Ophthalmic Images in Diverse Patient Populations: Difference between revisions
m (→update images) |
|||
| Line 77: | Line 77: | ||
== Conjunctival melanoma == | == Conjunctival melanoma == | ||
<gallery widths="200" heights="200"> | <gallery widths="200" heights="200"> | ||
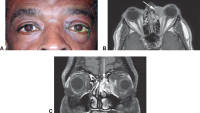
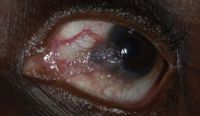
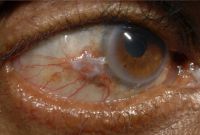
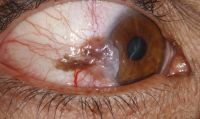
File: | File:Photographs showing conjunctival melanoma in various races.jpg|Photographs showing conjunctival melanoma in various races. A, White man with (B) conjunctival melanoma resulting from nevus. C, African American woman with (D) conjunctival melanoma from primary acquired melanosis. E, Hispanic woman with (F) conjunctival melanoma de novo. | ||
</gallery> | </gallery> | ||
Revision as of 09:38, May 8, 2023
All content on Eyewiki is protected by copyright law and the Terms of Service. This content may not be reproduced, copied, or put into any artificial intelligence program, including large language and generative AI models, without permission from the Academy.
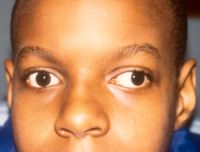
Currently, a disproportionate number of textbook figures and photographs are of eye conditions in white patients. Many ocular conditions can appear differently in individuals of color or those with darker skin. The purpose of this page is to share images of both common and rare pathology of the external, anterior, and posterior segments in patients of color. The American Academy of Ophthalmology's Committee for Resident Education’s DEI workgroup initiated this image collection to serve as a source for education and future versions of the Basic and Clinical Science Course (BCSC) and other texts.
Visit the Academy website to learn more about its commitment to diversity, equity, and inclusion in the ophthalmic community and review educational resources related to DEI in ophthalmology.
A-C
Acanthamoeba keratitis
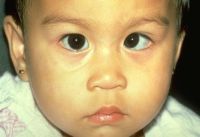
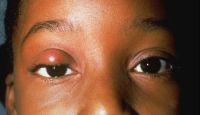
Amblyopia
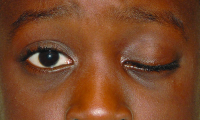
Amblyogenic ptosis
Aniridia-associated keratopathy and nystagmus
Arlt's line
Asteroid hyalosis
Bacterial orbital cellulitis with proptosis
Bardet-biedl syndrome
Basal cell carcinoma (eyelid)
Chalazion
Conjunctival melanoma
Conjunctival nevus
Corneal arcus
CRAO (dark choroid)
D-F
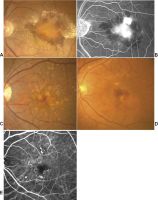
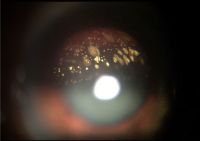
Diabetic retinopathy
Figure 1. Color fundus photograph of the left eye in case 1 in 1995 showing lipid exudates (arrow), cotton wool spots, and intraretinal hemorrhages of diabetic retinopathy as well as multiple refractile intraretinal crystals (arrowhead). Figure 2. Color fundus photograph of the left eye in case 1 in 2001 after focal photocoagulation for diabetic macular edema. The edema has completely resolved, and there are fewer intraretinal crystals, which are arranged in a pattern different from that in 1995. Figure 3. Color fundus photograph of the right eye in case 2 showing a frond of retinal neovascularization and many iridescent intraretinal crystals within the foveal avascular zone. Figure 4. Mid-phase fluorescein angiogram of the right eye in case 2 showing the perfused retinal neovascularization and the absence of any fluorescein angiographic sign of the crystals. Figure 5. Color fundus photograph of the right eye in case 2 one year after panretinal laser photocoagulation. Most of the crystals have resolved. Figure 6. Color fundus photograph of the right eye in case 3. The distribution of the intraretinal crystals follows the pattern of the distribution of intraretinal lipid from diabetic macular edema. The diabetic lipid exudates (arrow) can be distinguished from the refractile crystals (arrowhead).
Episcleral vessels
Exotropia
G-I
Hurler's syndrome
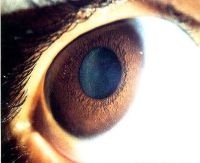
Iris melanoma
Iris nevus
J-L
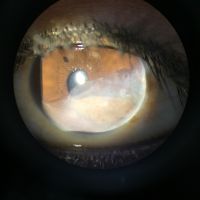
Lens-induced glaucoma
M-O
Melanoma (conjunctiva)
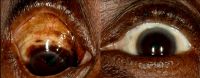
Metastatic carcinoma
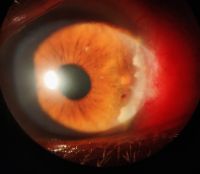
A 37-year-old presented with ocular metastasis with primary ductal carcinoma of the left breast. The case presented with complaints of redness and pain OS for 1 month, and there was a past history of a left modified radical mastectomy 3 years previously at the same institution where the patient didn’t complete the chemotherapy. On examination, OD-within normal limits, OS lids appeared edematous, circumcorneal congestion with prominent episcleral vessels seen, anterior chamber had exudative deposits and 1+ grade of cellular activity present, iris was atrophied from 3’o-5’o clock hours.
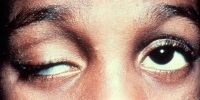
Molluscum contagiosum
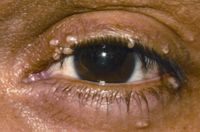
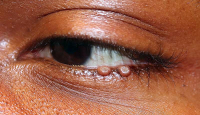
Giant eyelid molluscum contagiosum in a child with AIDS. A 6-year-old boy presented with a 3-month history of multiple, pedunculated, nodules with a central umbilication (Fig 1A). A clinical diagnosis of molluscum contagiosum was made and investigations revealed HIV infection with a CD4 count of 124/ml3. Highly active antiretroviral therapy (HAART) was initiated. The larger lesions were excised (Fig 1B). Characteristic eosinophilic intracytoplasmic inclusion bodies were seen on histopathologic examination (Fig 1C; hematoxylin-eosin 40). The child is currently on maintenance therapy with HAART with no recurrence of the lesions.
Neovascular glaucoma
Nevus of ota (eyelids)
Overaction of left inferior oblique
P-R
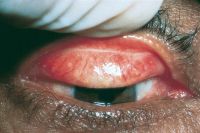
Papillary conjunctivitis
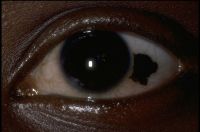
Primary acquired melanosis (PAM)
Pterygium
Congenital ptosis
S-Z
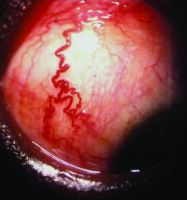
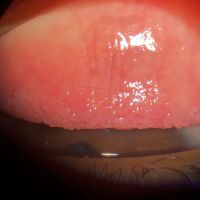
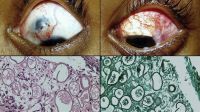
Scleromalacia perforans
Scleromalacia Perforans from Long-Standing Bulbar Conjunctival Rhinosporidiosis. A 12-year-old child presented with a 6-month old painless, reddish-blue swelling superior to the upper limbus (Fig 1A). Scleral thinning with uveal show and a conjunctival mass with dot-like, yellowish-white surface excrescences were noted. Excision with a donor scleral patch graft was performed (Fig 1B). Histopathology showed partially separated squamous metaplastic epithelium(Fig 1CeD,), edematous stroma, and numerous thick walled sporangia indicating rhinosporidiosis. Several of these appeared degenerated and empty. Others showed granular debris material (Fig 1C, Hematoxylin-Eosin; Fig 1D, Gomori’s MethenamineSilver 400). Ocular rhinosporidiosis most commonly involves the tarsal conjunctiva. Scleral melt from bulbar conjunctival rhinosporidiosis is known but extremely rare.