Alpha Gal Syndrome
All content on Eyewiki is protected by copyright law and the Terms of Service. This content may not be reproduced, copied, or put into any artificial intelligence program, including large language and generative AI models, without permission from the Academy.
Disease Entity
Alpha-gal syndrome (AGS) is an IgE-mediated hypersensitivity response to carbohydrate galactose-α-1,3-galactose (alpha-gal) epitope, a sugar molecule found in on the glycoproteins/glycolipids of nonprimate mammals. It includes both a drug-induced immediate hypersensitivity response to injected pharmaceuticals and a delayed reaction in response to consumption of mammalian-derived products, most commonly red meat. .[1][2] [3][4][5]
Etiology
Alpha-gal syndrome is believed to be a tick-mediated sensitization to the alpha-gal epitope.[1][2][3] More than 10 species of tick across six continents have been indicated in the development of the allergy. Although initially believed to be an sIgE response solely induced by a tick bite after a blood meal, it has now been shown that some tick species express alpha-gal in its unfed and fed salivary glands. Therefore, regions with high tick populations are at greater risk. [2][6][7]
Pathophysiology
Although alpha-gal syndrome refers to a spectrum of hypersensitivity reactions mediated by the epitope "alpha-gal", its main vector of introduction is believed to be through tick bites. Alpha-gal is a nearly ubiquitous epitope found in glycoproteins and glycolipids of nonprimate mammals. The initial belief was, that after a mammalian blood meal, a tick may introduce the alpha-gal epitope into human circulation triggering an anti-α-gal sIgE response. Then, upon consumption of red meat, a person would develop an allergic reaction of variable severity. However, more recently, it has been shown that ticks may express alpha-gal even unfed in their salivary glands. In both cases, the interaction of alpha-gal with antigen-presenting B cells triggers the immune cascade with proliferation of sIgE producing cells.[2][8][9]
Allergic reactions are most common after sensitization and ingestion of red meat, however cases have been shown after exposure to certain medications (i.e. Cetuximab) and animal-derived gelatin products.[10]
Diagnosis
History
Often patients will describe a known history of tick bite or tick exposure with recurrent symptomology after consuming red meat. They may endorse worsening symptoms in the evening, after having eaten meat at lunch or dinner. Patients may also report increased symptom severity with alcohol consumption, NSAID use or physical exertion.[10][11][12]
Symptoms
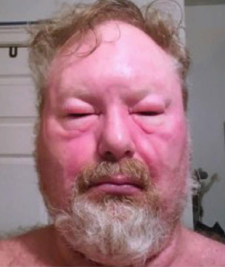
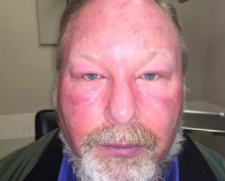
Most common symptoms in AGS include urticaria, facial angioedema and pruritis in 80-90% of of individuals. Anaphylaxis rates have been shown to be as high as 60%, in some studies. GI symptoms, such as nausea, vomiting and diarrhea are also fairly common, presenting in about 2/3rds of patients with AGS.[4][5][10][12]
Laboratory test
When there is a high clinical suspicion of AGS, diagnosis may be confirmed with a serum alpha-gal IgE test. A positive test is considered when the alpha-gal IgE value is either ≥0.1 IU/mL or ≥2% of total IgE. Skin prick testing and intradermal testing have been shown to to be less reliable and are not the preferred testing method.[10][11][13][14]
Differential diagnosis
- Other allergy (i.e. cow's milk allergy, cat pork syndrome)
- Autoimmune disease
- Insect bite
- Medication reaction
- Chronic urticaria
- Hereditary angioedema
- Morbihan Disease
Management
The mainstay of treatment is the avoidance of mammalian meat. As reaction severity cannot be accurately predicted based on amount of meat consumed or frequency of meat consumption, it is generally accepted that total avoidance is indicated.[15] The degree to which the meat is cooked seems to be unrelated to symptom severity. A small percentage of patients may need to additionally avoid dairy and/or gelatin products.[7][10][16] Depending on the individual's response, either antihistamines or an EpiPen should be available for possible reactions.[10]
Prognosis
In one study, a small percentage of patients that refrained from meat consumption were later able to consume meat without an allergic reaction. Desensitization studies are currently underway.[17][18]
References
- ↑ Jump up to: 1.0 1.1 Chung CH, Mirakhur B, Chan E, et al. Cetuximab-induced anaphylaxis and IgE specific for galactose-alpha-1,3-galactose. N Engl J Med 2008;358:1109–1117.
- ↑ Jump up to: 2.0 2.1 2.2 2.3 Krzyszof R, Wagner A, Rutkowski R, et al. Alpha-gal syndrome: An emerging cause of food and drug allergy. Clin Exp Allergy 2020;50:894-903.
- ↑ Jump up to: 3.0 3.1 O’Neil BH, Allen R, Spigel DR, et al. High incidence of cetuximab related infusion reactions in Tennessee and North Carolina and the association with atopic history. J Clin Oncol 2007;25:3644–3648.
- ↑ Jump up to: 4.0 4.1 Commins SP, Satinover SM, Hosen J, et al. Delayed anaphylaxis, angioedema, or urticaria after consumption of red meat in patients with IgE antibodies specific for galactose-alpha-1,3-galactose. J Allergy Clin Immunol 2009;123:426–433.
- ↑ Jump up to: 5.0 5.1 Platts-Mills TAE, Li RC, Keshavarz B, Smith AR, Wilson JM. Diagnosis and management of patients with the α-gal syndrome. J Allergy Clin Immunol Pract 2020;8:15-23.
- ↑ Van Nunen SA, O’Connor KS, Clarke LR, et al. An association between tick bite reactions and red meat allergy in humans. Med J Aust 2009;190:510–511. 5
- ↑ Jump up to: 7.0 7.1 Patel C, Iweala OI. ‘Doc, will I ever eat steak again?’: diagnosis and management of alpha-gal syndrome. Curr Opin Pediatr 2020;32:816–824.
- ↑ Commins SP, James HR, Kelly LA, et al. The relevance of tick bites to the production of IgE antibodies to the mammalian oligosaccharide galactose-alpha-1,3-galactose. J Allergy Clin Immunol 2011;127:1286.e6–1293.e6.
- ↑ Cabezas-Cruz A, Hodžić A, Román-Carrasco P, et al. Environmental and molecular drivers of the α-Gal syndrome. Front Immunol 2019;10:1210.
- ↑ Jump up to: 10.0 10.1 10.2 10.3 10.4 10.5 Commins SP. Diagnosis & management of alpha-gal syndrome: lessons from 2,500 patients. Expert Rev Clin Immunol 2020;16:667–677.
- ↑ Jump up to: 11.0 11.1 Mabelane T, Basera W, Botha M, et al. Predictive values of alpha-gal IgE levels and alpha-gal IgE: Total IgE ratio and oral food challenge-proven meat allergy in a population with a high prevalence of reported red meat allergy. Pediatr Allergy Immunol 2018;29:841–849.
- ↑ Jump up to: 12.0 12.1 Wilson JM, Schuyler AJ, Workman L, et al. Investigation into the α-Gal syndrome: characteristics of 261 children and adults reporting red meat allergy. J Allergy Clin Immunol Pract 2019;7:2348– 2358.e4.
- ↑ Crispell G, Commins SP, Archer-Hartman SA, et al. Discovery of alpha-gal-containing antigens in North American tick species believed to induce red meat allergy. Front Immunol 2019;10:1056.
- ↑ Sharma SR, Crispell G, Mohamed A, et al. Alpha-gal syndrome: involvement of Amblyomma americanum α-D-Galactosidase and β-1,4 galactosyltransferase enzymes in α-Gal metabolism. Front Cell Infect Microbiol 2021;11:775371.
- ↑ Iweala OI, Nagler CR. The microbiome and food allergy. Annu Rev Immunol 2019;37:377–403.
- ↑ Kim MS, Straesser MD, Keshavarz B, et al. IgE to galactose-alpha1,3-galactose wanes over time in patients who avoid tick bites. J Allergy Clin Immunol Pract 2019; 8:364.e2–367.e2.
- ↑ Kim MS, Straesser MD, Keshavarz B, et al. IgE to galactose-alpha1,3-galactose wanes over time in patients who avoid tick bites. J Allergy Clin Immunol Pract 2019; 8:364.e2–367.e2.
- ↑ Pattanaik D, Lieberman P, Lieberman J, et al. The changing face of anaphylaxis in adults and adolescents. Ann Allergy Asthma Immunol 2018;121:594–597.