There is no known safe limit of alcohol consumption during pregnancy. Both quantity and pattern (binge) of drinking are more likely important factors in the teratogenic effects. Pregnant women and reproductive-aged women without reliable contraception should be advised to abstain from alcohol. Interventions from a primary care physician that include alcohol use screening in women of child-bearing age is thought to be influential in prevention of FASD.[39]
General Treatment
Early detection along with appropriate behavioral and special education are the most important factors for improved outcomes in children with FAS[25]. These specialized therapies improve social and cognitive abilities and have an inverse relationship with time of diagnosis. Treatment is highly individualized and can include occupational therapy, speech therapy, and cognitive behavioral therapy for patients who suffer from anxiety and/or depression.
Medical Therapy
There are no specific medications approved to treat FAS, but appropriate medication can be used for related disease manifestations (e.g. stimulants for hyperactivity).
Complications
FAS is a lifelong disorder, and most treatment is addressed at the level that the syndrome is expressed. Patients generally tend to have lower academic performance, difficulty reading social cues, and higher rates of incarceration[40]. These manifestations of FAS can lead to downstream effects on health through socioeconomic factors.
Prognosis
Long-term prognosis for FAS patients is generally poor with higher rates of alcohol/drug abuse, psychiatric disorders, unemployment, sexual misconduct, and disability[41][42]. Studies suggest there may be an association between FAS and Autism Spectrum Disorder.[43] One study also reported much lower average life expectancy for FAS patients at 34 years old with deaths reported due to suicide (15%), accidents (14%), poisoning by illegal drugs or alcohol (7%), diseases of the nervous and respiratory systems (8% each), and diseases of the digestive system (7%)[44].
Additional Resources
- Centers for Disease Control and Prevention (CDC: https://www.cdc.gov/ncbddd/fasd/index.html
- National Organization on Fetal Alcohol Syndrome: https://nofas.org/
- Families Affected by Fetal Alcohol Spectrum Disorder (FAFASD): https://fafasd.net/
References
- ↑ Chudley AE, Conry J, Cook JL, Loock C, Rosales T, LeBlanc N. Fetal alcohol spectrum disorder: Canadian guidelines for diagnosis. Cmaj 2005;172:S1-S21.
- ↑ Astley SJ. Comparison of the 4-digit diagnostic code and the Hoyme diagnostic guidelines for fetal alcohol spectrum disorders. Pediatrics 2006;118:1532-45.
- ↑ CDC. Key Findings: Neurobehavioral Disorder Associated with Prenatal Alcohol Exposure. Centers for Disease Control and Prevention https://www.cdc.gov/ncbddd/fasd/features/neurobehavioral-disorder-alcohol.html (2018).
- ↑ Jump up to: 4.0 4.1 4.2 Goodlett CR, Horn KH, Zhou FC. Alcohol teratogenesis: mechanisms of damage and strategies for intervention. Experimental Biology and Medicine 2005;230:394-406.
- ↑ Sulik KK. Genesis of Alcohol-Induced Craniofacial Dysmorphism. Experimental Biology and Medicine 2005;230:366-75.
- ↑ Varadinova M, Boyadjieva N. Epigenetic mechanisms: A possible link between autism spectrum disorders and fetal alcohol spectrum disorders. Pharmacological research 2015;102:71-80.
- ↑ Deltour L, Ang HL, Duester G. Ethanol inhibition of retinoic acid synthesis as a potential mechanism for fetal alcohol syndrome. The FASEB journal 1996;10:1050-7.
- ↑ Popova S, Charness ME, Burd L, Crawford A, Hoyme HE, Mukherjee RAS, Riley EP, Elliott EJ. Fetal alcohol spectrum disorders. Nat Rev Dis Primers. 2023;9(1):11.
- ↑ https://www.cdc.gov/fasd/data/index.html
- ↑ May PA, Chambers CD, Kalberg WO, Zellner J, Feldman H, Buckley D, Kopald D, Hasken JM, Xu R, Honerkamp-Smith G, Taras H, Manning MA, Robinson LK, Adam MP, Abdul-Rahman O, Vaux K, Jewett T, Elliott AJ, Kable JA, Akshoomoff N, Falk D, Arroyo JA, Hereld D, Riley EP, Charness ME, Coles CD, Warren KR, Jones KL, Hoyme HE. Prevalence of Fetal Alcohol Spectrum Disorders in 4 US Communities. JAMA. 2018 Feb 6;319(5):474-482.
- ↑ Lupton C, Burd L, Harwood R. Cost of fetal alcohol spectrum disorders. Am J Med Genet C Semin Med Genet. 2004 May 15;127C(1):42-50. doi: 10.1002/ajmg.c.30015. PMID: 15095471.
- ↑ Jump up to: 12.0 12.1 12.2 12.3 Strömland K. Ocular abnormalities in the fetal alcohol syndrome. Acta Ophthalmologica Supplement 1985;171:1-50.
- ↑ Jump up to: 13.0 13.1 13.2 13.3 13.4 Strömland K. Ocular involvement in the fetal alcohol syndrome. Survey of ophthalmology 1987;31:277-84.
- ↑ Jump up to: 14.0 14.1 Strömland K, Pinazo-Durán MD. Ophthalmic involvement in the fetal alcohol syndrome: clinical and animal model studies. Alcohol and alcoholism 2002;37:2-8.
- ↑ Astley SJ, Clarren SK. A fetal alcohol syndrome screening tool. Alcoholism: Clinical and experimental research 1995;19:1565-71.
- ↑ Jump up to: 16.0 16.1 16.2 16.3 16.4 16.5 16.6 16.7 16.8 Abdelrahman A, Conn R. Eye abnormalities in fetal alcohol syndrome. The Ulster medical journal 2009;78:164.
- ↑ Ribeiro I, Vale P, Tenedorio P, Rodrigues P, Bilhoto M, Pereira H. Ocular manifestations in fetal alcohol syndrome. European journal of ophthalmology 2007;17:104-9.
- ↑ Manning MA, Hoyme HE. Fetal alcohol spectrum disorders: a practical clinical approach to diagnosis. Neuroscience & Biobehavioral Reviews 2007;31:230-8.
- ↑ Sokol RJ, Clarren SK. Guidelines for use of terminology describing the impact of prenatal alcohol on the offspring. Alcoholism: Clinical and Experimental Research 1989;13:597-8.
- ↑ Astley SJ, Clarren SK. Measuring the facial phenotype of individuals with prenatal alcohol exposure: correlations with brain dysfunction. Alcohol and Alcoholism 2001;36:147-59.
- ↑ Jump up to: 21.0 21.1 Hellström A, Chen Y, Strömland K. Fundus morphology assessed by digital image analysis in children with fetal alcohol syndrome. Journal of pediatric ophthalmology and strabismus 1997;34:17-23.
- ↑ Hug TE, Fitzgerald KM, Cibis GW. Clinical and electroretinographic findings in fetal alcohol syndrome. Journal of American Association for Pediatric Ophthalmology and Strabismus 2000;4:200-4.
- ↑ Jump up to: 23.0 23.1 23.2 23.3 Green CR, Munoz DP, Nikkel SM, Reynolds JN. Deficits in eye movement control in children with fetal alcohol spectrum disorders. Alcoholism: clinical and experimental research 2007;31:500-11.
- ↑ Jump up to: 24.0 24.1 Fetal Alcohol Syndrome - American Association for Pediatric Ophthalmology and Strabismus. Aapos.org https://aapos.org/glossary/fetal-alcohol-syndrome (2021).
- ↑ Jump up to: 25.0 25.1 O'Connor MJ, Frankel F, Paley B, et al. A controlled social skills training for children with fetal alcohol spectrum disorders. Journal of consulting and clinical psychology 2006;74:639.
- ↑ Jump up to: 26.0 26.1 Hoyme HE, Kalberg WO, Elliott AJ, et al. Updated clinical guidelines for diagnosing fetal alcohol spectrum disorders. Pediatrics 2016;138:e20154256.
- ↑ Jump up to: 27.0 27.1 Gyllencreutz, E. et al. Ophthalmologic Findings in Fetal Alcohol Spectrum Disorders – A Cohort Study From Childhood to Adulthood. American Journal of Ophthalmology 214, 14–20 (2020).
- ↑ Kable JA, Jones KL. Identifying Prenatal Alcohol Exposure and Children Affected by It: A Review of Biomarkers and Screening Tools. Alcohol Res. 2023 May 25;43(1):03.
- ↑ Strömland K, Hellström A. Fetal alcohol syndrome—an ophthalmological and socioeducational prospective study. Pediatrics 1996;97:845-50.
- ↑ Strömland K. Visual impairment and ocular abnormalities in children with fetal alcohol syndrome. Addiction biology 2004;9:153-7.
- ↑ Maurage P, Bollen Z, Masson N, D'Hondt F. A review of studies exploring fetal alcohol spectrum disorders through eye tracking measures. Prog Neuropsychopharmacol Biol Psychiatry. 2020 Dec 20;103:109980.
- ↑ Popova S, Lange S, Shield K, et al. Comorbidity of fetal alcohol spectrum disorder: a systematic review and meta-analysis. The Lancet 2016;387:978-87.
- ↑ Weyrauch D, Schwartz M, Hart B, Klug MG, Burd L. Comorbid mental disorders in fetal alcohol spectrum disorders: a systematic review. Journal of Developmental & Behavioral Pediatrics 2017;38:283-91.
- ↑ Roozen S, Ehrhart F. Fetal alcohol spectrum disorders and the risk of crime. Handb Clin Neurol. 2023;197:197-204.
- ↑ Jump up to: 35.0 35.1 Sharpe TT, Alexander M, Hutcherson J, et al. Report from the CDC. Physician and allied health professionals' training and fetal alcohol syndrome. Journal of Women's Health 2004;13:133-9.
- ↑ Vorgias D, Bernstein B. Fetal Alcohol Syndrome. 2021 Jul 26. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan–. PMID: 28846263.
- ↑ Chen SY, Kannan M. Neural crest cells and fetal alcohol spectrum disorders: Mechanisms and potential targets for prevention. Pharmacol Res. 2023 Aug;194:106855.
- ↑ Andreu-Fernández V, La Maida N, Marquina M, Mirahi A, García-Algar O, Pichini S, Minutillo A. Novel Interventions on Comorbidities in Patients with Fetal Alcohol Spectrum Disorder (FASD): An Integrative Review. Biomedicines. 2024 Feb 22;12(3):496.
- ↑ Leruste S, Doray B, Maillard T, Lebon C, Marimoutou C, Spodenkiewicz M. Scoping review on the role of the family doctor in the prevention and care of patients with foetal alcohol spectrum disorder. BMC Prim Care. 2024 Feb 22;25(1):66.
- ↑ Jones K. Successfully raising resilient foster children with fetal alcohol syndrome: What works. Envision: The Manitoba Journal of Child Welfare 2004;3:1-18.
- ↑ Rangmar J, Hjern A, Vinnerljung B, Strömland K, Aronson M, Fahlke C. Psychosocial outcomes of fetal alcohol syndrome in adulthood. Pediatrics 2015;135:e52-e8.
- ↑ Streissguth AP, Bookstein FL, Barr HM, Sampson PD, O'MALLEY K, Young JK. Risk factors for adverse life outcomes in fetal alcohol syndrome and fetal alcohol effects. Journal of Developmental & Behavioral Pediatrics 2004;25:228-38.
- ↑ Carpita B, Migli L, Chiarantini I, Battaglini S, Montalbano C, Carmassi C, Cremone IM, Dell'Osso L. Autism Spectrum Disorder and Fetal Alcohol Spectrum Disorder: A Literature Review. Brain Sci. 2022 Jun 16;12(6):792.
- ↑ Thanh NX, Jonsson E. Life expectancy of people with fetal alcohol syndrome. Journal of Population Therapeutics and Clinical Pharmacology 2016;23.