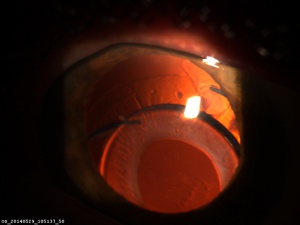
Dead Bag Syndrome
All content on Eyewiki is protected by copyright law and the Terms of Service. This content may not be reproduced, copied, or put into any artificial intelligence program, including large language and generative AI models, without permission from the Academy.
Disease
Dead Bag Syndrome, first described by Samuel Masket MD, is the late dislocation of an intraocular lens (IOL) in a capsule that has remained clear after surgery (i.e. without signs of fibrosis or proliferative change) but has become diaphanous and floppy. Specifically, it can be defined as loss of all lens epithelial cells (LEC) after cataract surgery, leading to failure of the IOL to remain in optical axis.[1][2] In cataract surgery, a new IOL is placed in the eye to replace the patient’s clouded lens. IOLs rely on remnant LECs to secure their position in the eye after cataract surgery. Loss of LECs result in dead bag syndrome.[1] The exact etiology from which dead bag syndrome arises is still under investigation. Current hypothesized etiologies include capsule degradation/delamination in areas of cellular attachment leading to dislocation.[3]
It is distinct from true exfoliation syndrome, which has splitting and delamination of the anterior capsule, and pseudoexfoliation syndrome, which has deposition of fibrillary material in the anterior segment.[4] It is diagnosed through visualizing the thin membrane of a delaminated capsule on the anterior surface of the crystalline lens, or more commonly seen on slit lamp exam before cataract extraction with implantation of IOL in the anterior chamber. The difference between dead bag and true exfoliation syndrome is based on the age group and exposure to infrared radiation or high heat, where younger age patients and those not exposed to radiation are at higher risk for dead bag syndrome.[4][5]
Risk Factors/Causative Events
Risk factors of Dead Bag Syndrome include:
- Zonular weakening that may not have been seen at the time of the surgery, but was found later.[6]
- This differs from true exfoliation as no zonular weakening found with that.[6]
The use of mechanical or chemical methods to destroy LECs in order to eliminate PCO.[7]
Pathophysiology
Disruption of the blood-aqueous-barrier during cataract surgery triggers an immune response in the lens epithelial cells to undergo epithelial-mesenchymal transition, resulting in migration, proliferation, and ultimately posterior capsule opacification (PCO). There are two types of PCO caused by two types of cells. Anterior epithelial cells residing in the central zone of the anterior capsule convert to myofibroblasts and migrate to the posterior capsule, leading to fibrous metaplasia. In contrast, the pluripotent cells around the capsule equator also migrate to the posterior capsule but instead form large, balloon-shaped cells (bladder cells).[8]
Dead Bag Syndrome is unique in that there is no evidence of fibrosis or opacification caused by lens epithelial cells. Microscopic examination of capsules with Dead Bag Syndrome shows little to no lens epithelial cells. Therefore, it is hypothesized that Dead Bag Syndrome is caused by an absence or insufficient amount of lens epithelial cells, possibly from prior capsular damage (i.e. excessive capsular pressure in an intumescent cataract) or from removal of lens epithelial cells by cleaning/polishing the capsule during cataract surgery.[4]
Histological examination of dead bag syndrome shows:
- Capsular thinning and/or splitting
- LECs that are either completely absent, or had only rare LECs on inner capsular surface
- IOL may show small amount of granular pigment deposition, but IOL also may appear unremarkable
No distinct secondary proliferation of LEC or fibrotic changes.[4]
Complications
The main complication of Dead Bag Syndrome is lens dislocation, which can result in decreased visual acuity. Dislocations can also cause retinal detachment, bleeding, inflammation, and macular or corneal edema.[9]
Management
If IOL subluxation occurs, it should be monitored/observed for worsening dislocation and visual acuity.
If IOL dislocation occurs, it should be monitored/observed by the physician. If necessary, it can be surgically managed in which a vitrectomy is performed first in order to prevent pulling on the retina when manipulating the IOL. Then based on the lens type and eye anatomy, the dislocation can be fixed in two ways: IOL rescue/repositioning or an IOL exchange. In IOL rescue/repositioning, the dislocated lens is preserved and is moved to a more stable location, pending quality of the lens. In IOL exchange, the old lens is removed and replaced by new IOL.[9]. Many techniques are available including a Yamane-like technique.
Research
Dr. Culp et al. describe in a case series (n=10) the clinical and histopathological findings of dead bag syndrome. The study found no secondary proliferation of lens epithelial cells or fibrosis on microscopic examination of the capsular bag but did find signs of capsular degradation such as thinning and splitting. Zonular weakness was also noted and found to be linked to in-the-bag IOL dislocation.[4]
Additional Resources
Four minute video interview with author Dr. Liliana Werner MD PhD
https://www.aao.org/interview/histopathologic-findings-in-dead-bag-syndrome
Commentary by Dr. Ehud Assia MD and Dr. Amar Agarwal MD
https://www.healio.com/news/ophthalmology/20220303/surgeons-report-new-entity-of-dead-bag-syndrome
Written interview of author Dr. Liliana Werner MD PhD
https://www.eyeworld.org/2022/what-you-need-to-know-about-dead-bag-syndrome
Two minute interview with author Dr. Nicole Fram MD
https://eyetube.net/series/clinical-minute/clinical-minute-february-2022-video
Dead Bag IOL exchange by Dr. Tom Oetting MD
https://www.youtube.com/watch?v=qNKum5niHUk
- ↑ Jump up to: 1.0 1.1 Shihan MH, Novo SG, Duncan MK. Cataract surgeon viewpoints on the need for novel preventative anti-inflammatory and anti-posterior capsular opacification therapies. Current Medical Research and Opinion. 2019; 35(11): 1971-1981
- ↑ Spalton DH, Russell SL, Evans-Gowing R, Eldred, JA, Wormstone M. Effect of total lens epithelial cell destruction on intraocular lens fixation in the human capsular bag. Journal of Cataract & Refractive Surgery. 2014;40(2): 306-312.
- ↑ Werner, L., 2021. Histopathologic Findings in Dead Bag Syndrome. American Academy of Ophthalmology; 2021. Available at: https://www.aao.org/interview/histopathologic-findings-in-dead-bag-syndrome.
- ↑ Jump up to: 4.0 4.1 4.2 4.3 4.4 Culp, Catherine MD; Qu, Phillip MD; Jones, Jason MD; Fram, Nicole MD; Ogawa, Gregory MD; Masket, Samuel MD; Mamalis, Nick MD; Werner, Liliana MD, PhD Clinical and histopathological findings in the dead bag syndrome, Journal of Cataract & Refractive Surgery: February 2022 - Volume 48 - Issue 2 - p 177-184 doi: 10.1097/j.jcrs.0000000000000742
- ↑ Teekhasaenee C. Current Concepts in True Exfoliation Syndrome. J Glaucoma. 2018; 27(7):S105-S110.
- ↑ Jump up to: 6.0 6.1 Wong AL, Chan TC, Fong AH, Lam BN, Yuen HK. Clinical characteristics and surgical outcomes of phacoemulsification in true exfoliation syndrome. J Cataract Refract Surg. 2014;40(1):82-6.
- ↑ Sabbagh L. PCO: What’s wrong with doing a YAG. Review of Ophthalmology. https://www.reviewofophthalmology.com/article/pco-whats-wrong-with-doing-a-yag.
- ↑ Konopińska J, Młynarczyk M, Dmuchowska DA, Obuchowska I. Posterior Capsule Opacification: A Review of Experimental Studies. J Clin Med. 2021;10(13):2847. Published 2021 Jun 27. doi:10.3390/jcm10132847
- ↑ Jump up to: 9.0 9.1 Bakri, SJ, Berrocal A, Capone A, et al. Intraocular Lens Dislocation. Retina Health Series. https://www.asrs.org/patients/retinal-diseases/27/intraocular-lens-dislocation.