Dome-Shaped Macula
All content on Eyewiki is protected by copyright law and the Terms of Service. This content may not be reproduced, copied, or put into any artificial intelligence program, including large language and generative AI models, without permission from the Academy.
Disease Entity
Disease:
Dome-shaped macula (DSM) is characterized by a convex anterior protrusion (bowing towards the vitreous cavity) of the macula associated with high myopia and a posterior staphyloma.
Epidemiology
DSM has been shown to occur in 10.7-12% of highly myopic eyes in hospital-based patients.[1][2][3] The prevalence of DSM in the general population is currently unknown. However, DSM (especially unilateral) may be noted with hyperopia or emmetropia also.[4]
Risk Factors
DSM is associated with high myopia, and its presence is positively correlated with the severity of myopic maculopathy.[3] Though initially thought to only occur with high myopia, DSM has also been noted in mildly myopic and non-myopic eyes.[5][6] In such cases, the ultrasonogram may show an excavation at the posterior pole.
Pathophysiology
Several theories have been proposed, but the exact pathophysiology of DSM remains unclear. When DSM was first observed by Gaucher in 2008, it was believed to be due to either choroidal thickening, a the posterior eye-wall collapsing, or vitreomacular traction.[1][7] Subsequently, focal thickening of the subfoveal sclera has been shown to be a more likely mechanism, though the reason for the thickening is unknown.[8] A defect in Bruch’s membrane may also create a focal relaxation in the posterior sclera, allowing it to bulge anteriorly and form a dome.[9] Some speculate that the dome may compensate for the large axial length in high myopes, thus protecting against tractional damage to the fovea and distributing tractional forces more peripherally.[3]
Diagnosis
Optical Coherence Tomography (OCT) is necessary to diagnose DSM and identify the morphological type.[6] Because the convexity can appear in different orientations, it is important to obtain both vertical and horizontal scans or radial scanning to ensure visualization.[10] Radial scans are preferred to diagnose DSM.
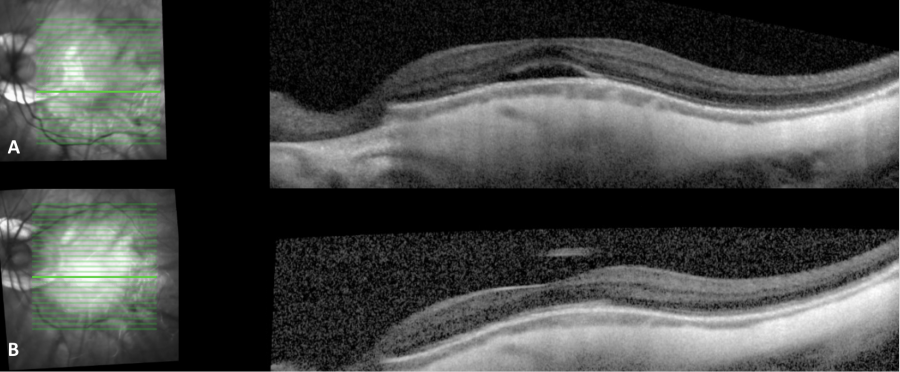
History
Patients with DSM are likely to have a history of high myopia and may experience worsening visual acuity or metamorphopsia.
Physical Exam
There is no specific abnormality in DSM that can be reliably visualized ophthalmoscopically in DSM.[10] Ophthalmoscopy findings that may raise suspicion for DSM include an oval-shaped area of macular pigment mottling, the appearance of a ridge bridging the fovea, and optic nerve, or a horizontally-oriented oval-shaped optic nerve. Such ridge passing through the fovea becomes more prominent stereoscopically when examined using an indirect ophthalmoscope and 20D lens.
Signs
Besides displaying an elevated macula on OCT, eyes with DSM may demonstrate pinpoint leakage on fluorescein angiography, a serous retinal detachment, retinal pigment epithelium elevations, a small pigment epithelial defect, or focal punctate hyperfluorescence with indocyanine green chorioangiography.[12]
Symptoms
Patients may experience a decrease in visual acuity or metamorphopsia as complications of associated serous foveal detachment or choroidal neovascularization.[13]
Clinical Diagnosis
DSM has been classified into 3 morphological types based on appearance with OCT:[6] [14]
1. Central Round Dome (21%)- DSM is evident on both horizontal and vertical OCT scan[15]
2. Horizontally Oriented Oval Shaped Dome (62%, most common type[6] [14])- vertical OCT scan shows DSM, but horizontal OCT scan is almost flat[15]
3. Vertically Oriented Oval Shaped Dome (17%)-horizontal OCT scan shows DSM, but vertical OCT scan is almost flat[15]
Differential Diagnosis
- Central serous chorioretinopathy
- Non-pigmented neoplasm of the choroid, such as choroidal hemangioma or amelanotic choroidal melanoma
- Bilateral diffuse uveal melanocytic proliferation (BDUMP)
- Uveal effusion syndrome
- Posterior scleritis
Management
General Treatment
DSM management focuses on reducing subretinal fluid (SRF), but no effective treatment for this complication has been established. Three monthly injections of aflibercept may improve best-corrected visual acuity (BCVA) and reduce central subfield thickness on OCT,[13] but bevacizumab and ranibizumab have proven ineffective at improving BCVA or subretinal fluid.[6][16][17] There are also limited reports of mineralocorticoid receptor antagonists successfully resolving serous foveal detachments.[18] Photodynamic therapy (PDT) trials for subretinal fluid associated with DSM have conflicted over the efficacy of this treatment.[6][19] Additionally, vitrectomy may aid in the transient resolution of sub-retinal detachment in DSM patients.[20] Due to the lack of a proven treatment, many physicians elect to observe asymptomatic or mildly symptomatic cases. Oftentimes the subretinal fluid resolves and recurs intermittently over time (Figure 1). A study[6] on 56 eyes with DSM noted that there was no significant improvement in BCVA or complete resolution of subretinal fluid with bevacizumab, ranibizumab, or PDT; and the authors concluded that DSM 'is often associated with chronic SRF, for which no effective treatment is current(ly) available'.
Complications
The most frequent complication of DSM is subretinal fluid, which may predispose to foveal serous retinal detachment (SRD).[6] The prevalence of SRD in DSM has been shown to vary widely, occurring in 2% to 67% of patients with DSM.[10] The cause of SRD in this context is a topic of debate. It is possible that scleral thickening under the dome obstructs choroidal fluid outflow, leading to a fluid collection.[8] Others have found that in eyes with DSM and SRD, the submacular choroid is abnormally thick for the amount of myopia, pointing to a mechanism similar to central serous chorioretinopathy.[21] The abrupt change in choroidal thickness in eyes with DSM may lead to retinal pigment epithelium dysfunction and SRD.[22] SRF in DSM has also been shown to be associated with higher macula dome height,[14][21] a lower degree of myopia,[6] and vertically-oriented oval shaped domes.[14][21] Besides structural factors, alterations in the mineralocorticoid pathway could also be involved.[18] Studies conflict over whether subretinal fluid actually results in a decrease in BCVA.[6][14][21]
Other complications of DSM include macular retinal atrophy,[1] lamellar and full-thickness macular holes, extrafoveal schisis,[3][23] and epiretinal membranes.
Choroidal neovascularization may occur in DSM,[24] but Zhao et. al did not find this complication more likely in DSM compared to high myopes without DSM.[3] Choroidal neovascularization (CNV) may not be a result of DSM, but associated with myopia itself.[25] CNV may be more common in DSM patients with older age and higher axial length.[15]
DSM with pigment epithelial detachment may have higher bulge height and thicker central sclera.[15]
On the other hand, some suggest that DSM may actually act as a protective factor against foveal schisis, macular holes, and choroidal neovascularization.[3] DSM may also prevent vision-threatening macular complications after cataract surgery in highly myopic eyes.[26]
Prognosis
In eyes with DSM, BCVA and central foveal thickness may remain stable for years.[6][27] Dome height and retinal pigment epithelium atrophy tend to increase over time, however,[27] and a dome height greater than 400 µm has been associated with subfoveal serous retinal detachment, larger size of retinal pigment epithelial atrophy, and decreased visual acuity.[28]
References
- ↑ 1.0 1.1 1.2 Gaucher D, Erginay A, Lecleire-Collet A, et al. Dome-shaped macula in eyes with myopic posterior staphyloma. Am J Ophthalmol. 2008;145(5):909-914.
- ↑ Chebil A, Ben Achour B, Chaker N, Jedidi L, Mghaieth F, El Matri L. [Choroidal thickness assessment with SD-OCT in high myopia with dome-shaped macula]. J Fr Ophtalmol. 2014;37(3):237-241.
- ↑ 3.0 3.1 3.2 3.3 3.4 3.5 Zhao X, Ding X, Lyu C, et al. Observational study of clinical characteristics of dome-shaped macula in Chinese Han with high myopia at Zhongshan Ophthalmic Centre. BMJ Open. 2018;8(12):e021887.
- ↑ Naresh Babu Kannan, Sagnik Sen, Prithviraj Udaya, Obuli Ramachandran, Kim Ramasamy, "Spectral-Domain Optical Coherence Tomography-Based Morphofunctional Characterization of Dome-Shaped Maculopathy in Indian Population", Journal of Ophthalmology, vol. 2020, Article ID 8869455, 7 pages, 2020. https://doi.org/10.1155/2020/8869455
- ↑ Errera M-H, Michaelides M, Keane PA, et al. The extended clinical phenotype of dome-shaped macula. Graefes Arch Clin Exp Ophthalmol. 2014;252(3):499-508.
- ↑ 6.00 6.01 6.02 6.03 6.04 6.05 6.06 6.07 6.08 6.09 6.10 Lorenzo D, Arias L, Choudhry N, et al. Dome-shaped macula in myopic eyes: twelve-month follow-up. Retina. 2017;37(4):680-686.
- ↑ Mehdizadeh M, Nowroozzadeh MH. Dome-shaped macula in eyes with myopic posterior staphyloma. Am J Ophthalmol. 2008;146(3):478; author reply 478-479.
- ↑ 8.0 8.1 Imamura Y, Iida T, Maruko I, Zweifel SA, Spaide RF. Enhanced depth imaging optical coherence tomography of the sclera in dome-shaped macula. Am J Ophthalmol. 2011;151(2):297-302.
- ↑ Fang Y, Jonas JB, Yokoi T, Cao K, Shinohara K, Ohno-Matsui K. Macular Bruch’s membrane defect and dome-shaped macula in high myopia. PLoS One. 2017;12(6):e0178998.
- ↑ 10.0 10.1 10.2 Ohno-Matsui K, Fang Y, Shinohara K, Takahashi H, Uramoto K, Yokoi T. Imaging of Pathologic Myopia. Asia Pac J Ophthalmol (Phila). March 2019. doi:10.22608/APO.2018494
- ↑ Image courtesy of Danny A. Mammo MD
- ↑ Sahoo NK, Singh SR, Rajendran A, Shukla D, Chhablani J. Masqueraders of central serous chorioretinopathy. Survey of Ophthalmology. 2019;64(1):30-44. doi:10.1016/j.survophthal.2018.09.001
- ↑ 13.0 13.1 Giacomelli G, Mencucci R, Sodi A, et al. Aflibercept in Serous Foveal Detachment in Dome-Shaped Macula: Short-Term Results in a Retrospective Study. Ophthalmic Surg Lasers Imaging Retina. 2017;48(10):822-828.
- ↑ 14.0 14.1 14.2 14.3 14.4 Caillaux V, Gaucher D, Gualino V, Massin P, Tadayoni R, Gaudric A. Morphologic characterization of dome-shaped macula in myopic eyes with serous macular detachment. Am J Ophthalmol. 2013;156(5):958-967.e1.
- ↑ 15.0 15.1 15.2 15.3 15.4 Ohsugi H, Ikuno Y, Oshima K, Yamauchi T, Tabuchi H. Morphologic characteristics of macular complications of a dome-shaped macula determined by swept-source optical coherence tomography. Am J Ophthalmol. 2014 Jul;158(1):162-170.e1. doi: 10.1016/j.ajo.2014.02.054. Epub 2014 Mar 12. PMID: 24631474.
- ↑ Chinskey ND, Johnson MW. Treatment of Subretinal Fluid Associated With Dome-Shaped Macula. Ophthalmic Surgery, Lasers and Imaging Retina. 2013;44(6):593-595. doi:10.3928/23258160-20131010-01
- ↑ Tamura N, Sakai T, Tsuneoka H. Spontaneous resolution of foveal detachment in dome-shaped macula observed by spectral domain optical coherence tomography. Clin Ophthalmol. 2014;8:83-86.
- ↑ 18.0 18.1 Dirani A, Matet A, Beydoun T, Mantel I, Behar-Cohen F. Resolution of foveal detachment in dome-shaped macula after treatment by spironolactone: report of two cases and mini-review of the literature. Clin Ophthalmol. 2014;8:999-1002.
- ↑ Arapi I, Neri P, Mariotti C, et al. Considering photodynamic therapy as a therapeutic modality in selected cases of dome-shaped macula complicated by foveal serous retinal detachment. Ophthalmic Surg Lasers Imaging Retina. 2015;46(2):217-223.
- ↑ Soudier G, Gaudric A, Gualino V, Nardin M, Speeg-Schatz C, Gaucher D. Epiretinal Membrane in Dome-Shaped Macula Complicated with Serous Retinal Detachment: Transient Efficacy of Surgery. Case Rep Ophthalmol. 2017;8(3):515-520.
- ↑ 21.0 21.1 21.2 21.3 Viola F, Dell’Arti L, Benatti E, et al. Choroidal Findings in Dome-Shaped Macula in Highly Myopic Eyes: A Longitudinal Study. American Journal of Ophthalmology. 2015;159(1):44-52. doi:10.1016/j.ajo.2014.09.026
- ↑ Tan ACS, Yzer S, Freund KB, Dansingani KK, Phasukkijwatana N, Sarraf D. Choroidal changes associated with serous macular detachment in eyes with staphyloma, dome-shaped macula or tilted disk syndrome. Retina. 2017;37(8):1544-1554.
- ↑ García-Ben A, Garcia-Basterra I, González-Gómez A, et al. Comparison of long-term clinical evolution in highly myopic eyes with vertical oval-shaped dome with or without untreated serous retinal detachment. Br J Ophthalmol. 2019;103(3):385-389.
- ↑ Marchese A, Arrigo A, Sacconi R, et al. Spectrum of choroidal neovascularisation associated with dome-shaped macula. Br J Ophthalmol. October 2018. doi:10.1136/bjophthalmol-2018-312780
- ↑ Lee JH, Lee SC, Choi S, Koh HJ, Kim SS, Lee CS. Two-year outcomes of intravitreal bevacizumab for choroidal neovascularization associated with a dome-shaped macula in pathologic myopia. Eye . 2017;31(3):507-508.
- ↑ Zhu X, He W, Zhang S, Rong X, Fan Q, Lu Y. Dome-shaped macula: a potential protective factor for visual acuity after cataract surgery in patients with high myopia. British Journal of Ophthalmology. 2019:bjophthalmol - 2018. doi:10.1136/bjophthalmol-2018-313279
- ↑ 27.0 27.1 Soudier G, Gaudric A, Gualino V, et al. Long-term evolution of dome-shaped macula: increased macular bulge is associated with extended macular atrophy. Retina. 2016;36(5):944-952.
- ↑ Sánchez JF, Fajardo Sánchez J, Chau Ramos CE, Roca Fernández JA, Urcelay Segura JL. Clinical, fundoscopic, tomographic and angiographic characteristics of dome shaped macula classified by bulge height. Archivos de la Sociedad Española de Oftalmología (English Edition). 2017;92(10):458-463. doi:10.1016/j.oftale.2017.07.001

